GLP-1 Providers That Accept Medicaid: Verified Online Options for 2026
By Weight Loss Provider Guide Editorial Team · Last verified: April 9, 2026
Weight Loss Provider Guide is an independent comparison resource for GLP-1 telehealth providers. We may earn a commission when you use our partner links — this never influences our rankings or recommendations. Full disclosure below.
Bottom line:
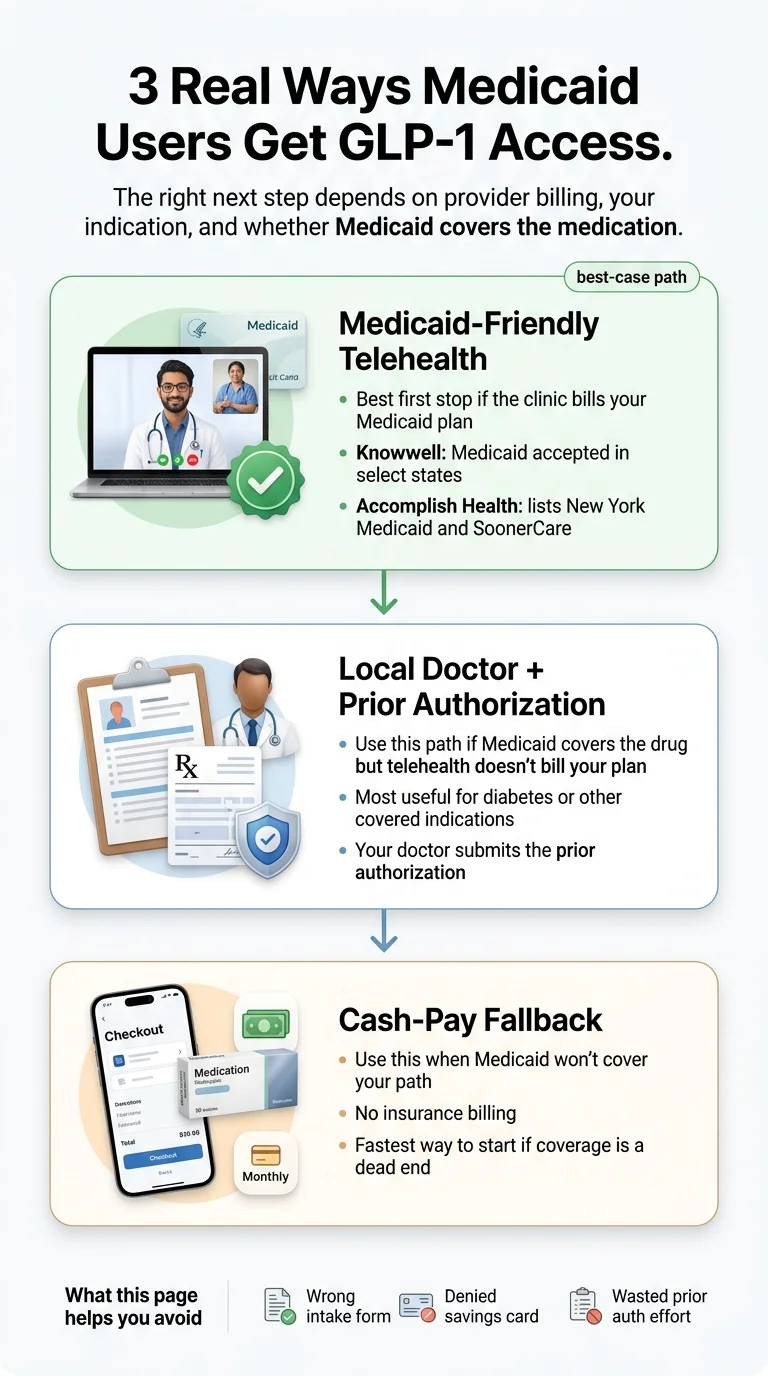
Most national GLP-1 telehealth brands — including Ro, Hims/Hers, MEDVi, and PlushCare — do not accept Medicaid. We checked the insurance pages of 12 major online GLP-1 providers and found only two with clearly documented Medicaid billing paths: knownwell (Medicaid accepted in select states via the Lilly telehealth network) and Accomplish Health (explicitly lists New York Medicaid and SoonerCare/Oklahoma Medicaid). A third, Form Health, has contradictory information on its own pages and should be verified directly.
If those two paths don't work for your state or plan, this page maps the next moves: prior authorization with your local doctor, the three Medicaid-specific coverage indications that work in all states, and the most affordable cash-pay alternatives.
If you're on Medicaid and searching for GLP-1 providers that accept Medicaid, you're running into a wall that isn't your fault. The GLP-1 telehealth market was built for cash-pay and commercial insurance customers. But that doesn't mean you're stuck — it means you need a different map.
