Wegovy Prior Authorization Denied? Here's Exactly What to Do Next
By Weight Loss Provider Guide Team · Last verified: April 7, 2026
Wegovy prior authorization denied? That usually means one of three things: your doctor's paperwork was incomplete, your insurer says you don't meet their clinical criteria, or your plan excludes weight-loss drugs entirely. Each one has a different fix — and picking the wrong path wastes weeks you don't have.
If the denial was a paperwork problem, your doctor can correct and resubmit — often without a formal appeal. If it was a criteria issue, a targeted appeal with the right evidence can overturn the decision. And if your plan truly excludes weight-loss medications, a standard appeal usually won't work — but you still have real options, including alternative FDA-approved indications, reduced self-pay pricing, and telehealth paths that bypass insurance altogether.
Most private and employer-sponsored plans give you up to 180 days to file an internal appeal, though Medicare and some other plan types have shorter windows. You have time to do this right, but not time to do it twice. This guide will help you decode exactly why you were denied, decide whether to resubmit, appeal, or pivot, and take the right next step — starting today.
This page is for you if: You already received a Wegovy PA denial (letter, portal message, or pharmacy rejection).
Not for you if: You haven't submitted a PA yet — start with our guide to getting Wegovy prior authorization approved.
Key number: Up to 180 days for internal appeal under most commercial plans. Medicare deadlines are shorter — check your denial letter.

Quick-Reference: What Your Denial Probably Means
Find the language closest to what your denial letter says:
If your denial says: "Incomplete information" or "additional documentation required"
If your denial says: "Does not meet medical necessity criteria"
If your denial says: "Step therapy required" or "try preferred alternative first"
If your denial says: "Non-formulary" or "not on preferred drug list"
If your denial says: "Benefit exclusion" or "weight management not covered"
If your denial says: "Continuation criteria not met" or "renewal denied"
Sources: Novo Nordisk denial/appeals guide (NovoMedLink); Healthcare.gov appeal rights
Why Was Your Wegovy Prior Authorization Denied?
Most Wegovy denials aren't random. They fall into five predictable categories, and your best next move depends entirely on which one you're in. Before you do anything else, find the exact denial wording — it's in your denial letter, your insurer's online portal, the Explanation of Benefits (EOB), or the pharmacy rejection notice.
Missing or Incorrect Documentation
Most common — and easiest to fixYour doctor's office submitted the PA, but something was missing or wrong: BMI or weight records not attached, no documented history of prior weight-loss attempts, missing or incorrect ICD-10 diagnosis codes, lab results not included, or paperwork arriving after the insurer's review window.
You Didn't Meet Clinical Criteria
Appealable if evidence was incompleteYour insurer reviewed the PA and decided you don't qualify based on their medical policy. Common reasons: BMI not documented at or above threshold (typically ≥30, or ≥27 with a qualifying comorbidity), no qualifying weight-related condition documented, no evidence of a structured weight-management program — some insurers including CVS Caremark require 3–6 months documentation before approving Wegovy.
Step Therapy Required
Two paths: document failures or complete step therapyYour insurer wants you to try a cheaper medication first — phentermine, liraglutide (Saxenda), topiramate, naltrexone/bupropion (Contrave), or metformin (off-label).
Wegovy Is Non-Formulary
Formulary exception request availableWegovy isn't on your plan's approved drug list, but weight-loss medications aren't explicitly excluded either. This is different from a benefit exclusion.
Weight-Loss Medications Are Excluded From Your Benefits
Standard appeals rarely succeed — pivot insteadYour plan doesn't cover any medications prescribed for weight loss — period. It's not a documentation issue or a criteria issue. In 2025, KFF reported that 19% of firms with 200+ workers covered GLP-1s for weight loss. Medicare still does not cover drugs prescribed solely for weight loss, though new pathways are opening.
Resubmit, Appeal, or Pivot: The 30-Second Decision
If the denial was a paperwork problem, don't file an appeal — resubmit. If it was a criteria problem, appeal with better evidence. If it's a true exclusion, stop burning weeks on appeals and pivot to a path that actually works. Getting this decision right in the first 24 hours is the difference between starting treatment soon and spinning your wheels for a month.
