GLP-1 in Massachusetts: How to Get It, What It Really Costs, and the Best Path in 2026
Bottom Line
Yes, you can still get GLP-1 in Massachusetts in 2026 — even after the insurance cuts that left tens of thousands of MA residents scrambling. If you still have any shot at insurance coverage, Ro is the strongest online path because it handles FDA-approved medications and fights for prior authorization on your behalf (membership starts at $39, medication billed separately starting at $149/mo for the Wegovy pill). Source: Ro pricing page, verified April 2026.
If insurance is already gone, Eden Health is where we'd start — $149 first month, $249 ongoing for compounded semaglutide when prescribed. Source: Eden program page, verified April 2026.
| Your Situation | Best Path | Type | From | Best For |
|---|---|---|---|---|
| Still might have coverage | Ro | FDA-approved | $39/mo memb + $149 med | Large-employer or diabetes indication |
| Coverage gone | Eden Health | Compounded (prescribed) | $149 first month | Transparent cash-pay pricing |
| Brand-name, no insurance | Ro or LillyDirect | FDA-approved | $149–$299/mo + memb | Brand-name only preference |
| On Medicare | Medicare GLP-1 Bridge | FDA-approved (Wegovy, Foundayo, Zepbound KwikPen) | $50/mo copay | Medicare Part D, starts Jul 2026 |
| Want in-person care | Local obesity clinic / PCP | Usually FDA-approved | Higher total cost | Existing physician relationship |

What Happened to GLP-1 Coverage in Massachusetts?
Almost every major Massachusetts insurer dropped or restricted GLP-1 coverage for weight loss in 2026. If you got a surprise letter, a shocking pharmacy bill, or heard about the changes on the news — you're not imagining it. This affects hundreds of thousands of people across the state.
Here's exactly who changed what, when, and what options remain.
Massachusetts GLP-1 Insurance Coverage Tracker (April 2026)
| Insurer / Plan | Weight-Loss GLP-1? | Diabetes GLP-1? | Large Employer? | Effective | Source |
|---|---|---|---|---|---|
| Blue Cross Blue Shield of MA | ❌ Excluded on renewal | ✅ Yes (prior auth) | Yes — 100+ employees can add | Jan 1, 2026 | BCBS MA FAQ |
| Point32Health (Harvard Pilgrim / Tufts) | ❌ Excluded | ✅ Yes | Some large groups may buy up to Premium formulary | Jan 1, 2026 or plan anniversary | Point32Health notice |
| Mass General Brigham Health Plan | ❌ Excluded (fully insured commercial) | ✅ Yes (prior auth) | Yes — 50+ enrolled subscribers | Jan 1, 2026 (small); renewal (large) | MGB HP notice |
| WellSense (MA Clarity Plans) | ❌ Excluded | ✅ Yes | N/A | Jan 1, 2026 | WellSense prescriptions |
| Health New England | ❌ Excluded (individual / small group; <100 subscribers) | ✅ Yes | Yes — 100+ actively enrolled subscribers | Jan 1, 2026 (individual/small); renewal (large) | HNE GLP-1 page |
| Health Connector (Marketplace) | ❌ All carriers dropped for 2026 | ✅ Yes | N/A | 2026 plan year | MA Health Connector |
| GIC (State Employees) | ❌ Voted to drop (10–7) | ✅ Yes | N/A | July 2026 plan year | GBH News, Feb 26, 2026 |
| MassHealth (Medicaid) | ❌ Wegovy/Saxenda dropped Jan 2025; more July 1, 2026 | ✅ Yes | N/A | Phased: Jan 2025 + Jul 1, 2026 | MassHealth notice |
| Medicare | ⚡ NEW: $50/mo via GLP-1 Bridge (Jul–Dec 2026) | ✅ Yes (Part D) | N/A | July 1, 2026 | CMS GLP-1 Bridge |
The numbers behind this
One thing to check right now
If you're on Medicare — good news
The silver lining
How Much Does GLP-1 Actually Cost in Massachusetts Without Insurance?