This page gives you that map. We cover the few providers that actually bill Medicaid, the states where Medicaid covers GLP-1 medications for weight loss (only 13 fee-for-service programs as of January 2026, per KFF), how to get prior authorization if your indication qualifies, and the most affordable cash-pay alternatives if your state or plan says no.
Jump to section
- Which Providers Accept Medicaid?
- 3 Things Most Pages Confuse
- Does Your State Cover GLP-1s?
- The BALANCE Model: What's Coming
- Which Lane Is Right for You?
- Best Cash-Pay Alternatives
- How to Get Prior Authorization
- Savings Cards & Medicaid: The Answer
- States That Cut GLP-1 Coverage
- knownwell vs Accomplish Health
- FAQ: 11 Questions Answered
Which GLP-1 Providers That Accept Medicaid Can You Actually Use?
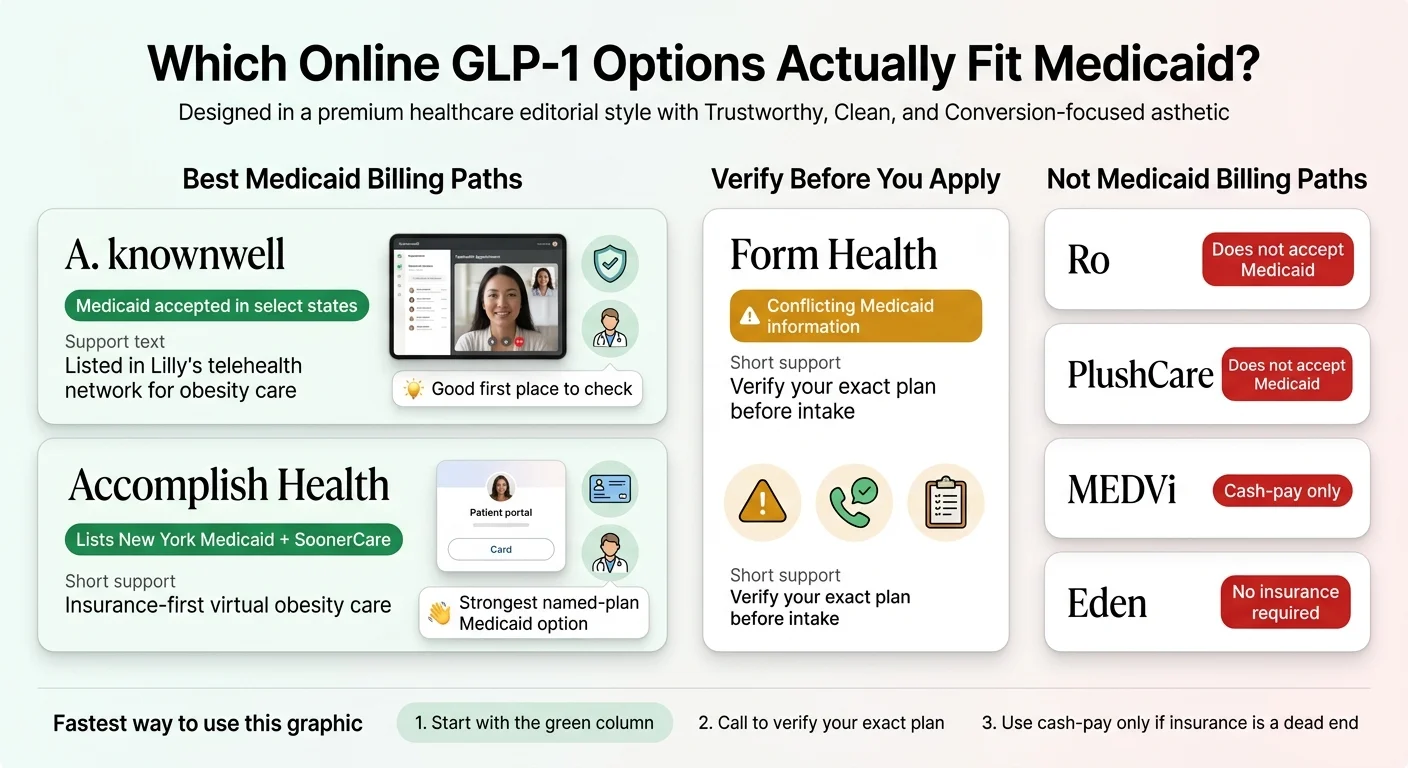
Very few. And that's the first thing most pages about this topic fail to say clearly enough. We checked the public insurance pages, FAQ sections, and terms of service for 12 of the most-searched GLP-1 telehealth providers. Here is what we found as of April 2026.