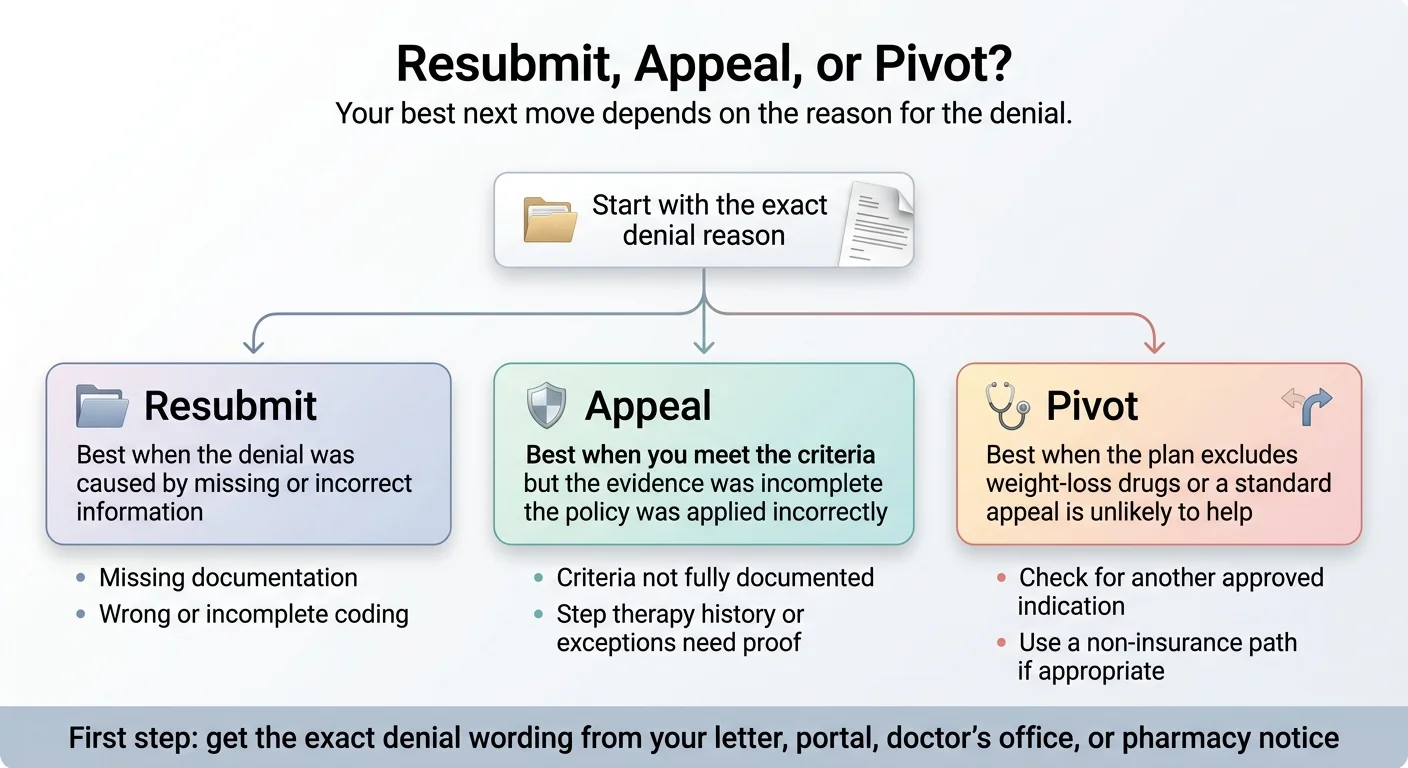
Correct & Resubmit
- Missing documents (labs, weight history, chart notes)
- Wrong or incomplete ICD-10 codes
- PA form errors or omissions
- Documentation that arrived late
File a Formal Appeal
- You meet BMI criteria but it wasn't documented
- You have qualifying comorbidities not included
- You tried and failed step therapy medications
- Renewal denied due to framing error (current vs baseline BMI)
Pivot to Alternative Path
- True benefit exclusion — plan doesn't cover weight-loss drugs
- Standard appeal won't change plan design
- Alternative FDA-approved indication available
- Self-pay or telehealth is the faster path
The benefit exclusion trap — don't spend 4–8 weeks here
Novo Nordisk's own provider-facing denial guide acknowledges that benefit exclusions typically don't have ordinary appeal rights. A standard appeal against a true benefit exclusion usually returns the same answer: "This benefit is not included in your plan." That's a plan design decision — not a reflection of your health or your need.