The sticker shock is the thing that sends most people back to searching. So let's kill it fast. Brand-name retail prices — what you'd pay walking into CVS with no coverage — are brutal. But almost nobody needs to pay retail.
| Path | Medication | Month 1 | Ongoing Monthly | Annual Est. | Source |
|---|---|---|---|---|---|
| Brand-name retail (no coverage) | Wegovy pen | ~$1,300 | ~$1,300 | ~$15,600 | Retail pharmacy |
| Brand-name retail (no coverage) | Zepbound | ~$1,060 | ~$1,060 | ~$12,720 | Retail pharmacy |
| Ro (FDA-approved, cash-pay) | Wegovy pill | $39 memb + $149 med | $149 memb + $199–299 | ~$4,200–5,300 | Ro pricing |
| Ro (FDA-approved, cash-pay) | Wegovy pen | $39 memb + $199 med | $149 memb + $199–349 | ~$4,200–5,900 | Ro pricing |
| LillyDirect (FDA-approved) | Zepbound KwikPen | $299 | $299–449 | ~$3,588–5,388 | LillyDirect |
| Medicare GLP-1 Bridge | Wegovy or Zepbound | $50 copay | $50 copay | $300 (6 months) | CMS.gov |
| Eden Health (compounded) | Semaglutide | $149 | $249 | ~$2,890 | Eden program |
| MEDVi (compounded) | Semaglutide | $179 | $299 | ~$3,470 | MEDVi pricing |
Ro membership ($39 first month, $149/mo ongoing) billed separately from medication. Compounded medication prices are provider-stated and verified from provider websites April 2026. "Compounded" means prepared by a compounding pharmacy based on a physician's prescription — these are not FDA-approved as finished products.
Yes, you can use your HSA or FSA
The math is on your side.
The difference between $1,300/month retail and $149/month through a legitimate cash-pay provider is over $13,000 a year. That's the gap this page exists to close.
Which GLP-1 Path Fits Your Situation?
You don't need more information. You need sorting. Find yourself below.
"Still might have coverage"
Your best first move is Ro. They center FDA-approved medications and fight for prior authorizations. If your employer opted in, or if you have a diabetes indication, this path saves the most money.
Jump to: Insurance-first path with Ro →"Insurance dropped coverage"
Eden Health is where we'd start. $149 first month, $249 ongoing for compounded semaglutide when prescribed. No hidden membership fees. Straightforward cancellation.
Jump to: Cash-pay with Eden Health →"On Medicare"
You may be in luck. The Medicare GLP-1 Bridge launches July 1, 2026 — Wegovy and Zepbound for $50/month. Talk to your doctor now about getting your prior authorization ready.
Jump to: Medicare section →"State employee losing GIC coverage"
Your GIC coverage for weight-loss GLP-1 ends July 2026. All the cash-pay telehealth options in this guide work for you. If you have an HSA, use it.
See cash-pay options →On MassHealth and worried about losing coverage?
MassHealth already removed Wegovy and Saxenda in January 2025, and additional anti-obesity agents will be removed July 1, 2026. Source: MassHealth pharmacy notice. If you're currently on medication, the cash-pay options listed here become your fallback.
Can You Get GLP-1 Online in Massachusetts Legally?
Yes. Massachusetts allows telehealth prescribing, and the same standard of care applies whether the visit happens in person or online. Source: Massachusetts Board of Registration in Medicine telemedicine policy. But there are rules worth knowing.
The basics:
- Any clinician prescribing to a Massachusetts patient must hold an active Massachusetts medical license.
- The consultation must happen through a HIPAA-compliant platform.
- A real prescription from a licensed physician is required — no exceptions.
How to verify before you pay:
- 1Check the clinician's MA license. mass.gov license lookup — search for the prescriber's name. Active license = legitimate. If the provider won't tell you who's prescribing, walk away.
- 2Check the pharmacy. For 503B outsourcing facilities, verify FDA registration at fda.gov. For 503A pharmacies, check state board of pharmacy licensing.
