How Long Does Prior Authorization Take for Zepbound?
Quick Answer
The insurer's formal decision usually takes 24 hours to 5 calendar days once they receive a complete submission. That's the official clock.
But “insurer decision” and “medication in hand” are two very different timelines — and the gap between them is where most of the frustration lives. The full end-to-end timeline — from your doctor's office starting paperwork through a decision — is often 2–3 weeks when going through a telehealth service.
Below: exactly how to tell whether your wait is normal, what's probably causing the holdup, and what to do about it today.
Is Your Zepbound Prior Authorization Still on Track?
Before the details, here's a quick status check based on how long it's been since your doctor submitted the PA request.
| Time since submission | What it probably means | What to do today |
|---|---|---|
| 0–3 business days | Still within normal range for most plans. Many ePA (electronic prior authorization) decisions happen in 24–72 hours. | Confirm your doctor actually submitted. Ask: "Was it sent electronically or by fax? What date?" |
| 4–7 business days | Plausible on some plans, but worth confirming. BCBSIL allows up to 5 calendar days for non-urgent requests. | Call your insurer's pharmacy benefits number. Ask: "Do you have a PA on file for Zepbound? What date was it received? Is anything missing?" |
| 8–14 business days | Likely stalled. The insurer either requested additional documentation or never received the original submission. | Call both your doctor's office and your insurer the same day. Get the missing-documentation list in plain language. Push for resubmission within 48 hours. |
| 15+ business days or denied | Either denied, stuck in an appeal queue, or your plan may not cover Zepbound at all — which is a coverage exclusion, not a PA delay. | Get the denial reason in writing. Determine whether this is a documentation issue, a criteria issue, or a plan exclusion — each has a different fix. |
Benchmarks: CMS Part D coverage determination rules (cms.gov); Blue Shield of California drug PA timing (blueshieldca.com); Cigna pharmacy PA timing (cigna.com); BCBSIL (bcbsil.com). Verified April 11, 2026.
Want a personalized read on your situation?
Our free matching tool walks you through the best path forward based on your insurance type, timeline, and goals.
Get your next-step plan in 60 secondsHow Long Does Prior Authorization Take for Zepbound? The Official Timelines.
Every insurer has a published decision window — the maximum time they're allowed once they receive a complete PA request. Here's what we verified from official sources:
| Plan / insurer type | Standard decision window | Expedited / urgent window | Source |
|---|---|---|---|
| Medicare Part D | 72 hours | 24 hours | CMS.gov coverage determinations |
| Blue Shield of California | 24–72 hours (typical) | Not separately published | blueshieldca.com drug PA page |
| Cigna pharmacy requests | 72 hours | 24 hours | Cigna exception process |
| BCBSIL (Blue Cross Blue Shield of Illinois) | 5 calendar days | 48 hours | bcbsil.com prior authorization |
| Ro's end-to-end insurance path | ~2–3 weeks total (intake + docs + submission + insurer review) | N/A | ro.co/weight-loss/zepbound |
The takeaway nobody tells you:
The insurer's formal review clock is often just a fraction of the total wait. When Ro says “2–3 weeks,” that includes their medical team reviewing your case, preparing documentation, submitting to the insurer, and waiting for the insurer's decision. The insurer's part might be only a few days of that. The rest is everything that happens before and after.This is exactly why someone on Reddit says “mine took less than a day” while someone else says “it's been 10 weeks.” They're measuring different things.