Providers With Documented Medicaid Billing Paths
| Provider | Medicaid Accepted? | Documented States/Plans | What They Offer | Source |
|---|---|---|---|---|
| knownwell | Yes — select states | Medicaid marked "Yes" in at least 4 states on the Lilly telehealth directory (appears to include MA, NH, RI, TX) — [NEEDS VERIFICATION — confirm directly with knownwell] | Insurance-first obesity care, brand-name FDA-approved GLP-1s | Lilly telehealth directory |
| Accomplish Health | Yes — specific named plans | New York Medicaid and SoonerCare (Oklahoma Medicaid) explicitly listed; also Aetna, BCBS, Cigna, UHC, Medicare | Insurance-billed obesity medicine, brand-name GLP-1s | accomplish.health/insurance |
A critical note on knownwell's Medicaid states:
Conflicting Medicaid Information — Verify Directly
| Provider | Status | What We Found | Our Recommendation |
|---|---|---|---|
| Form Health | Contradictory | One page says Form "does not accept Medicaid" for program costs. A separate consent page says Form may bill insurance payers "including Medicare or Medicaid." | Call Form Health directly with your specific state and Medicaid MCO name before intake. Do not assume they accept your plan. |
Source: formhealth.co — multiple pages conflict as of April 2026.
Providers That Do NOT Accept Medicaid
This table exists to save you time. If your core requirement is "bills my Medicaid plan directly," these popular GLP-1 brands are not the answer.
| Provider | Accepts Medicaid? | What Their Site Says | What They Are |
|---|---|---|---|
| Ro | No | "If you have Medicaid or any government-funded plan, you can't join the Ro Body membership or pay out of pocket through Ro" | FDA-approved GLP-1s via insurance concierge (commercial plans only) — source |
| PlushCare | No | "Medicaid is not currently accepted" | Telehealth primary care, some GLP-1 prescribing — source |
| MEDVi | No | "Our providers are not contracted with any health insurance plan, including Medicaid and Medicare" | Cash-pay compounded GLP-1 telehealth — source |
| Eden | No | "No insurance required, no co-pays or deductibles" | Cash-pay GLP-1 telehealth (compounded and FDA-approved) — source |
| Hims / Hers | No | Membership-based cash-pay model, insurance not billed | Cash-pay GLP-1 telehealth — source |
| TrimRx | No | "Does not accept Medicaid or any other insurance" | Cash-pay compounded GLP-1 telehealth — source |
| SkinnyRX | No | Cash-pay model, no insurance billing | Cash-pay compounded GLP-1 telehealth — source |
If your state has a Medicaid-friendly provider path:
Start with knownwell or Accomplish Health to verify they are in-network with your specific Medicaid MCO.
The 3 Things Most Pages Confuse About Medicaid and GLP-1s
Here's why this search is so frustrating: there are three separate questions that most pages — and most providers — mash together into one unhelpful answer.
Question 1: Does the provider accept Medicaid billing?
This is what you actually searched for. As shown above, the answer is almost always no for national telehealth GLP-1 brands. Only knownwell and Accomplish Health have documented Medicaid billing paths.
Question 2: Does your state Medicaid program cover GLP-1 medications for weight loss?
This is a completely different question. Even if a provider accepts Medicaid, your state program might not cover the medication for your indication. As of January 2026, only 13 state Medicaid fee-for-service (FFS) programs cover GLP-1s for obesity/weight loss — down from 16 in late 2025, after California, Pennsylvania, New Hampshire, and South Carolina cut coverage.
Question 3: Does your medical indication qualify for coverage?
All state Medicaid programs must cover GLP-1s for medically accepted indications like Type 2 diabetes. And since March 2024, Wegovy has an FDA-approved indication for cardiovascular risk reduction in patients with established heart disease — which follows different coverage logic than weight loss. Since December 2024, Zepbound is approved for obstructive sleep apnea. And since August 2025, Wegovy is approved for MASH (metabolic dysfunction-associated steatohepatitis).
These three layers explain why someone in New York with Type 2 diabetes can get Ozempic through Medicaid with minimal hassle, while someone in Texas with obesity alone can't get Wegovy — even though both are GLP-1 medications. Understanding which layer is blocking you determines your next move.
Does Medicaid Cover GLP-1 Medications in Your State? The 2026 Reality
Only 13 state Medicaid fee-for-service programs covered GLP-1 medications specifically for the treatment of obesity as of January 2026, according to KFF. That number has been shrinking, not growing — four states eliminated obesity-related GLP-1 coverage between October 2025 and January 2026.
States Covering GLP-1s for Obesity Under Medicaid FFS (January 2026)
| Coverage Tier | States | Key Details |
|---|---|---|
| Full obesity coverage (Wegovy + Zepbound and/or Saxenda) | Connecticut, Iowa, Kentucky, Michigan, Minnesota, North Carolina, West Virginia, and others [KFF confirms 13 total — verify your state PDL directly] | Coverage criteria vary — most require BMI ≥30 (or ≥27 with comorbidities) and prior authorization |
| Recently reinstated | North Carolina | Cut in Oct 2025 due to budget stalemate; reinstated Dec 2025 with Wegovy as preferred, Zepbound and Saxenda as non-preferred |
| Restricted obesity coverage | Michigan | Limited to "morbidly obese" with step therapy — must try and fail other interventions before GLP-1 approval |
Source: KFF Medicaid GLP-1 tracking (January 2026). We were unable to locate one definitive public list of all 13 states from a single source — if your state isn't listed, search "[your state] Medicaid preferred drug list 2026" to check your formulary directly.
