GLP-1 Providers That Accept Medicare
By WPG Research Team · Last verified: April 9, 2026 · Sources: CMS.gov, provider websites, KFF, FDA
Weight Loss Provider Guide is an independent comparison resource for GLP-1 telehealth providers. We may earn a commission when you visit a provider through our links, at no additional cost to you. Our editorial assessments are based on publicly available information verified on the dates noted. Full disclosure below.
Bottom line:
We verified every major online GLP-1 provider's Medicare policy. Only three clearly qualify as GLP-1 providers that accept Medicare for clinical visits right now: Form Health (best overall, 91/100), knownwell (best with no membership fee, 88/100), and Shapely (best if you live in CA, FL, NY, or TX, 76/100).
Starting July 1, 2026, the Medicare GLP-1 Bridge covers Wegovy, Zepbound KwikPen, and Foundayo at a flat $50/month for eligible Part D beneficiaries. None of the providers on this page are perfect — but these three are the only ones we found that actually work with your Medicare benefits.
Jump to section
- Medicare Compatibility Matrix (10 Providers)
- Form Health — Best Overall (91/100)
- knownwell — Best No Membership Fee (88/100)
- Shapely — Best in CA, FL, NY, TX (76/100)
- Provider Acceptance vs Drug Coverage
- Does Medicare Cover Wegovy, Zepbound, Ozempic?
- The Medicare GLP-1 Bridge: Who Qualifies?
- Original Medicare vs Medicare Advantage
- What to Do If Your Medication Is Denied
- Providers That Do NOT Accept Medicare
- Best Fallback Paths If Medicare Won't Cover
- How to Prepare for the Bridge Now
- What Happens After the Bridge Ends?
- FAQ: 13 Questions Answered

Which GLP-1 Providers That Accept Medicare Can You Actually Use?
Most online GLP-1 providers do not accept Medicare. We checked the insurance and billing pages for every major telehealth weight loss program as of April 2026 and scored them on a transparent 100-point rubric. The verified short list is small: Form Health, knownwell, and Shapely are the only three that clearly bill Medicare for clinician visits.
Scoring Rubric
30 pts
Clearly accepts/bills Medicare for clinician visits
20 pts
Helps with insurance navigation and prior authorization
15 pts
Offers an FDA-approved medication path
15 pts
Geographic reach
10 pts
Transparent self-pay fallback if insurance fails
10 pts
Friction/trust factors (clarity, exclusions)
Medicare Compatibility Matrix — Verified April 9, 2026
| Provider | Medicare Score | Accepts Medicare for Visits? | Helps with Prior Auth? | Medication Path | Self-Pay Fallback | Gov't Insurance Excluded? |
|---|---|---|---|---|---|---|
| Form Health | 91/100 | Bills visits and labs through Medicare | Insurance navigation built in | FDA-approved (Wegovy, Zepbound, Contrave, Saxenda) | $299/mo self-pay plan | No — accepts Medicare |
| knownwell | 88/100 | Accepts Medicare and most major plans | Yes | FDA-approved only | $299 first visit / $149 follow-up | No — accepts Medicare |
| Shapely | 76/100 | Original Medicare + most MA PPO in CA, FL, NY, TX | Yes | FDA-approved + compounded fallback | Copays as low as $15; compounded from $99 | No — accepts Medicare in 4 states |
| Ro | 39/100 | Cannot coordinate government insurance | Commercial plans only | FDA-approved + cash-pay | $39 first mo / $149/mo + med cost | Yes — government insurance excluded |
| PlushCare | 18/100 | Dropped Medicare Part B Jan 2026; some MA may work | Limited | FDA-approved | Per-visit self-pay | Mostly — see text |
| Walgreens | 8/100 | Self-pay only, ages 18–64, no insurance | No | FDA-approved | $49/visit self-pay | Yes — no insurance billing |
| MEDVi | N/A | Cash-pay only | No | Compounded (not FDA-approved) | $179 first mo / $299 refills | Yes — cash-pay only |
| Eden | N/A | Not enrolled with Medicare/Medicaid | No | Compounded (not FDA-approved) | Cash-pay | Yes — cash-pay only |
| TrimRx | N/A | Direct-to-patient cash model | No | Compounded (not FDA-approved) | From $199/mo | Yes — cash-pay only |
| SkinnyRx | N/A | Not enrolled in Medicare/Medicaid | No | Compounded (not FDA-approved) | Cash-pay | Yes — cash-pay only |
Sources: Form Health FAQ and insurance page (formhealth.co, April 2026), knownwell insurance page (knownwell.co, April 2026), Shapely Medicare page (getshapely.com, April 2026), provider insurance/terms pages. Verified April 9, 2026.