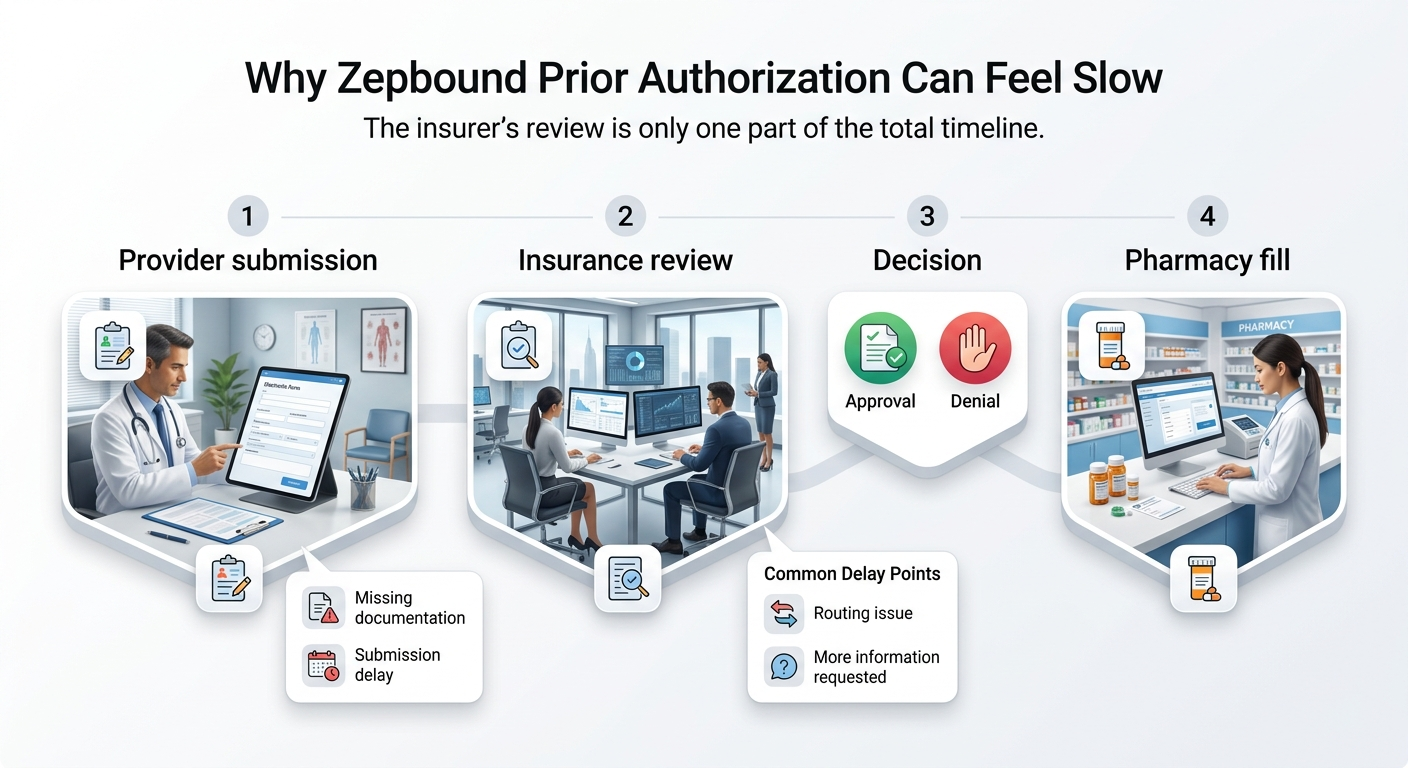
Why Can Your Insurer Say “72 Hours” While You've Been Waiting Two Weeks?
Because you're experiencing the whole chain, not just the insurer's clock. Here's what actually happens between “doctor prescribed Zepbound” and “medication in hand” — and where delays hide.
Doctor's office intake (often several days, sometimes longer)
Your doctor writes the prescription. Then their staff has to gather your documentation, fill out the insurer-specific PA form, and submit it. If the office is busy, short-staffed, or unfamiliar with Zepbound's documentation requirements, this step alone can take a week or more. You may think the PA has been "submitted" when it's actually sitting in a queue at your doctor's office.
Submission method matters
Electronic PA (ePA) through platforms like CoverMyMeds processes faster than fax. Fax submissions introduce manual handling on both ends. If your doctor's office faxed the request and the insurer's fax system misfiled it — or if the request was sent to the regular claims department instead of the pharmacy benefits PA team — the clock hasn't even started.
Insurer review (24 hours – 5 calendar days)
This is the official decision window in the table above. If documentation is complete, this step is usually fast. If something's missing, the insurer sends a "request for additional information" — which goes back to your doctor's office and restarts the waiting cycle.
Pharmacy processing after approval (varies)
Once approved, the authorization has to reach your pharmacy. If you're using a specialty pharmacy or mail-order, add transit time. If the pharmacy doesn't have Zepbound in stock, add more.