Your fastest path forward is one of these: alternative FDA-approved indication, employer benefits advocacy, self-pay brand Wegovy through NovoCare, or a telehealth GLP-1 program that doesn't require insurance.
What to Do in the Next 24 Hours
Most people waste the first day after a denial searching emotionally instead of doing the three things that actually matter: getting the exact denial reason, confirming the deadline, and starting the documentation file.
Get the Exact Denial Wording
Not "I was denied." The actual language. Pull it from the denial letter mailed to your home, your insurer's member portal (under "claims" or "authorizations"), the Explanation of Benefits (EOB), your doctor's office — they usually get notified first — or the pharmacy rejection screen.
Write down or screenshot the exact reason. This is the single most important piece of information you need.
Confirm Your Appeal Deadline
For most commercial and employer-sponsored plans, you have up to 180 days from the denial notice. Medicare Part D deadlines are typically 60 calendar days. Call the insurer and ask: "What is my deadline to file an internal appeal for this denial?" Also ask whether you have external review rights.
Write down the deadline, the reference number, and the name of the person you spoke with.
Start Your Documentation File
Whether you're resubmitting, appealing, or pivoting, organize your records now.
- The denial letter itself
- A copy of the original PA submission (ask your doctor's office)
- Your weight and BMI history (before treatment and current)
- List of comorbidities with diagnosis codes
- Records of prior weight-loss attempts (programs, medications, dates, outcomes)
- Lab results your insurer may want
- Notes from every phone call (date, time, name, what was said)
What Not to Do
- • Don't assume "denied" means "denied forever." Many denials are paperwork issues that get resolved in days.
- • Don't file a generic appeal without reading the denial reason. An appeal that doesn't address the actual denial reason will almost certainly fail.
- • Don't miss the deadline. Set a calendar reminder for 30 days before it expires.
- • Don't spend weeks appealing a true benefit exclusion. Check first.
- • Don't panic-buy full-price Wegovy. Self-pay options at much lower pricing exist (covered below).
Exactly What to Say When You Call Your Insurance Company
The call isn't for arguing. It's for extracting the insurer's exact rules so you know what you're working with. Think of it as an information-gathering mission, not a negotiation.
Questions to ask your insurer
- 1."What is the exact denial reason on file for this prior authorization?"
- 2."Is this a missing-information issue, a criteria issue, step therapy, non-formulary, or a benefit exclusion?"
- 3."What clinical policy or criteria document was used to evaluate my request?" (Ask them to send it to you — you have the right to see it.)
- 4."Can my provider correct and resubmit the PA, or does this require a formal appeal?"
- 5."What specific documentation was missing or insufficient?"
- 6."What is my deadline for filing an internal appeal?"
- 7."Do I have external review rights?"
- 8."If this is a benefit exclusion, is there any medical exception process?"
- 9."What is the correct submission method — portal, fax, or mail — and what's the case or reference number?"
Ask them to send you the criteria document and appeal instructions in writing (portal message or email). Don't rely on verbal answers alone. Pro tip: If you have an employer-sponsored plan and the denial is a benefit exclusion, also call your HR or benefits department — they can tell you whether adding GLP-1 coverage is being considered for the next enrollment period.
What Your Doctor Needs to Include in the Appeal
The appeal packet is where most cases are won or lost, and the quality of your doctor's letter of medical necessity is the single biggest factor. Novo Nordisk provides appeal letter templates to healthcare providers through NovoMedLink.

Start here
- Denial letter
- Exact denial wording
- Appeal deadline
- Case or reference number
Clinical evidence
- Diagnosis with ICD-10 codes (E66.01, E66.09, E11.x, I10, G47.33, E78.x, etc.)