Best Overall for Most Medicare Beneficiaries: Form Health
Form Health
Best Overall91/100Accepts Medicare · Bills visits + labs through insurance · FDA-approved anti-obesity medications only
Form Health is the strongest verified answer for Medicare beneficiaries looking for an online GLP-1 provider because it explicitly accepts Medicare, bills clinician visits and labs through insurance, and stays exclusively on the FDA-approved anti-obesity medication side. It is staffed by board-certified obesity medicine physicians — not general practitioners who happen to prescribe GLP-1s on the side.
Why Form Health wins this comparison
It actually bills Medicare for visits and labs. Form Health's insurance page explicitly lists Medicare, alongside major commercial plans like Blue Cross Blue Shield, Cigna, Aetna, and UnitedHealthcare. When your visit is covered, you pay your plan's copay — not a separate subscription fee on top of your insurance.
It focuses on FDA-approved anti-obesity medications. Form Health names Wegovy, Zepbound, Contrave, and Saxenda in its public FAQ — drugs with FDA-approved weight management indications. Compounded GLP-1s cannot be billed to Medicare under any pathway. Form keeps you in the FDA-approved lane.
It has a self-pay fallback. If Medicare covers your visits but the medication itself gets denied, Form offers a $299/month self-pay program so you are not left stranded.
It requires an existing PCP relationship. You need a primary care provider and a PCP visit within the last 12 months. Some people will see that as friction. We see it as a feature — it builds on your existing medical team, which makes prior authorization requests stronger.
Best for
- • Medicare beneficiaries who want visits billed to insurance
- • Anyone planning to use the Bridge in July 2026
- • People who prefer FDA-approved medications only
Honest tradeoff
Form Health is NOT the cheapest or fastest path. If you want $179/month compounded shipped in a week with no PCP requirement, Form is not built for that. But if you are on Medicare and want a provider that works with your coverage, Form is the cleanest verified path we found.
Best No-Membership-Fee Option: knownwell
knownwell
Best No Membership Fee88/100Accepts Medicare · Nationwide virtual care · No membership fee · Transparent per-visit pricing
knownwell is the strongest second choice for Medicare beneficiaries who want a GLP-1 provider with no recurring subscription fee. It accepts Medicare and most major commercial insurance plans, offers nationwide virtual care, and charges nothing for membership — you pay per visit or your insurance copay.
No membership fees. Most telehealth GLP-1 programs charge $99–$199/month just for access to a provider, before the medication cost. knownwell does not. You pay per appointment — $299 for the first visit and $149 for follow-ups if self-paying, or your Medicare copay if your plan covers the visit.
Accepts Medicare with nationwide virtual coverage. knownwell's insurance page lists Medicare alongside major commercial plans, and its virtual care model is available nationwide — not locked to a handful of states.
Transparent self-pay pricing. If your Medicare plan does not cover knownwell as in-network, you know exactly what you will pay upfront. No hidden fees. No surprise charges after the visit.
Best for
- • Medicare beneficiaries avoiding monthly subscriptions
- • People outside Form Health's coverage area
- • Beneficiaries who want per-visit billing with no commitment
Honest tradeoff
knownwell does NOT have the most detailed Medicare-specific onboarding experience. Form Health makes the Medicare pathway clearer during signup. But knownwell's no-fee structure and nationwide reach make it the best alternative when Form is not available or when you want to minimize ongoing costs.
Best if You Live in CA, FL, NY, or TX: Shapely
Shapely
Best in CA, FL, NY, TX76/100Original Medicare + most MA PPO · CA, FL, NY, TX · Dietitian included · Copays as low as $15
Shapely is the most straightforward Medicare match if you happen to live in one of its four states. Its Medicare page explicitly says it accepts Original Medicare and most PPO Medicare Advantage plans in California, Florida, New York, and Texas.
It names Medicare on a dedicated page. While many providers bury their insurance information, Shapely has a page specifically addressing Medicare acceptance. It publishes specific numbers: copays as low as $15 for visits and typical medication costs around $25 every 4 weeks for covered beneficiaries.
Both FDA-approved and compounded fallback paths. If your Medicare plan covers the visit but denies the branded medication, Shapely does not just send you away. It has self-pay programs including compounded options starting at $99, so you have a fallback within the same provider relationship.
Includes dietitian access. For Medicare beneficiaries, dietitian visits billed through Medicare are a meaningful benefit — especially because the Bridge and BALANCE programs both require lifestyle support alongside medication.
Only available in 4 states. Shapely does NOT serve all 50 states. If you live outside CA, FL, NY, or TX, this is not an option for you today.