States That Recently Cut GLP-1 Obesity Coverage
| State | What Changed | Effective | What's Still Covered |
|---|---|---|---|
| California (Medi-Cal) | Eliminated all GLP-1 coverage for weight loss, adults 21+ | Jan 1, 2026 | Diabetes, CV risk reduction, sleep apnea, MASH; under-21 via EPSDT |
| Pennsylvania | Ended adult GLP-1 coverage for weight loss | Jan 1, 2026 | Diabetes, other FDA-approved indications; under-21 via EPSDT |
| New Hampshire | Eliminated obesity GLP-1 coverage | Late 2025 | Diabetes and other approved indications |
| South Carolina | Eliminated obesity GLP-1 coverage | Late 2025 | Diabetes and other approved indications |
What Every State's Medicaid DOES Cover
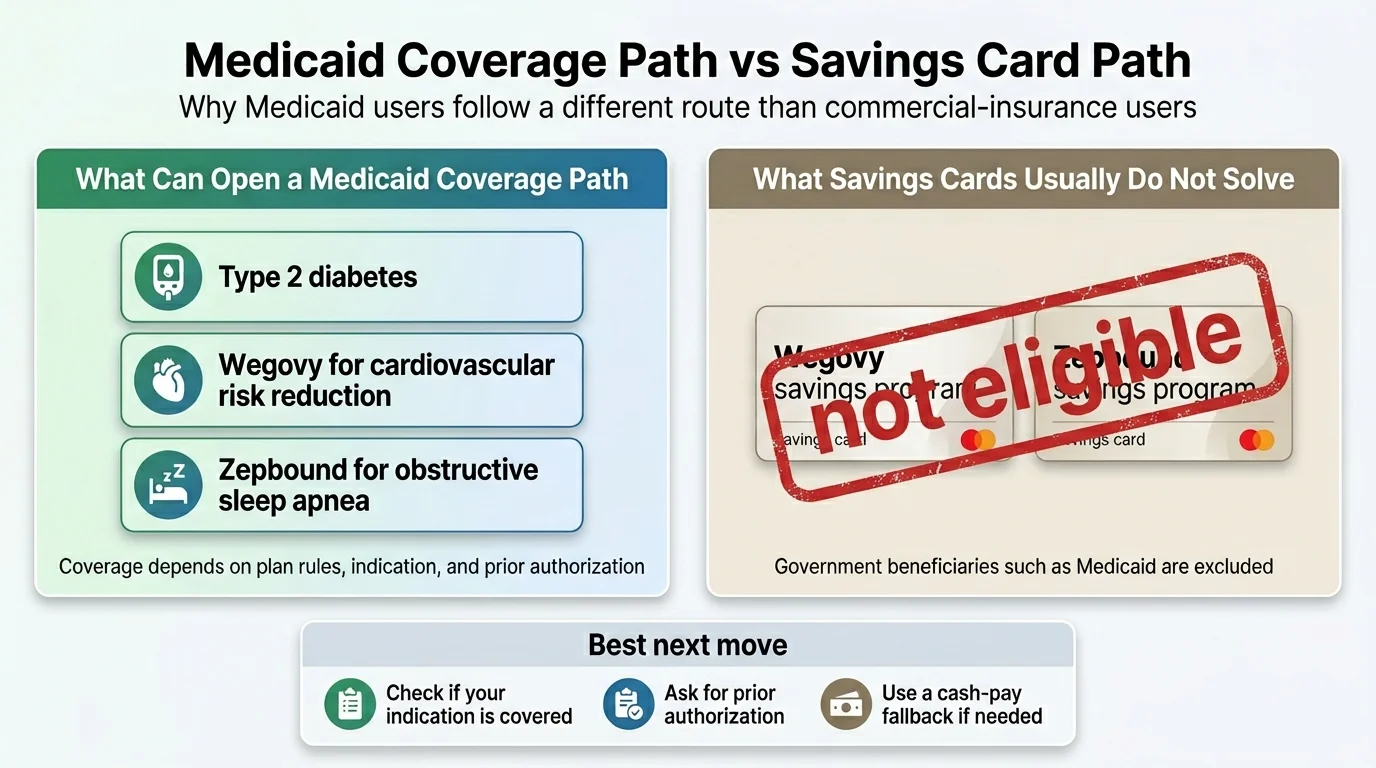
Regardless of where you live, your Medicaid program must cover GLP-1s for medically accepted FDA-approved indications beyond weight loss. That includes:
Type 2 diabetes: Ozempic, Mounjaro, Rybelsus, and others are covered when prescribed for blood sugar management, though specific product availability varies by state formulary.