- Baseline weight and BMI — documented before Wegovy
- Current weight and BMI with percentage change from baseline
- Weight-related comorbidities each documented in medical records
- Cardiovascular disease history (if applicable — opens different coverage pathway)
- Prior weight-loss attempts — dates, types, duration, outcomes
- Prior medications tried — names, doses, dates, why stopped
- Structured weight-management program documentation (3–6 months if required)
- Letter of medical necessity
- Relevant lab results (A1C, lipid panel, liver enzymes, sleep study)
- Chart notes from recent visits
For renewal appeals (maintenance PA denials)
- Treatment start date and baseline weight/BMI before Wegovy
- Current weight/BMI framed as percentage change from baseline
- Duration on stable maintenance dose
- Documentation of maintained initial weight loss
- Clinical rationale for continued treatment (obesity is chronic — stopping leads to regain)
- Chart notes from recent follow-up visits
What the Letter of Medical Necessity Must Do
This isn't a form letter. It needs to:
- 1.Name the exact denial reason and directly address it
- 2.Explain why the denial is incorrect based on the clinical evidence
- 3.Connect your condition to the insurer's own criteria — reference their policy document by name if possible
- 4.Detail why alternatives are inappropriate — prior failures, contraindications, or clinical reasons step therapy isn't right
- 5.Explain the clinical consequences of treatment interruption — weight regain, worsening comorbidities, cardiovascular risk
Point your doctor to NovoMedLink for Wegovy-specific appeal letter templates.
Ask About a Peer-to-Peer Review
Some insurers offer a peer-to-peer discussion between your prescribing doctor and the plan's reviewing clinician. This can sometimes resolve a denial faster than a written appeal — the insurer's medical director may approve the PA after hearing the clinical case directly. Not every insurer offers this, but it's worth asking.
What If Your Wegovy Renewal or Maintenance PA Was Denied?
Renewal denials might be the most frustrating category. You've been on Wegovy. It's working. You've lost weight. And now your insurer says you don't qualify anymore. It feels backwards — and real patients describe it exactly that way.
Why Maintenance Denials Happen (Even When Treatment Is Working)
Most insurers require periodic re-authorization — typically every 3–6 months. The continuation criteria are different from the initial approval criteria, and that's where things break down. Common continuation requirements include:
- • Documentation that you've been on a stable maintenance dose for at least 3 months
- • Proof that you've lost at least 5% of your baseline (starting) body weight — not 5% of your current weight
- • Ongoing documentation of weight-management lifestyle modifications
- • Updated chart notes from your prescribing provider
The critical mistake: If your doctor submits the renewal with only your current BMI — which may now be lower because the medication is working — the insurer may decide you no longer meet the BMI threshold for coverage. The renewal should be built around your baseline weight before treatment, your percentage loss from that baseline, and the clinical case for continued treatment.
What real patients say about renewal denials:
"Feels like I'm being punished now that the medicine has started to work." — r/WegovyWeightLoss
"Both had their doctors resubmit with additional information and both got approved." — r/WegovyWeightLoss
That's the pattern we see most often: initial renewal denial → resubmission with better baseline documentation → approval. Ask your doctor to document your baseline weight and BMI at the start of treatment and keep it in your chart permanently.
Can You Appeal If Your Plan Says Wegovy Is Excluded?
Sometimes — but this is where you need to be strategic about where you spend your energy.
Non-formulary
Wegovy isn't on your plan's preferred drug list, but the plan does cover the category. You can request a formulary exception with supporting documentation — and these can succeed.
Benefit exclusion
Your plan does not cover weight-loss medications at all — the entire medication class is outside your benefit. Standard appeals have very low success rates here.
When a Medical Exception Might Still Work
- • Your condition involves a different FDA-approved indication (cardiovascular risk reduction, MASH)
- • Your doctor can make a case that Wegovy is medically necessary for a covered condition, not weight loss
- • Your plan has a general medical exception process
If You Have an Employer-Sponsored Plan: Talk to HR
Ask your HR or benefits team whether adding GLP-1 coverage is being considered for next enrollment, how to formally request it, and whether you can get coworkers to support the request. Coverage decisions are revisited annually — your voice matters here. Employer coverage of GLP-1s has been growing steadily year over year.
Are There Other Covered Ways to Get Wegovy (or Another GLP-1)?