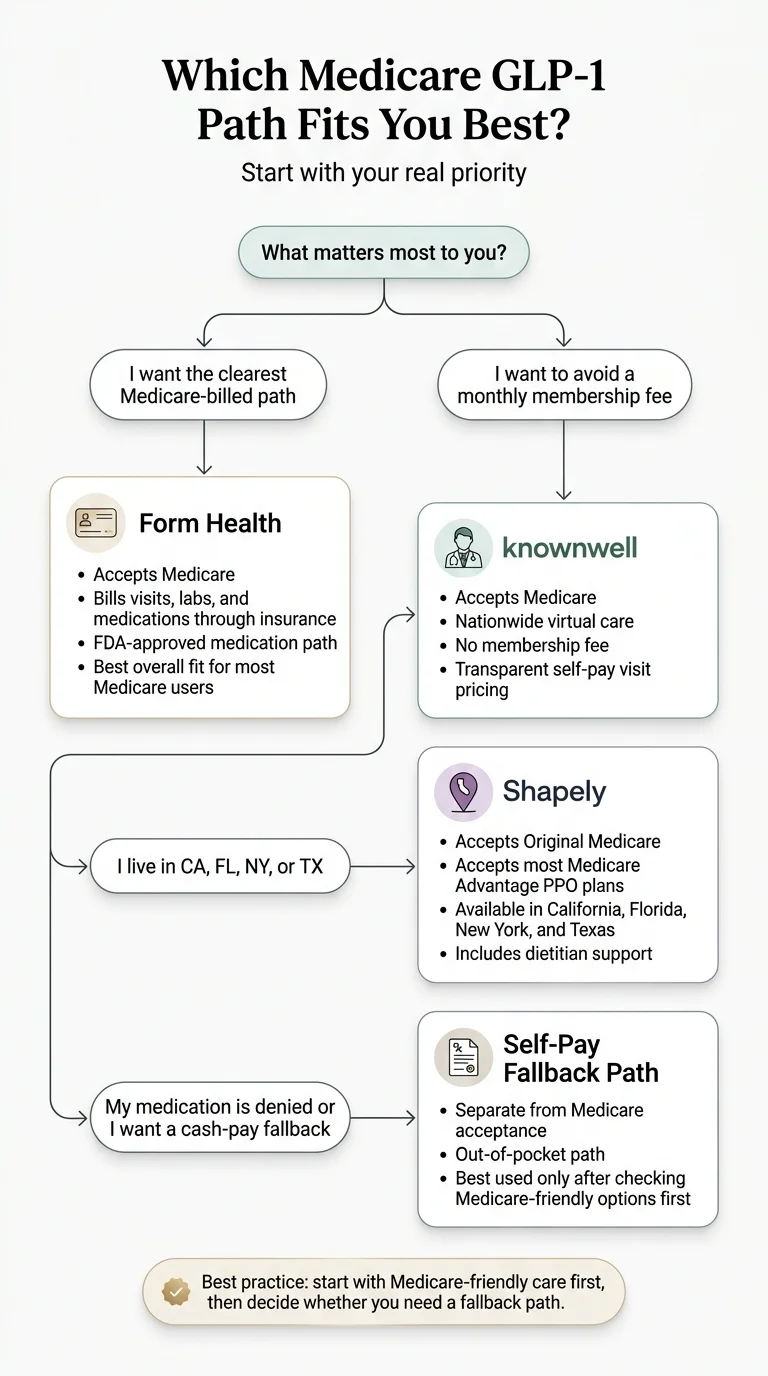
Medicare Acceptance and Medicare Drug Coverage Are Not the Same Thing
This is the section that stops the back-and-forth searching. If you take one thing from this page, make it this:
Visit Side
"Accepts Medicare" means the provider bills your Medicare plan for clinical visits
The doctor appointment, lab orders, dietitian consultations. This is the visit side. Form Health, knownwell, and Shapely pass this test.
Medication Side
"Medicare covers the drug" means Part D pays for the actual medication
Wegovy, Zepbound, Ozempic, or Mounjaro. This requires separate prior authorization, separate approval criteria, and a formulary check. This is where most people hit a wall.

Does Medicare Cover Wegovy, Zepbound, Ozempic, or Mounjaro in 2026?