- 3Confirm what you're getting. The provider should clearly disclose whether the medication is FDA-approved or compounded. If they blur the line, that's a red flag — the FDA has taken enforcement action against companies doing exactly that. Source: FDA, April 2026.
Every provider in our comparison below ships statewide in Massachusetts and meets these baseline checks.
Which GLP-1 Providers Are Worth Considering in Massachusetts?
We evaluated providers on seven criteria: Massachusetts availability, licensing transparency, medication type disclosure, pharmacy sourcing, pricing clarity, cancellation terms, and track record. Here's what we found.
| Provider | Type | Semaglutide | Tirzepatide | Month 1 | Ongoing | Best For |
|---|---|---|---|---|---|---|
| Ro | FDA-approved | ✅ (Wegovy pill & pen) | ✅ (Zepbound KwikPen/vials) | $39 memb + $149–199 | $149 + $199–449 | Insurance-first, brand-name |
| Eden Health | Compounded (prescribed) | ✅ | ✅ | $149 | $249 | Cash-pay, transparent |
| MEDVi | Compounded (prescribed) | ✅ | ✅ | $179 | $299 | Low entry price |
| TrimRX | Compounded (prescribed) | ✅ | ✅ | ~$129–149 | ~$199 | Budget alternative |
| LillyDirect | FDA-approved (brand) | ❌ | ✅ (Zepbound) | $299 | $299–449 | Brand-name tirzepatide |
| Hims & Hers | FDA-approved + compounded | ✅ (Wegovy) | ✅ | $39 memb + $149–199 | $149 memb + varies | Name recognition |
Pricing labeled "provider-stated" was pulled from provider websites but not independently verified through test enrollment. Prices with a direct link were verified from live provider pages April 2026.
Ro
FDA-approvedFrom
$39 memb + $149 med
then $149 + $199–449/mo
Best for: Insurance-first, brand-name FDA-approved medication
Who it's for: If you still have any chance at insurance coverage, or you specifically want FDA-approved, brand-name medication — Ro is the play.
Ro centers entirely on FDA-approved GLP-1s — Wegovy (pen and the new pill), Foundayo (orforglipron), Zepbound (KwikPen and vials), Ozempic, and Saxenda. Their platform includes a dedicated insurance concierge that fights for prior authorization and coverage on your behalf. If your employer opted into continued coverage, Ro can help you actually use it. If insurance doesn't work out, Ro offers cash-pay at manufacturer pricing. Source: Ro pricing page, verified April 2026.
How pricing works: Ro Body membership is $39 first month, $149/month after (or $74/mo with annual prepay). Medication is billed separately. Wegovy pill starts at $149/month, Wegovy pen at $199/month, Zepbound KwikPen at $299/month for the first fill.
Important note
The honest tradeoff: Ro is not the cheapest monthly route — $194–$494+/month depending on drug and dose. If low monthly cost matters most, a compounded cash-pay option will be significantly cheaper. But because Ro sticks exclusively to FDA-approved medications and actively works your insurance, it's the safest first move for anyone who still has a realistic shot at coverage.
Check your insurance eligibility with Ro — takes 5 minutesEden Health
Compounded (prescribed)Top PickFrom
$149
then $249/mo
Best for: Cash-pay after insurance loss — transparent pricing, no hidden fees
Who it's for: Your insurance is gone. You know it. You need an affordable path forward that doesn't require fighting with your carrier.
Eden connects patients with independent licensed providers and state-licensed pharmacies for compounded semaglutide and tirzepatide programs. Source: Eden program page. Their pricing: $149 for the first month when prescribed, $249/month ongoing. No membership fee layered on top. No surprise jump after a promotional window.
We like Eden for the Massachusetts audience specifically because the pricing model is transparent enough to plan around — and right now, planning is what Massachusetts residents need more than anything.
The honest tradeoff
Think about what $249/month actually buys you. It buys you the 20, 40, 60+ pounds you've already lost. It buys you not going backward. That's not an expense — it's protecting an investment you already made in your health.