Cardiovascular risk reduction: Wegovy is approved to reduce the risk of major adverse cardiovascular events in patients with established CV disease (heart attack, stroke, coronary artery disease) plus obesity/overweight — per the March 2024 FDA approval based on the SELECT trial.
Obstructive sleep apnea: Zepbound is approved for moderate-to-severe OSA in adults with obesity, per the December 2024 FDA approval.
MASH (metabolic dysfunction-associated steatohepatitis): Wegovy was approved for MASH in August 2025. If your doctor has diagnosed MASH alongside obesity, this may open a coverage pathway even in states that exclude weight-loss-only indications.
This matters enormously. If you have a qualifying condition beyond obesity alone, your path to a GLP-1 through Medicaid may already be open — regardless of your state's obesity coverage policy. Ask your doctor whether any of these indications apply to your medical history.
If you're in a state that covers GLP-1s for obesity and want an insurance-first online clinic:
If your state doesn't cover obesity but you have diabetes, heart disease, sleep apnea, or MASH: Talk to your doctor about prescribing for your covered indication — see our prior authorization section below.
The BALANCE Model: Could Medicaid GLP-1 Coverage Expand in Your State?
The biggest potential shift in Medicaid GLP-1 access is the BALANCE Model (Better Approaches to Lifestyle and Nutrition for Comprehensive hEalth) — a voluntary CMS Innovation Center program that allows state Medicaid programs to cover GLP-1s for weight management at government-negotiated prices.
BALANCE Model Timeline
| Date | What's Happening | Impact on Medicaid GLP-1 Access |
|---|---|---|
| February 2026 | CMS completed manufacturer pricing negotiations with Eli Lilly and Novo Nordisk | Negotiated prices locked in for participating states |
| April 1, 2026 | FDA approved Foundayo (orforglipron), oral GLP-1 pill | First daily oral GLP-1 — included in BALANCE negotiations |
| May 2026 | BALANCE Model opens to first participating state Medicaid programs | Could add GLP-1 obesity coverage in new states at negotiated prices |
| July 1, 2026 | Medicare GLP-1 Bridge launches ($50/month copay) | Doesn't directly affect Medicaid, but signals federal commitment to access expansion |
| July 31, 2026 | Deadline for state Medicaid BALANCE applications | After this date, participating vs non-participating states become clearer |
| January 2027 | BALANCE launches in Medicare Part D; remaining Medicaid states can join through this date | Broader coverage picture solidifies |
| December 2031 | Model testing concludes | BALANCE is a demonstration program, not permanent legislation |
The catch nobody is saying clearly:
Which Lane Is Right for You?
After checking 12 providers and reviewing the coverage landscape, we have mapped every Medicaid GLP-1 situation into three lanes.
Lane 1: Your State Covers the Drug AND You Have an Insurance-First Provider
Best-case scenario
You live in one of the 13 FFS coverage states (or your MCO covers it), or you have a qualifying non-obesity indication (diabetes, CV disease, sleep apnea, MASH), AND knownwell or Accomplish Health is in-network with your plan.
Your next step: Contact knownwell or Accomplish Health to verify they're in-network with your specific Medicaid MCO. Then work with their team to submit prior authorization.
Who this fits: Medicaid enrollees in New York, Oklahoma (SoonerCare), or one of knownwell's Medicaid states who have a coverable indication.
Lane 2: Your State Covers the Drug BUT No Telehealth Provider Bills Your Plan
More common than Lane 1
Your state Medicaid might cover the medication, but no online GLP-1 clinic accepts your specific MCO.
Your next step: See your primary care doctor or a local obesity medicine specialist. Ask them to prescribe the GLP-1 for your covered indication and submit prior authorization through your Medicaid plan directly. We walk through that process step-by-step below.
Lane 3: Your State Doesn't Cover GLP-1s for Obesity AND Insurance Won't Work
Reality for the majority of Medicaid enrollees
You're in one of the 37+ states that don't cover GLP-1s for weight loss under FFS, you don't have a qualifying alternative indication, and the Medicaid-friendly telehealth providers aren't in your state.
Your next step: Move to cash-pay. Compounded GLP-1 medications through licensed telehealth providers can start under $200/month — a fraction of the $900–$1,300/month brand-name retail price. No prior authorization, no denial letters, no appeals. You can start this week.