Under standard Part D rules as of April 2026, Medicare still does not cover GLP-1 medications prescribed solely for weight loss. The exceptions are specific FDA-approved indications and the temporary Medicare GLP-1 Bridge launching July 1, 2026. Here is the drug-by-drug breakdown:
Medicare GLP-1 Drug Coverage Matrix — April 2026
| Medication | Covered by Standard Part D? | Covered by GLP-1 Bridge ($50/mo)? | For What Indication? |
|---|---|---|---|
| Wegovy (semaglutide injection + oral tablet) | Only for cardiovascular risk reduction in adults with established CVD who are overweight/obese | Yes — for weight loss in eligible beneficiaries | CVD risk reduction (Part D) or weight loss (Bridge) |
| Zepbound KwikPen (tirzepatide injection) | Only for moderate-to-severe obstructive sleep apnea in adults with obesity | Yes — for weight loss in eligible beneficiaries | Sleep apnea (Part D) or weight loss (Bridge) |
| Foundayo (orforglipron — oral pill, FDA-approved April 1, 2026) | Not covered for weight loss under standard Part D exclusion | Yes — added to Bridge as of April 6, 2026 | Weight loss (Bridge pathway only) |
| Ozempic (semaglutide injection) | For Type 2 diabetes management | No — not included in Bridge | Type 2 diabetes only |
| Mounjaro (tirzepatide injection) | For Type 2 diabetes management | No — not included in Bridge | Type 2 diabetes only |
| Any compounded GLP-1 | Never covered | Never covered | N/A — not FDA-approved |
Sources: CMS Medicare GLP-1 Bridge FAQ (cms.gov, updated April 6, 2026), FDA drug approval pages, KFF analysis (March 2026), Eli Lilly Foundayo approval announcement.
What This Means in Plain English
If you have Type 2 diabetes: Your Part D plan likely already covers Ozempic or Mounjaro. Weight loss is a documented benefit even though the prescription is written for diabetes. You may not need the Bridge at all.
If you have cardiovascular disease and are overweight/obese: Wegovy may be coverable under your Part D plan right now for CVD risk reduction. This is a standard Part D benefit, not the Bridge.
If you have moderate-to-severe obstructive sleep apnea with obesity: Zepbound may be coverable under your Part D plan right now — standard benefit, not the Bridge.
If you want a GLP-1 specifically for weight loss without those conditions: The Bridge program starting July 1, 2026 is your first realistic Medicare pathway. Until then, cash-pay is your only option.
If you want compounded semaglutide or tirzepatide: Medicare will not cover it. Period. Not under Part D, not under the Bridge, not under BALANCE in 2027. Compounded medications have not undergone the FDA approval process required for Medicare coverage.
What Is the Medicare GLP-1 Bridge, and Who Qualifies?
The Medicare GLP-1 Bridge is a temporary CMS demonstration program running from July 1, 2026 through December 31, 2026. It is the first time in over 20 years that Medicare has covered any prescription medication specifically for weight loss. Eligible beneficiaries pay a flat $50/month copay for Wegovy, Zepbound KwikPen, or Foundayo.
Bridge Program Quick Facts
| Detail | What You Need to Know |
|---|---|
| Dates | July 1 – December 31, 2026 |
| Drugs covered | Wegovy (injection + oral tablet), Zepbound KwikPen, Foundayo (orforglipron — added April 6, 2026) |
| Your cost | $50/month flat copay |
| Who runs it | CMS, with Humana as the central processor — NOT your Part D plan |
| Enrollment needed? | No separate enrollment. You must be in a qualifying Part D PDP or MA-PD coordinated-care plan. |
| Prior authorization? | Yes — your doctor submits PA to the CMS central processor, not to your Part D plan |
| Telehealth allowed? | Yes — the prescribing provider does not need to be enrolled in Medicare, just not on the Preclusion List |
| After December 2026? | BALANCE Model begins Jan 2027 for participating Part D plans — check your plan during Open Enrollment |
Source: CMS Medicare GLP-1 Bridge FAQ (cms.gov, updated April 6, 2026).
Who Qualifies — The Actual CMS Criteria
Most articles simplify the Bridge eligibility criteria. You must be on a qualifying Part D plan, age 18+, currently on or willing to start lifestyle modification, AND meet one of these three clinical thresholds at the time GLP-1 therapy was initiated:
Threshold 1
BMI ≥ 35 at GLP-1 initiation — qualifies on its own
Threshold 2
BMI ≥ 30 at GLP-1 initiation PLUS heart failure with preserved ejection fraction (HFpEF), uncontrolled hypertension, or chronic kidney disease stage 3a or higher
Threshold 3
BMI ≥ 27 at GLP-1 initiation PLUS prediabetes, prior myocardial infarction (heart attack), prior stroke, or symptomatic peripheral artery disease
Critical detail most articles miss:
Another detail most articles miss:
What the $50 Copay Does NOT Do
The Bridge Timeline You Need to Follow
| When | What to Do |
|---|---|
| Now (April 2026) | Verify Part D enrollment. Schedule a doctor visit. Get your BMI documented. Discuss Wegovy, Zepbound, or Foundayo with your provider. |
| May–June 2026 | Ask your provider to prepare the prior authorization paperwork for the CMS central processor. Final PA guidance expected Spring 2026. |
| July 1, 2026 | Bridge launches. Fill your first prescription at $50/month. |
| Oct 15–Dec 7, 2026 | Open Enrollment. Check whether your Part D plan participates in the BALANCE Model for 2027. If not, consider switching. |
| Dec 31, 2026 | Bridge ends. |
| Jan 1, 2027 | BALANCE Model begins for participating plans. |
Think you qualify for the Bridge? The smartest move right now is scheduling a visit with Form Health or knownwell to get your documentation ready before July.