See Eden Health's Current Pricing →MEDVi
Compounded (prescribed)From
$179
then $299/mo
Best for: Low advertised entry price on compounded semaglutide
MEDVi's compounded semaglutide program starts at $179 for the first month and $299/month for refills. Source: MEDVi pricing page. They've scaled rapidly and serve a large patient base.
What to know before enrolling
If MEDVi's entry price is the deciding factor, verify these three things before enrolling: (1) confirm the prescribing clinician holds an active Massachusetts license, (2) ask which pharmacy compounds your medication and check its registration, and (3) understand the cancellation and billing terms.
Check MEDVi Availability in Massachusetts →TrimRX
Compounded (prescribed)From
~$129–149
then ~$199/mo
Best for: Budget alternative if Eden's pricing doesn't fit
TrimRX offers compounded semaglutide and tirzepatide programs at competitive pricing. If Eden's pricing doesn't work for your budget, TrimRX is worth exploring as a backup option. Verify current pricing and cancellation terms directly with the provider before enrolling.
See TrimRX current pricing →LillyDirect
FDA-approved (brand)From
$299
then $299–449/mo
Best for: Brand-name Zepbound (tirzepatide) without insurance
If you specifically want FDA-approved tirzepatide without insurance, LillyDirect ships directly from Eli Lilly. The Zepbound KwikPen starts at $299/month. No middleman. No markup. This is the manufacturer selling directly to you.
See LillyDirect pricing →Hims & Hers
FDA-approved + compoundedFrom
$39 memb + $149–199 med
then $149 memb + varies/mo
Best for: Name recognition; Wegovy partnership with Novo Nordisk
Hims now offers both compounded GLP-1 programs and FDA-approved Wegovy through a partnership with Novo Nordisk. Their membership is $39 for the first month, then $149/month, with medication billed separately — Wegovy pen starts at $199/month, Wegovy pill at $149/month. Source: Hims Wegovy page, April 2026.
We rank them below Ro and Eden because Ro's insurance concierge is stronger for the insurance-first path, and Eden's cash-pay pricing is more straightforward for the compounded path. But they're a recognizable name with wide distribution and a dual-track option.
See Hims Weight Loss Options →Local Doctor or Obesity Clinic
Best for: Established physician relationship, complex medical history, or preference for in-person care
Major Massachusetts obesity medicine programs include Mass General Weight Center, Beth Israel Deaconess, and Brigham and Women's. The tradeoff: local care typically costs more (office visit fees, separate pharmacy pricing, less price transparency) and involves more scheduling friction. But for some people — especially those with multiple medications, comorbidities, or a strong preference for face-to-face care — it's the right path.
Ask your doctor specifically whether they prescribe GLP-1 for weight management and what the total monthly cost looks like without insurance.
Are You on Medicare? Here's the Best GLP-1 News in Massachusetts Right Now.
If you're a Medicare beneficiary, the landscape just changed dramatically in your favor.
Medicare GLP-1 Bridge — launches July 1, 2026
How It Works
- Who submits: Your prescribing physician submits a prior authorization directly to a central CMS processor — not your Part D plan.
- Your Part D plan: Doesn't need to opt in. CMS manages the entire program.
- Filling: Any pharmacy. You pay $50/month.
- Who qualifies: Medicare Part D enrollees whose doctor attests they're prescribed the medication for weight reduction and who meet specific BMI and clinical criteria.
The catch
What to do right now
Should You Choose FDA-Approved or Compounded GLP-1?