See MEDVi's cash-pay pricing — starts under $200/moBest Cash-Pay GLP-1 Options If Medicaid Won't Cover It
Cash-Pay GLP-1 Providers Compared (April 2026)
| Provider | Starting Price | Medication Type | What's Included | Best For |
|---|---|---|---|---|
| MEDVi | From ~$149–$179/mo (verify at medvi.org) | Compounded semaglutide | Licensed provider consultations, monitoring, medication shipped | Best combination of price + structured clinical oversight |
| Eden | From ~$129/mo first month (verify at edentelemed.com) | Compounded and FDA-approved options | Licensed providers, prescription consult, clinical approach | Access to both compounded and FDA-approved medications |
| SkinnyRX | Verify at skinnyrx.com | Compounded semaglutide | Provider consultation, medication | Budget-focused, straightforward |
| TrimRx | From ~$149–$199/mo (verify at trimrx.com) | Compounded semaglutide | Provider visits, medication | Budget alternative |
GLP-1 telehealth pricing changes frequently. Every price above was checked against provider websites in April 2026 but may differ from what you see today. Higher doses cost more than starting doses.
What 'compounded' means:
Why MEDVi Is Our Top Cash-Pay Recommendation
Top Cash-Pay PickNo Insurance Req.Compounded semaglutide · All-in pricing · Ships to your door
MEDVi does not bill any insurance — they're purely cash-pay. But for Medicaid enrollees whose state won't cover GLP-1s, MEDVi offers something that matters: a clear all-in price with licensed medical oversight, no insurance paperwork, no prior auth delays, and medication that ships to your door.
What we like
Pricing includes provider visits and medication together — not separate membership fee + medication + consultation. Simpler when you're already navigating a confusing coverage situation.
Honest trade-off
MEDVi does NOT offer FDA-approved brand-name medications like Wegovy or Zepbound. If having an FDA-approved product is important to you, MEDVi is not your fit.
Here's the reality most people in your situation face: if your Medicaid plan won't cover any GLP-1 for weight loss, and you don't have a qualifying alternative indication, and you've already tried the prior auth route — the practical choice isn't between MEDVi and brand-name Wegovy. It's between starting now and waiting indefinitely. People in exactly this position — insurance said no, doctor said wait — are the ones who benefit most from having a clear, affordable path forward.
Check your eligibility on MEDVi — no insurance requiredOther Cash-Pay Alternatives
Eden
Offers both compounded and FDA-approved medication options, giving readers access to a wider range of treatments than compounded-only platforms. Starting from ~$129 first month. Verify current pricing at edentelemed.com.
SkinnyRX
Straightforward compounded semaglutide platform with a simple fee structure. Good budget option for readers who want no-frills access. Verify current pricing at skinnyrx.com.
TrimRx
Compounded semaglutide starting from ~$149–$199/month depending on plan and commitment. Verify current pricing at trimrx.com before enrolling.
How to Get Prior Authorization for a GLP-1 on Medicaid
If your state covers GLP-1s for your indication, prior authorization (PA) is almost certainly required. PA is not a denial — it's a paperwork gate. Here is how to get through it.
Confirm your drug is on your state's Preferred Drug List (PDL).
Search "[your state] Medicaid preferred drug list" to find your formulary. Preferred drugs (often Wegovy in states that cover obesity) have a smoother approval path. Non-preferred drugs may require trying the preferred option first.
Gather your documentation before your appointment.
Current BMI measurement (BMI ≥30, or ≥27 with comorbidities); documented history of weight management attempts (diet, exercise, behavioral counseling); lab work relevant to your indication (A1C, lipid panel, sleep study, cardiac records, liver enzymes for MASH); list of medications tried and failed with dates.
Have your doctor submit the PA with the strongest possible coding.
Diagnosis coding matters. E66.01 (morbid obesity due to excess calories) plus relevant comorbidity codes is stronger than E66.9 (obesity, unspecified). If you have cardiovascular disease, combining E66 with I25.x (chronic ischemic heart disease) can open the Wegovy-for-CV-risk-reduction pathway — which is a required coverage indication in all states.
Wait 2–10 business days.
Processing times vary by state and by whether you're in fee-for-service or managed care.
If denied, appeal immediately.
Request a peer-to-peer review — a phone call between your doctor and the Medicaid plan's medical reviewer. Many initial denials are reversed at this stage. Appeal deadlines vary by state: California is 10 days; Pennsylvania is 15 days. The sooner you appeal, the better your chances.
For a deeper walkthrough on prior authorization timelines and appeal strategies, see our full guide: Wegovy Prior Authorization: Criteria, Forms & What to Expect →
The Cardiovascular Indication Strategy
This isn't gaming the system — it's using the system as designed. If you have documented cardiovascular disease (prior heart attack, stroke, peripheral artery disease, coronary artery disease) AND obesity or overweight, your doctor can prescribe Wegovy specifically for cardiovascular risk reduction rather than weight loss.
This matters because cardiovascular risk reduction is an FDA-approved indication that Medicaid programs in all states are expected to cover under required-indication rules. A Wegovy prescription coded for CV risk reduction may be approved in states that explicitly deny coverage for the weight-loss-only indication — same medication, same patient, different clinical rationale and documentation. Ask your doctor whether this pathway applies to your medical history.