Original Medicare vs. Medicare Advantage: Which Is Easier for GLP-1 Access?
| Plan Type | Bridge Eligible? | Notes |
|---|---|---|
| Original Medicare + standalone PDP | Yes | Maximum provider flexibility — any Medicare-accepting provider |
| Medicare Advantage PPO with drug coverage (MA-PD) | Yes | May allow out-of-network telehealth at higher cost-sharing |
| Medicare Advantage HMO with drug coverage (MA-PD) | Yes | More restrictive networks — confirm provider is in-network |
| Original Medicare WITHOUT Part D | No | Must have Part D drug coverage to qualify |
| Medicare Supplement (Medigap) only | No | Medigap does not include drug coverage |
Source: CMS Medicare GLP-1 Bridge FAQ (cms.gov, April 2026). Verify your specific plan type's eligibility.
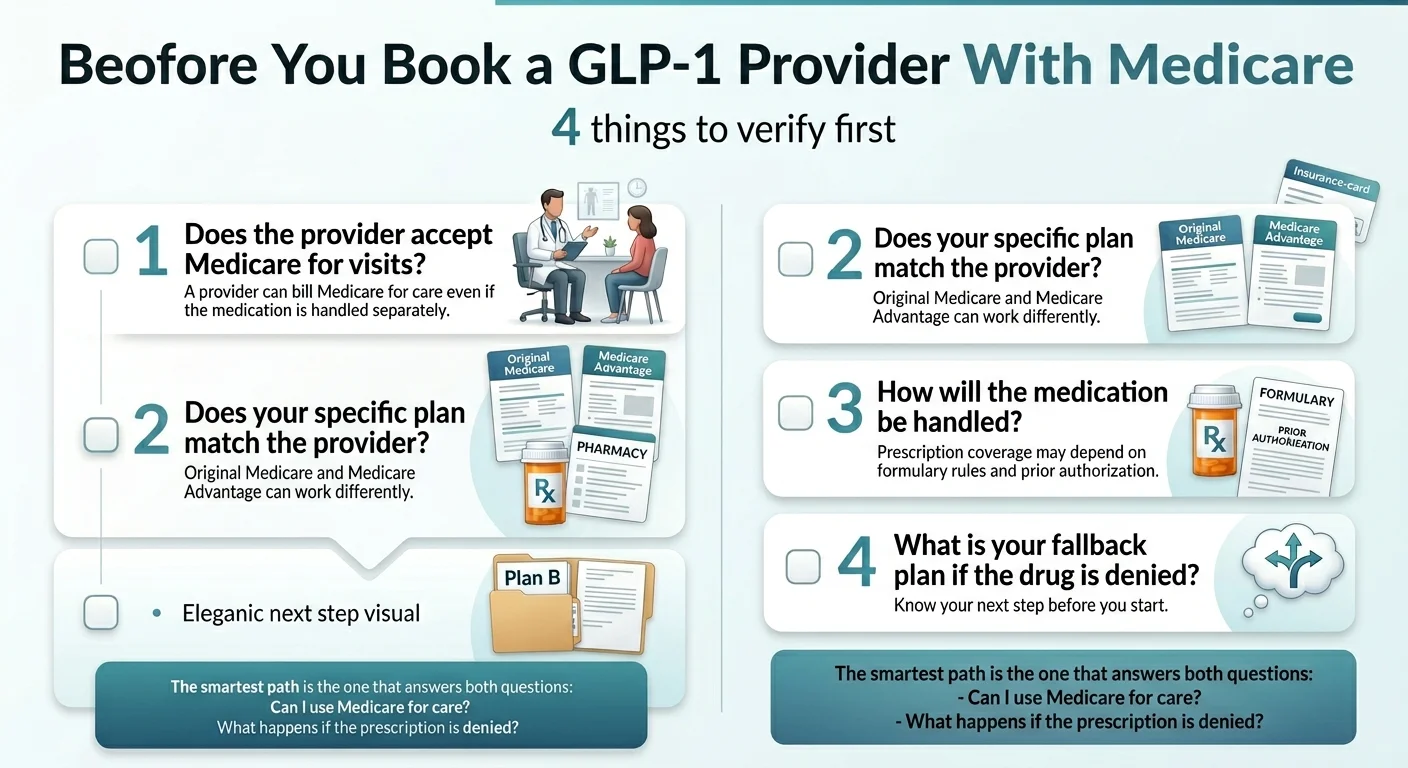
The Bridge itself works the same regardless of your Medicare flavor — $50/month, same drugs, same central processor. The difference is on the visit side: check whether your specific plan covers the specific provider you want to use. Call the provider's insurance line before your first appointment. Shapely specifically calls out Medicare Advantage PPO acceptance in its four states — a clean match if you have an MA PPO in CA, FL, NY, or TX.