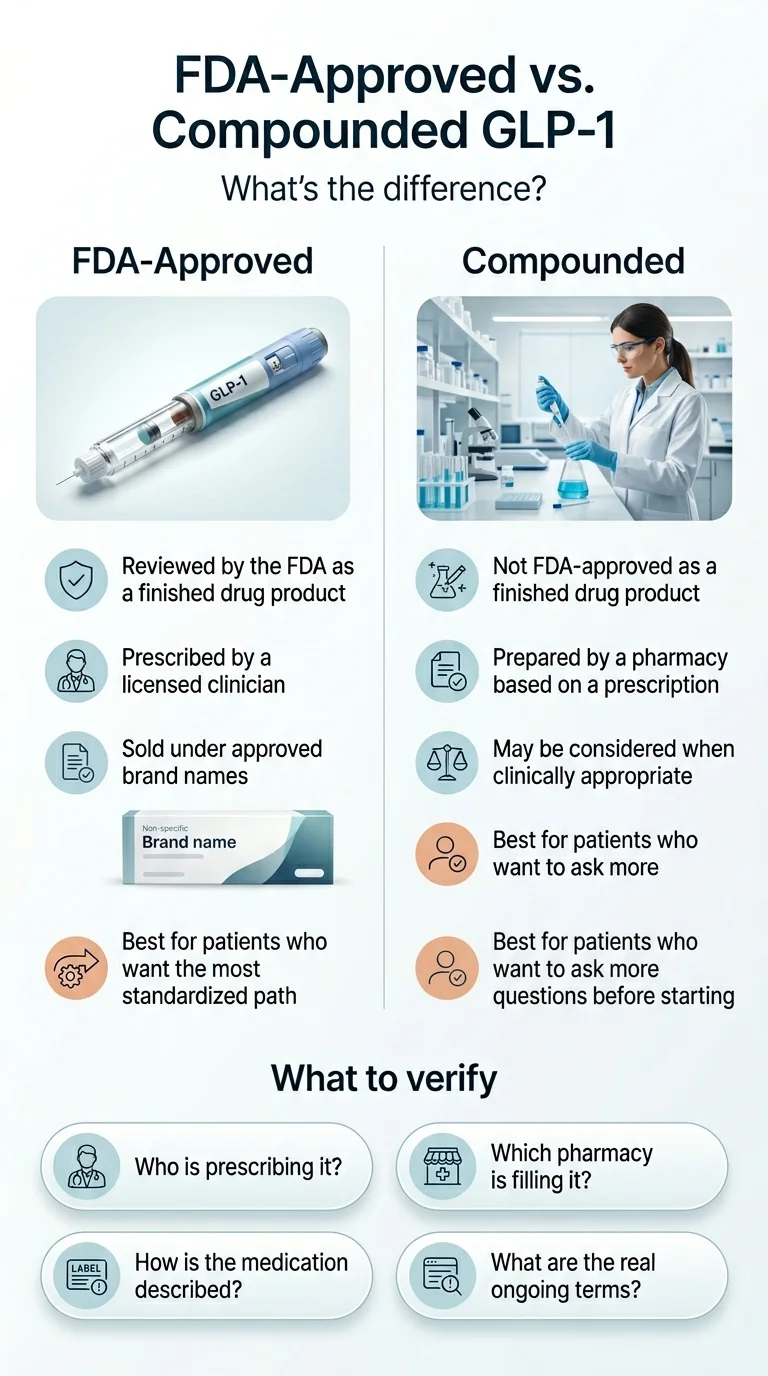
FDA-Approved
- Reviewed by FDA as a finished drug product
- Prescribed by a licensed clinician
- Sold under approved brand names (Wegovy, Zepbound)
- Best for the most standardized path
Compounded (Prescribed)
- Not FDA-approved as a finished drug product
- Prepared by a pharmacy based on a prescription
- May be considered when clinically appropriate
- Better for patients who want to ask more questions first
The regulatory reality — April 2026
What this means for you: If you can access and afford FDA-approved medication — through insurance, Ro, LillyDirect, or the Medicare GLP-1 Bridge — that's the first-line option. If those paths don't work and you're choosing between compounded GLP-1 through a legitimate provider or going without treatment entirely, a properly prescribed compounded medication from a licensed pharmacy is a real option that has helped hundreds of thousands of people continue treatment. The key is choosing a provider that operates transparently.
Semaglutide vs. Tirzepatide: Which Should You Choose?