The MASH Pathway
Since August 2025, Wegovy has been FDA-approved for MASH — a serious liver condition affecting an estimated 6–8 million Americans. If your doctor has diagnosed MASH, this creates another potential coverage pathway through Medicaid even in states that exclude weight loss as a standalone indication. MASH is diagnosed through imaging and/or liver biopsy. Ask your doctor if this pathway applies to your history. This is newer and less tested in the prior authorization system, so expect some friction — but the FDA approval is clear.
Can You Use Manufacturer Savings Cards or Coupons With Medicaid?
No.
This is one of the most common follow-up questions after a Medicaid denial, and the answer is straightforward.
- Wegovy Savings Card: Novo Nordisk's savings program explicitly excludes patients enrolled in Medicare, Medicaid, TRICARE, or any other federal or state healthcare program.
- Zepbound Savings Card: Eli Lilly's savings program similarly excludes government healthcare program beneficiaries.
Why: Federal anti-kickback statutes prohibit manufacturers from offering financial incentives to government healthcare beneficiaries. This is a legal restriction, not a company policy choice.
Is there any manufacturer assistance path? Novo Nordisk operates a Patient Assistance Program (PAP) that may be available to some applicants who are Medicaid-eligible but have received a coverage denial. Contact NovoCare directly at 1-888-693-6626 to ask about eligibility.
What If Your State Just Cut Your GLP-1 Medicaid Coverage?
If you're in California, Pennsylvania, New Hampshire, or South Carolina, this section is for you. All four states eliminated Medicaid GLP-1 coverage for weight loss between late 2025 and January 1, 2026.
California (Medi-Cal)
As of January 1, 2026, Medi-Cal does not cover GLP-1 medications when prescribed for weight loss or weight-related indications for members aged 21 and older. Claims are being denied with Reject Code 70. All previously approved prior authorizations for weight loss GLP-1s expired December 31, 2025.
What's still covered: GLP-1s for Type 2 diabetes, cardiovascular risk reduction, obstructive sleep apnea, MASH, and other FDA-approved non-weight-loss indications. Under-21 members may still qualify through EPSDT.
Your move: If you have a qualifying alternative indication, ask your doctor to resubmit with appropriate ICD-10 coding. If not, bridge to cash-pay while watching for BALANCE Model announcements.
Pennsylvania
Effective January 1, 2026, Pennsylvania Medicaid ended GLP-1 coverage for weight loss for adults 21 and older.
Your move: If you received a discontinuation letter, you have appeal rights. File within 15 days of the letter date to preserve coverage continuation during the appeal. Under-21 patients should appeal any denial immediately — GLP-1s may still be coverable under EPSDT.
Coverage Can Come Back — The North Carolina Example
North Carolina eliminated GLP-1 coverage in October 2025 due to a legislative budget stalemate, then reinstated coverage in December 2025 — with Wegovy restored as a preferred drug. The lesson: state coverage losses aren't always permanent.
In the meantime, you don't have to wait for policy to catch up to your health goals.
What's Coming in 2026 and Beyond
| Date | What's Happening | Impact on Medicaid GLP-1 Access |
|---|---|---|
| April 1, 2026 | FDA approved Foundayo (orforglipron), oral GLP-1 | First daily oral GLP-1 — included in BALANCE negotiations |
| May 2026 | BALANCE Model opens to first state Medicaid programs | Could add GLP-1 obesity coverage in new states at negotiated prices |
| July 1, 2026 | Medicare GLP-1 Bridge launches ($50/month copay) | Signals federal commitment to GLP-1 access expansion |
| July 31, 2026 | Deadline for state Medicaid BALANCE applications | Participating vs non-participating states become clearer |
| January 2027 | BALANCE launches in Medicare Part D; remaining Medicaid states can join | Broader coverage picture solidifies |
We update this page as these milestones hit. The "Last verified" date at the top tells you when we last checked every provider link, state coverage status, and pricing point.
knownwell vs Accomplish Health for Medicaid Users
These are the only two providers worth comparing head-to-head if your literal requirement is "bills Medicaid." (Form Health is worth a verification call, but we can't recommend it without resolving the contradiction on their own pages.)
knownwell
Best Multi-State Medicaid OptionMedicaid in select states · Listed in Lilly telehealth network · 4.6/5 on Trustpilot
knownwell is an insurance-first obesity medicine practice listed in Lilly's telehealth directory. They take a clinical, "weight-inclusive" approach — treating obesity as a chronic medical condition, not a cosmetic concern.
Medicaid status: Lilly's telehealth directory indicates Medicaid is accepted in select states. An archived insurance table suggests coverage in at least four states, possibly including Massachusetts, New Hampshire, Rhode Island, and Texas. [NEEDS VERIFICATION — contact knownwell directly before enrolling.]
What patients say: knownwell holds a 4.6/5 rating on Trustpilot with reviews consistently praising clinical quality, provider attentiveness, and a respectful care experience.
Best for: Medicaid enrollees who want a real medical-practice feel with board-certified obesity medicine specialists and may be in one of their covered states.