What Happens If Your Provider Accepts Medicare but Your Medication Is Denied?
This is where most people give up and start the whole search over. A medication denial does not mean the end of the road. It means you need to figure out why it happened and what to do next.
The 4 Most Common Denial Reasons
Wrong indication. Your prescription was written for "weight loss" but your Part D plan only covers the drug for diabetes, CVD risk reduction, or sleep apnea. This is the most common barrier. The Bridge program (July 2026) was designed specifically to close this gap.
Formulary exclusion. The specific drug is not on your Part D plan's formulary. Every plan has a different drug list. Just because Wegovy exists does not mean your plan covers it.
Prior authorization not submitted or incomplete. Many denials are paperwork failures, not medical ones. Incomplete submissions — missing BMI documentation, missing comorbidity records, missing lifestyle modification attestation — are a leading cause. This is where having a provider with PA experience makes a measurable difference.
Step therapy requirement. Your plan requires you to try a less expensive medication first before approving the one you want.
Your Denial Response Playbook
Step 1: Read the denial letter.
It will state the specific reason. Do not guess.
Step 2: Gather your documentation.
BMI history (current and at therapy initiation), list of qualifying comorbidities with diagnostic codes, evidence of previous weight loss attempts, and your provider's clinical notes supporting medical necessity.
Step 3: Decide your next move.
- If it is an indication issue and the Bridge is live: Ask your provider to resubmit through the Bridge pathway.
- If it is a formulary issue: Ask your provider to request a formulary exception — you have the right to this under Part D rules.
- If it is a PA failure: Resubmit with complete documentation. Consider switching to a provider with dedicated PA support.
- If it is a step therapy issue: Ask your doctor whether trying the required first-step drug makes clinical sense. If not, request a step therapy exception.
Step 4: If the appeal fails,
move to one of the self-pay fallback paths below. That does not mean you failed — it means the system was not built for your specific case yet.
For a deeper walkthrough on prior authorization timelines and appeal strategies: our prior authorization guide →
Which Popular Online GLP-1 Providers Do NOT Accept Medicare?
These are legitimate providers with real patients — they just are not the right answer for people searching for GLP-1 providers that accept Medicare.
Ro — Cash-pay membership, not a true Medicare path
Ro explicitly states it cannot coordinate GLP-1 coverage for government insurance plans, including Medicare and Medicaid. Its Body Program membership is cash-pay: $39 for the first month, then $149/month ongoing. Medicare beneficiaries can join Ro and pay out of pocket, but Ro will not bill Medicare or navigate Medicare coverage.
Provider says: Cannot coordinate government insurance for GLP-1 coverage. Medicare users can join and pay cash for certain options. Verified: Confirmed on Ro's insurance FAQ (ro.co) as of April 9, 2026.
PlushCare — Medicare Part B no longer accepted
PlushCare dropped Medicare Part B acceptance as of January 1, 2026. Some Medicare Advantage plans may still be accepted, but the policy is narrow enough that we cannot recommend it as a reliable Medicare path. If you have an MA plan, call PlushCare directly to verify before booking.
Walgreens Virtual Weight Management — Not built for Medicare users
Walgreens lists its weight management visit as a $49 self-pay service for ages 18–64 and explicitly does not handle insurance or prior authorizations. Medicare beneficiaries are typically 65+, and the lack of insurance billing and PA support makes this the wrong doorway.
LifeMD — Mixed signals on Medicare
LifeMD's support pages present conflicting information. One page states it accepts Medicare Fee-For-Service for qualifying virtual care in some states; another page says it does not accept insurance for its GLP-1 weight loss programs. Because the messaging is contradictory, we cannot list LifeMD as a clear Medicare path. Contact them directly and get written confirmation before booking.