If you're paying out of pocket, this decision comes down to results vs. cost.
| Semaglutide | Tirzepatide | |
|---|---|---|
| Avg. weight loss (pivotal trials) | ~15% (68 weeks, STEP 1) | ~16–22.5% (72 weeks, SURMOUNT-1) |
| Cash-pay compounded | $149–299/mo | $249–449/mo |
| FDA-approved cash-pay (Ro) | $149–349/mo + $149 memb | $299–449/mo + $149 memb |
| FDA-approved direct (manufacturer) | $149–349/mo via Ro/NovoCare | $299–449/mo via LillyDirect |
What Happens If You Stop Taking GLP-1?
We're including this because it's the fear underneath everything — and it's the reason finding an affordable path matters so much.
Research shows most people regain lost weight within approximately 18 months of stopping GLP-1 medication, along with re-worsening of cardiovascular risk factors, blood pressure, and blood sugar. An endocrinologist at the Massachusetts General Hospital Weight Center has described spending much of his time cobbling together less effective drug regimens for patients who lost coverage — and watching some of them start regaining weight. Source: Boston Globe, March 2026.
That's exactly why finding an affordable continuation plan matters. At $149–249/month through a legitimate provider, you're paying to keep every pound you've already lost. You're paying to protect your blood pressure, your A1C, your joints, your energy. You're paying to not go backward.
If you've been thinking "I'll just try to maintain on my own" — we understand that impulse.
But the data is clear, and so is the experience of Massachusetts residents who've already gone through this. The people who found an affordable alternative and stayed on medication are in a fundamentally different place than the people who stopped and hoped for the best.
Don't Wait — Check Your Eligibility Today →My Insurance Stopped Covering Wegovy or Zepbound — What Do I Do This Week?
If you're in the acute stage — letter just arrived, pharmacy just quoted you four figures — here's your action plan, in order.
Call your HR department today
Ask: "Did our employer opt in to continue GLP-1 weight management coverage for 2026?" At BCBS MA, large employers with 100+ employees have this option. At MGB HP, it's 50+ enrolled subscribers. At HNE, it's 100+ actively enrolled subscribers. Many employees don't know this option exists.
Check whether your diagnosis qualifies
Every Massachusetts insurer that dropped weight-loss coverage has kept diabetes coverage intact. If you have a Type 2 diabetes diagnosis, your GLP-1 may still be fully covered. Talk to your prescribing physician about whether your medical record supports this.
Transition to a cash-pay provider
You do not need to go cold turkey. A telehealth provider can have medication shipped to your door within 5–7 days. Eden Health and Ro are our top picks depending on whether you want compounded or FDA-approved medication.
Use your HSA/FSA
Prescription GLP-1 medications are generally eligible medical expenses. Confirm with your administrator, then use your HSA/FSA card at checkout for immediate savings.
Sample script for calling your plan
"I'm currently prescribed [medication name] for weight management. I understand coverage may have changed. Can you tell me: (1) Does my specific plan still cover this medication under any indication? (2) Did my employer opt in to continued weight management coverage? (3) Is there an appeal or exception process available?"
You don't have to figure this out alone. And you don't have to stop treatment while you figure it out.
How Do You Get Started with GLP-1 Telehealth in Massachusetts?
Once you've picked your path, the process is faster than most people expect.
Choose your provider
Use the comparison table above. If you're unsure, take the quiz.
Complete the health assessment
Medical history, current medications, BMI, and weight management goals. Takes about 5–10 minutes.
Physician review and consultation
A licensed Massachusetts physician reviews your information (usually asynchronous or video). Most complete this within 24–48 hours.
Prescription to pharmacy
If approved, your prescription goes to a licensed pharmacy. Medication ships to your Massachusetts address in temperature-controlled packaging, typically within 3–5 business days.
Ongoing check-ins
Dose adjustments, side effect management, and progress monitoring. This is what separates a medical program from a checkout page.