Check knownwell's current Medicaid availability →Accomplish Health
Strongest Named-Plan Medicaid OptionNY Medicaid + SoonerCare · Aetna, BCBS, Cigna, UHC, Medicare · Insurance-first
Accomplish Health is the most explicitly documented Medicaid option we found. Their insurance page publicly lists specific accepted plans — no ambiguity, no [NEEDS VERIFICATION]:
- New York Medicaid — accepted
- SoonerCare (Oklahoma Medicaid) — accepted
- Also in-network with Aetna, BCBS, Cigna, UHC, Medicare, Fidelis, Tufts, Sentara, CareSource (IN and WV)
Best for: Medicaid enrollees in New York or Oklahoma who want a clear, documented insurance-first path with zero ambiguity about acceptance.
Check Accomplish Health network eligibility →Why "My Friend Got Approved" Doesn't Mean You Will
One of the most common things we see in Reddit threads is someone saying "I got my GLP-1 covered through Medicaid" without specifying their state, indication, or managed care plan. This leads other Medicaid enrollees to believe they can too — and then they hit a wall.
What you're actually seeing when someone says "it worked"
- Your friend in Kentucky with Medicaid coverage for Wegovy has a different state formulary than your Medicaid in Texas.
- Your coworker who got Ozempic through Medicaid was prescribed it for Type 2 diabetes, not weight loss — a required coverage indication in all states.
- The person on Reddit who got Wegovy through Medi-Cal may have gotten it before January 1, 2026, when California eliminated weight-loss coverage.
State, indication, MCO, and timing all matter. That's why this page exists — to help you figure out your specific situation instead of chasing someone else's.
How We Verified These Providers
We checked the insurance/FAQ pages, terms of service, and any public network participation documentation for 12 providers: knownwell, Accomplish Health, Form Health, Ro, PlushCare, MEDVi, Eden, Hims/Hers, TrimRx, SkinnyRX, Walgreens Weight Management, and Found.
Source hierarchy:
- Provider's own insurance, FAQ, and terms pages
- Manufacturer telehealth directories (Lilly.com for knownwell network data)
- KFF Medicaid tracking data (for state coverage counts and policy changes)
- CMS announcements (for BALANCE Model and federal policy)
- State Medicaid formulary documents
- FDA announcements (for indication approvals and compounding policy)
[NEEDS VERIFICATION] flags indicate information we found that may be accurate but could not confirm on a current, primary-source URL. Where a provider's own pages contradict each other (Form Health), we surface the contradiction rather than picking a side.
Why we include non-affiliate options: knownwell and Accomplish Health are not affiliate partners. We include them because they are the honest answer to the question this page exists to answer. A page that only recommended affiliate partners for this query would fail you and fail the search intent.
Related Guides & Comparisons
- Wegovy Prior Authorization: Criteria, Forms & What to Expect
- Best GLP-1 Cash Pay Programs: 7 Real Picks (April 2026)
- Month-to-Month GLP-1 Providers: 8 Options Compared
- GLP-1 Providers With Flat-Rate Pricing — 7 Options Compared
- Semaglutide Providers That Accept HSA: 9 Verified Options
- Tirzepatide Providers That Accept HSA: 8 Verified Options
- Best GLP-1 Pill Provider 2026: Wegovy Pill, Foundayo & Rybelsus Compared
- Ozempic Cost Without Insurance: Real Prices Verified
- MEDVi vs Henry Meds: 7 Real Differences Compared
- GLP-1 Providers That Accept Afterpay: 6 Verified Options
Frequently Asked Questions: GLP-1 Providers & Medicaid
Your Next Step
You came here looking for GLP-1 providers that accept Medicaid. Now you know the honest answer: very few do, most states don't cover GLP-1s for weight loss, and the coverage map is getting smaller before it potentially gets bigger through BALANCE. But you also know the paths that are actually open.
If knownwell or Accomplish Health is in your state:
If your doctor can prescribe for a covered indication (diabetes, CV risk, sleep apnea, MASH):
Start with our Wegovy prior authorization guide →If insurance is a dead end entirely — cash-pay is your path:
Being on Medicaid shouldn't mean being locked out of medications that are changing people's lives. The system hasn't caught up yet. But your options are clearer than you think — and you don't have to wait for Washington to sort it out.
Affiliate Disclosure
Weight Loss Provider Guide is an independent comparison resource for GLP-1 telehealth providers. Some providers on this page are affiliate partners — when you use our links, we may earn a commission at no additional cost to you. This compensation never influences our rankings, editorial recommendations, or the inclusion of non-affiliate options like knownwell and Accomplish Health. Our editorial team researches, verifies, and compares telehealth platforms so you can make informed decisions. Not all providers listed are affiliate partners.
Published by Weight Loss Provider Guide, an independent comparison resource for GLP-1 telehealth providers.
Last Verified: April 9, 2026 · Pricing Verified: April 9, 2026