MEDVi — Cash-pay compounded only
MEDVi operates on a direct cash-pay model. Compounded semaglutide starts at $179 for the first month, with refills at $299/month. It does not accept Medicare or any insurance. It is a legitimate option for people who want compounded treatment and are comfortable paying out of pocket — but it is a self-pay fallback, not a Medicare answer.
Eden — Cash-pay, not enrolled with Medicare
Eden's terms of service state it is not enrolled with federal or state programs including Medicare and Medicaid. All services are cash-pay.
TrimRx — Cash-pay compounded, no Medicare billing
TrimRx has published that compounded medications are generally not covered by Medicare and that its program operates on a direct-to-patient cash-pay model. Compounded semaglutide starts at $199/month.
SkinnyRx — Cash-pay, not enrolled in Medicare
SkinnyRx's terms state that it and its affiliated providers are not enrolled in Medicare or Medicaid and do not accept health insurance. All services are cash-pay.
If Medicare Won't Cover Your Medication: The Best Fallback Paths
You have done everything right — picked a Medicare-friendly provider, submitted the prior authorization, maybe even appealed — and the answer is still no. Or maybe July 2026 feels too far away. Here are your options, organized by what matters most to you.
Medicare Beneficiary Self-Pay Fallback Matrix
| Fallback Path | Monthly Cost | Medication Type | Medicare Users Eligible? | Notes |
|---|---|---|---|---|
| Wegovy oral tablet (NovoCare self-pay) | $149/mo (1.5mg–4mg doses) | FDA-approved | Government beneficiaries excluded | Novo Nordisk terms explicitly exclude Medicare patients even when self-paying |
| Wegovy pen via Ro (cash-pay) | $199 first mo, $199–$349 thereafter + $39/$149 membership | FDA-approved | Can join Ro and pay cash | Ro cannot bill Medicare but allows cash-pay enrollment |
| MEDVi compounded | $179 first mo, $299/mo refills | Compounded (not FDA-approved) | Cash-pay, no insurance check | Lowest entry-point for compounded among major providers |
| TrimRx compounded | From $199/mo | Compounded (not FDA-approved) | Cash-pay | Direct-to-patient model |
| Shapely compounded fallback | From $99/mo | Compounded (not FDA-approved) | Available as fallback within Shapely | Only in CA, FL, NY, TX |
| Medicare GLP-1 Bridge (July 2026) | $50/mo | FDA-approved (Wegovy, Zepbound KwikPen, Foundayo) | If you meet eligibility criteria | Temporary: July 1 – Dec 31, 2026 |
All pricing verified April 9, 2026. Pricing may change — verify directly with providers before committing.
The NovoCare exclusion you need to know about:
If You Want FDA-Approved Medication at Cash-Pay Pricing
Ro Body Program: Medicare beneficiaries can join Ro and pay cash. Wegovy pen is $199 for the first month, then $199–$349/month depending on dose, plus Ro's membership ($39 first month, $149/month ongoing). Currently the most accessible FDA-approved cash-pay path for Medicare patients, since Ro does not run NovoCare eligibility checks that would exclude government beneficiaries.
If Budget Is the Priority and You Understand the Compounded Tradeoff
With that clearly stated — for Medicare beneficiaries on a fixed income who cannot afford $344–$494/month for branded Wegovy through Ro and cannot wait until July for $50/month Bridge pricing, compounded programs offer a significantly lower entry point.
MEDVi — Best Compounded Cash-Pay Fallback
Lowest Entry PriceNo Insurance Required$179 first month · $299/mo refills · Month-to-month · No contracts
MEDVi starts at $179 for the first month of compounded semaglutide, with refills at $299/month. Month-to-month billing, no contracts. It does not accept Medicare or any insurance. But for Medicare beneficiaries who need to start before July 2026 and can't afford branded pricing, it is the lowest verified entry price among major compounded providers.
Important: MEDVi offers compounded semaglutide, not FDA-approved brand-name medications like Wegovy or Zepbound. Compounded medications are not FDA-approved and will never be covered by Medicare.
If you need to start before July and budget matters → Check MEDVi ($179 first month)Other Cash-Pay Compounded Alternatives
TrimRx
Compounded semaglutide from $199/month. Direct-to-patient model, no insurance requirement. Verify current pricing at trimrx.com.
Eden
Both compounded and FDA-approved medication options available. Cash-pay, no insurance billing. Verify current pricing at edentelemed.com.
SkinnyRX
Budget-focused compounded semaglutide. Cash-pay, straightforward pricing. Verify at skinnyrx.com.
How to Prepare for the Medicare GLP-1 Bridge Right Now
The Bridge does not launch until July 1, 2026. But the beneficiaries who fill their first prescription on day one will be the ones who prepared in April, May, and June. Here is your action plan:
Verify your Part D enrollment (5 minutes).