Yes — and this section is where most denial guides stop too early. Wegovy isn't just a weight-loss medication anymore. If your weight-management coverage was denied, a different diagnosis might open a completely different coverage door.
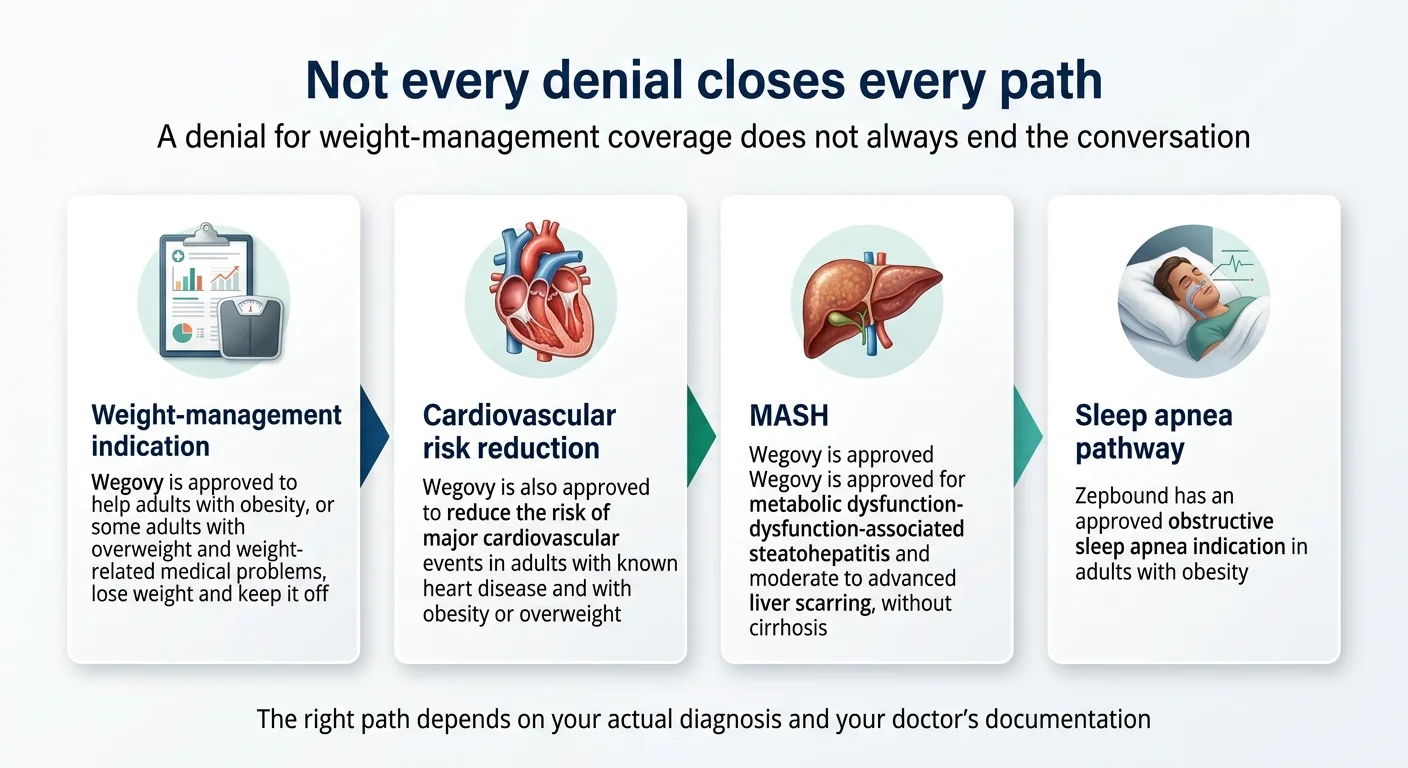
The Cardiovascular Risk Reduction Pathway
In March 2024, the FDA approved Wegovy for reducing the risk of major adverse cardiovascular events (heart attack, stroke, and cardiovascular death) in adults with established cardiovascular disease and obesity or overweight. Some plans that exclude weight-loss drugs still cover cardiovascular medications. Medicare now covers obesity medicines like Wegovy when FDA-approved for another covered medical reason such as cardiovascular risk reduction.