How to Tell If a GLP-1 Provider Is Legitimate
The surge in demand has attracted serious providers and opportunists alike. Here's how to tell the difference in about five minutes.

7 checks before you pay:
- ✓Does the provider disclose which physician will prescribe? If you can't get a name, don't proceed.
- ✓Can you verify the physician's Massachusetts license? mass.gov license lookup.
- ✓Does the provider name the compounding pharmacy? They should. If they won't, that's a red flag.
- ✓Is the pharmacy a registered 503B outsourcing facility? Verify at FDA.gov.
- ✓Does the provider clearly distinguish FDA-approved from compounded? The FDA has warned more than 30 companies for blurring this line.
- ✓Is pricing transparent before you pay? First-month cost, ongoing cost, what's included, what's not — all clear before checkout.
- ✓What's the cancellation policy? Know before you commit.
Red flags that should make you leave
- ✕ AI-generated before-and-after photos
- ✕ Physicians you can't verify through state licensing
- ✕ Language claiming compounded medications are "FDA-approved"
- ✕ No pharmacy disclosure
- ✕ Countdown timers and fake scarcity
- ✕ No way to reach a real human
Side Effects, Exclusions, and When to Talk to Your Doctor First
GLP-1 medications are well-studied, and for most people the benefits far outweigh the side effects. But this is a medical decision, and you deserve honest information.
Common (usually improve over time)
- Nausea
- Constipation
- Diarrhea
- Reduced appetite
- Occasional fatigue
Typically worst when starting or increasing dose. Smaller meals, hydration, and following your titration schedule helps significantly.
Less common but important
- Pancreatitis (rare)
- Gallbladder issues
- Thyroid concerns (rare)
Your prescribing physician will screen for these before and during treatment.
Talk to your doctor first if you have:
- • A history of medullary thyroid cancer or MEN2 syndrome (contraindications)
- • A history of pancreatitis
- • Multiple medications with potential interactions
- • An active eating disorder
- • Pregnancy or plans to become pregnant
For most healthy adults with obesity or overweight, GLP-1 medications have a strong safety profile backed by extensive clinical trial data. Your prescribing physician — whether through telehealth or in person — will review your complete medical history before prescribing.
Frequently Asked Questions
Still Not Sure Which GLP-1 Program Is Right for You?
We ask about your insurance situation, budget, medication preference, and health goals — then recommend the best provider path for your specific situation in Massachusetts. No email required. No commitment.
Ships statewide in Massachusetts · Pricing verified April 2026
Related guides
How We Evaluated Providers for This Guide
What we checked: Massachusetts-wide service, prescribing clinician licensing, pharmacy disclosure and registration status, medication type disclosure (FDA-approved vs. compounded), published pricing (first month and ongoing), cancellation terms, and any FDA enforcement actions.
What we verified directly: Pricing pages, pharmacy disclosures, licensing claims, cancellation policies, and FDA enforcement database entries — all checked within the past 30 days.
What is provider-stated and not independently verified: Patient outcome claims, internal quality metrics, and customer volume numbers.
Our update commitment: This page is reviewed and updated at least monthly. Insurance coverage data is verified against official insurer notices. Pricing is checked against live provider pages.
Affiliate disclosure: Some links on this page are affiliate links, meaning we may earn a commission if you sign up through our link at no extra cost to you. This does not influence which provider we recommend. Our recommendations are based on the evaluation criteria above.
The test we apply: If we removed every affiliate link from this page, would it still be the most useful GLP-1 resource for Massachusetts residents? We believe it is.
Sources: Official notices from Blue Cross Blue Shield of MA, Point32Health, Mass General Brigham Health Plan, WellSense Health Plan, Health New England, the MA Group Insurance Commission (GBH News, WBUR), the MA Health Policy Commission, MassHealth pharmacy notices, CMS.gov (Medicare GLP-1 Bridge), the FDA enforcement database, the Daily Hampshire Gazette, the Boston Globe, the New England Journal of Medicine, IRS Publication 502, and direct verification of provider pricing pages. All sources accessed and verified in April 2026.