Log into Medicare.gov or call 1-800-MEDICARE (1-800-633-4227). Confirm you are enrolled in a qualifying PDP or MA-PD plan for 2026.
Schedule a doctor visit this month.
See your PCP or a Medicare-accepting GLP-1 telehealth provider (Form Health, knownwell, or Shapely). Get your BMI measured and documented, discuss your weight history and qualifying comorbidities, tell your doctor you want to be ready for the Bridge, and ask your doctor to note your BMI at therapy initiation if you have used a GLP-1 previously.
Build your prior authorization file (May 2026).
Gather: current BMI measurement, BMI at therapy initiation (if applicable), diagnostic records for qualifying comorbidities, documentation of lifestyle modification, and your provider's clinical notes supporting medical necessity.
Watch for CMS Spring 2026 updates.
Final PA guidance, appeals process details, and operational information are expected soon. Check the CMS Bridge page or ask your provider.
Plan for 2027 now.
During Open Enrollment (October 15 – December 7, 2026), check whether your Part D plan participates in the BALANCE Model. BALANCE is voluntary — not every plan will join. If yours does not, consider switching to maintain GLP-1 weight loss coverage without a gap.
Get your documentation ready before July — start with a Medicare-accepting provider:
What Happens After the Bridge Ends in December 2026?
The Bridge is temporary — six months. After December 31, 2026, your GLP-1 weight loss coverage depends on the BALANCE Model.
BALANCE (Better Approaches to Lifestyle and Nutrition for Comprehensive Health) is a CMS Innovation Center demonstration model, not a permanent benefit change. It launches in Medicare Part D in January 2027 for plans that choose to participate.
How We Verified These Providers
Sources used: CMS.gov (Medicare GLP-1 Bridge FAQ, BALANCE Model page), FDA drug approval pages, Eli Lilly investor announcements, KFF analysis (March 2026), and each provider's current public-facing insurance/FAQ/pricing pages as of April 9, 2026.
Score rubric: The Medicare Compatibility Score is our editorial assessment based on the 100-point rubric published in the comparison table. It reflects how well each provider serves someone searching for "GLP-1 providers that accept Medicare" — not a general quality rating.
What "Last verified" means: Every data point in the comparison matrix was checked against the provider's live website on April 9, 2026. We re-verify monthly through 2026 and immediately after any CMS, FDA, or provider policy change.
What we did NOT do: We did not use fake review schema, star ratings without real data, or aggregated scores from unverified platforms. Testimonials are clearly labeled as patient stories from provider websites.
Related Guides & Comparisons
- GLP-1 Providers That Accept Medicaid: 2 Verified Options (2026)
- Best GLP-1 Cash Pay Programs: 7 Real Picks (April 2026)
- GLP-1 Providers With Flat-Rate Pricing — 7 Options Compared
- Month-to-Month GLP-1 Providers: 8 Options Compared
- Semaglutide Providers That Accept HSA: 9 Verified Options
- Tirzepatide Providers That Accept HSA: 8 Verified Options
- Best GLP-1 Pill Provider 2026: Wegovy Pill, Foundayo & Rybelsus Compared
- Ozempic Cost Without Insurance: Real Prices Verified
- GLP-1 Providers That Accept Afterpay: 6 Verified Options
- GLP-1 Providers That Accept CareCredit: 7 Verified Options
- MEDVi vs Henry Meds: 7 Real Differences Compared
Frequently Asked Questions: GLP-1 Providers & Medicare
Your Next Step
You now know the verified list: Form Health, knownwell, and Shapely are the only three online GLP-1 providers that clearly bill Medicare for clinical visits. The Bridge program opens July 1 at $50/month. Your preparation window is right now.
For the clearest Medicare-billed path:
If insurance is a dead end and you need to start now:
Check MEDVi — $179 first month, no Medicare requiredAffiliate Disclosure
Weight Loss Provider Guide is an independent comparison resource for GLP-1 telehealth providers. We may earn a commission when you visit a provider through our links, at no additional cost to you. Our editorial assessments are based on publicly available information verified on the dates noted. We do not accept payment for higher rankings or scores. Not all providers listed are affiliate partners — Form Health, knownwell, and Shapely are not affiliate partners and are included because they are the verified answer to this query.
This content is for informational purposes only and does not constitute medical advice. Always consult your healthcare provider before starting or changing any medication. Medicare coverage rules, provider policies, and pricing can change — verify current details directly with your provider and plan before making decisions.
Last Verified: April 9, 2026 · Pricing Verified: April 9, 2026