Who this applies to: Adults with documented cardiovascular disease (heart attack, stroke, peripheral artery disease, coronary artery disease) AND obesity or overweight. This is not a general workaround — it requires real cardiovascular disease history.
The MASH (Liver Disease) Pathway
Wegovy has an FDA-approved indication for metabolic dysfunction-associated steatohepatitis (MASH) with moderate-to-advanced liver fibrosis. If you have documented MASH, this may create a separate coverage pathway.
The Sleep Apnea Pathway (Zepbound)
If Wegovy was denied but you have documented moderate-to-severe obstructive sleep apnea, Zepbound (tirzepatide) has an FDA-approved indication for that condition. Your doctor may be able to prescribe Zepbound under the sleep apnea indication — especially worth exploring if your plan covers sleep apnea treatment but excludes weight-loss drugs.
| Your diagnosis | Possible drug | Coverage angle | What your doctor submits |
|---|---|---|---|
| Established cardiovascular disease + obesity/overweight | Wegovy | CV risk reduction (not weight loss) | PA under cardiovascular indication with CVD documentation |
| MASH with moderate-to-advanced fibrosis | Wegovy | Liver disease treatment | PA under MASH indication with fibrosis documentation |
| Moderate-to-severe obstructive sleep apnea + obesity | Zepbound | Sleep apnea treatment | PA under OSA indication with sleep study |
| Type 2 diabetes | Ozempic (same active ingredient as Wegovy) | Diabetes management | PA under diabetes indication — talk to your doctor |
Important: These are not workarounds or loopholes. They are legitimate FDA-approved uses of these medications. Your doctor needs to determine whether any of these apply to your clinical situation.
Can You Still Get Wegovy (or Semaglutide) If Insurance Denied It?
Yes — and the out-of-pocket cost is significantly lower than most people expect. Whether you're still appealing or you've decided to move on, you have several real options at real prices.
Brand-Name Wegovy Self-Pay (Through NovoCare)
Novo Nordisk offers reduced self-pay pricing for Wegovy through NovoCare Pharmacy:
- • Wegovy pill (oral tablet, 1.5 mg): $149/month. The 4 mg tablet is $149/month through August 31, 2026, then $199/month.
- • Injectable Wegovy pens: Starting at $199/month for introductory doses. Higher doses may be priced higher.
- • No insurance required. Available at NovoCare Pharmacy directly.
Source: Wegovy.com self-pay pricing. Verified April 2026. Subject to change.
Telehealth GLP-1 Programs (No Insurance Required)
Telehealth providers prescribe compounded semaglutide or tirzepatide with no prior authorization and no insurance required. You consult with a licensed physician, get prescribed if eligible, and receive medication shipped to your home — often within the same week.
Important: Compounded GLP-1 drugs are not FDA-approved and are not the same as brand-name Wegovy. According to the FDA, compounded drugs have not been reviewed for safety, effectiveness, or quality the way FDA-approved products have. They are legal when prescribed by a licensed provider and dispensed by a licensed compounding pharmacy.
Programs worth considering if your plan excludes weight-loss coverage:
MEDVi
A comprehensive physician-supervised semaglutide program with medication, provider consultations, and shipping included. Strong clinical support and ongoing monitoring starting at $179/month.
Check If You Qualify for MEDViEden Health
Good option if you want a more clinical experience with licensed providers and a focus on the full treatment picture. No PA required.
See Eden's GLP-1 Plans| Option | Monthly cost | What you get | Best for |
|---|---|---|---|
| Appeal and get Wegovy covered by insurance | Your plan's copay (if approved) | FDA-approved Wegovy at insurance pricing | Patients with fixable denials who meet criteria |
| Oral Wegovy self-pay (NovoCare) | $149–$199/mo | FDA-approved Wegovy tablets, no insurance needed | Patients who want brand-name at reduced cost |
| Injectable Wegovy self-pay (NovoCare) | $199–$349/mo | FDA-approved Wegovy pens, no insurance needed | Patients who prefer injections at reduced cost |
| MEDVi (telehealth) | Starting at $179/mo | Physician-supervised semaglutide, home delivery, ongoing support | Patients who want affordable treatment now without insurance delays |
| Eden Health (telehealth) | Starting at $129/mo | Compounded GLP-1 program, licensed providers, same-price guarantee at every dose | Patients seeking low-cost cash-pay option |
Pricing verified April 2026. All pricing subject to change.
What Are Your Chances of Winning an Appeal?
Appeal outcomes vary widely by plan and denial reason. But here's what the data shows: KFF found that in Medicare Advantage, about 11.5% of denied prior authorization requests were appealed in 2024, and 80.7% of those appeals fully or partially overturned the initial denial.
The bigger problem? Fewer than 1 in 10 patients ever file an appeal at all. Most people accept the denial and either pay out of pocket or give up on treatment. Don't be most people.
Appeals worth fighting
- ✓ Denial for missing documents or wrong codes (resubmission, not even a formal appeal)
- ✓ You meet clinical criteria but evidence wasn't properly submitted
- ✓ You have documented step therapy failures or contraindications
- ✓ Renewal denied because current BMI used instead of baseline weight-loss data
- ✓ Your doctor is willing to write a detailed LMN and/or do peer-to-peer
Appeals that rarely succeed
- ✗ True benefit exclusions (plan doesn't cover weight-loss drugs at all)
- ✗ Cases where you genuinely don't meet the criteria and no alternative indication exists
- ✗ Appeals without specific documentation addressing the denial reason
Patient appeal vs. provider appeal: You have the right to file an appeal yourself, but provider-submitted appeals carry more clinical weight. Under ACA regulations, most non-grandfathered plans must provide at least one internal appeal and one external review by an independent third-party reviewer. External review is your strongest tool if the internal appeal fails.
How Long Do You Have to Appeal?
Move like you have 180 days but plan like you have 30. Most commercial and employer-sponsored plans allow up to 180 days from the denial notice for an internal appeal. Medicare deadlines are shorter — typically 60 calendar days for Part D. The sooner you act, the sooner you're either approved or free to pursue alternatives.
| Milestone | Typical timeline |
|---|---|
| Internal appeal deadline (most commercial plans) | Up to 180 days from denial |
| Internal appeal deadline (Medicare Part D) | 60 calendar days (confirm on denial letter) |
| Internal appeal decision (pre-service) | Generally within 30 days |
| Internal appeal decision (urgent/expedited) | 72 hours |
| External review deadline | Generally 4 months after final internal appeal denial |
| External review decision | Usually within 45 days |
If you're close to the deadline
File a basic internal appeal immediately — even an incomplete one — to preserve your rights. You can supplement with additional documentation after filing. Missing the deadline may permanently close your appeal option.
Our Sources and What We Verified
| What we checked | Source | Last verified |
|---|---|---|
| Denial categories and appeal paths | Novo Nordisk denial/appeals guide (NovoMedLink) | April 2026 |
| Appeal rights and timelines | Healthcare.gov, CMS | April 2026 |
| Continuation/renewal criteria | CVS Caremark PA criteria document | April 2026 |
| Wegovy self-pay pricing | Wegovy.com, NovoCare | April 2026 |
| Cardiovascular/MASH/OSA indications | FDA prescribing information and approvals | April 2026 |
| Medicare coverage and GLP-1 Bridge | CMS, NovoCare Medicare page | April 2026 |
| Employer coverage statistics | KFF/Health System Tracker (2025) | April 2026 |
| Prior authorization appeal data | KFF Medicare Advantage analysis (2024) | April 2026 |
What We Don't Claim: We don't guarantee any appeal outcome. Individual plan criteria, coverage decisions, and eligibility determinations are unique to each patient and plan.
How We Make Money: This page includes links to providers we may earn a commission from if you sign up. This doesn't affect our editorial process. We recommend providers we've vetted.
Not Medical or Legal Advice: This page is for informational purposes. Consult your prescribing healthcare provider, insurer, or a patient advocate for decisions about your specific situation.
Frequently Asked Questions
Don't let a denial stop your treatment
Whether you're appealing or ready to explore cash-pay options — physician-supervised GLP-1 programs are available now, with no prior authorization and same-week shipping for eligible patients.