Refill and dose-change complications
Zepbound requires dose titration — you start at 2.5 mg and increase over time. Some plans require a new PA or modification for each dose change. Others issue a blanket approval for all doses within the authorization period. If your pharmacy runs a refill at a new dose and the system rejects it, you may be back at step 1.
"I wait, and wait, 2 weeks go by, no update…" — Zepbound subreddit user describing their PA experience. Individual experiences vary widely based on plan type and documentation completeness.
"It turned out they submitted where normal insurance claims would be sent." — Zepbound subreddit user who discovered their PA request was misrouted. This is more common than you'd think.
Does Zepbound Always Require Prior Authorization?
Usually — but not always, and the answer depends on how you're getting it.

Through insurance (Zepbound single-dose pen):
Yes, almost always. Eli Lilly's own patient materials confirm most single-dose pen prescriptions require a prior authorization form. (zepbound.lilly.com/access-coverage)
Among Medicare beneficiaries using diabetes-indication GLP-1s, a Penn LDI study published in JAMA found PA was required for a growing share of prescriptions — and the trend is toward more requirements, not fewer.
Through self-pay (LillyDirect vial or KwikPen):
No PA needed. Eli Lilly's healthcare provider materials confirm that self-pay routes through LillyDirect bypass insurance entirely — no PA, no formulary check, no waiting on your plan's decision. (zepbound.lilly.com/hcp)
This is why two people can both be “starting Zepbound” while living in completely different timelines. One is navigating insurance; the other paid cash and had medication delivered in days.
What Does Your Doctor Need to Submit for Zepbound PA?
The fastest approvals happen when the first submission already includes everything the insurer will ask for. We reviewed Zepbound-specific PA requirements from Eli Lilly's PA Resource Guide, Highmark's Zepbound PA form, CVS Caremark's criteria document, UnitedHealthcare's weight-loss PA criteria, and BCBSM's step therapy guidelines — and the same documentation items appear across nearly every plan.

Zepbound PA documentation: what decides whether it moves fast or stalls
| Document / data point | Why insurers ask for it | Which plans emphasize it | What you can prepare |
|---|---|---|---|
| Current weight and BMI with a date | Required for every Zepbound PA — proves you meet BMI threshold (≥30, or ≥27 with comorbidity; some plans like BCBS Michigan require ≥35). | All plans (Lilly PA Resource Guide) | Step on a scale at your doctor's office. Make sure it's in your chart with today's date. |
| Comorbidity documentation | Proves medical necessity beyond BMI alone. Hypertension, type 2 diabetes, dyslipidemia, OSA, and cardiovascular disease are the most commonly accepted. | All plans — UHC and CVS Caremark specifically list qualifying conditions. | Bring a list of your diagnoses and any relevant lab results (A1c, lipid panel, blood pressure readings). |
| 6-month lifestyle modification history | Most plans require documented evidence of dietary changes and physical activity attempts before approving Zepbound. | CVS Caremark requires 6-month comprehensive program. Highmark accepts diet logs, gym receipts, wearable device summaries, and counseling documentation. | Gather any records: diet program enrollment, gym membership, dietitian visits, app data, or a written statement from your doctor noting dietary counseling over the past 6 months. |
| Prior weight-loss medication history | Step therapy — some plans want to see you've tried another option first. CVS Caremark currently requires trying Wegovy before approving Zepbound. | CVS Caremark (formulary policy), UHC (criteria document). | List every weight-loss medication you've tried, with dates, doses, how long you took it, and why you stopped. |
| ICD-10 diagnosis codes | The specific code determines which coverage bucket your request falls into. E66.01 (obesity) vs. G47.33 (OSA) can trigger completely different criteria. | All plans. | Your doctor handles this — but ask which indication (weight management vs. OSA) they're submitting under, because it affects which criteria apply. |
| Sleep study results (OSA path only) | Required if submitting under the obstructive sleep apnea indication. Must show AHI ≥15 events/hour. | UHC, CVS Caremark, Highmark. | If you have a sleep study, bring the results. If you suspect OSA but haven't been tested, ask your doctor — the OSA path can open a separate coverage door. |
| Baseline weight for renewal | Plans require proof that Zepbound is working. BCBSM requires 5% weight loss from baseline for continuation. | BCBSM (guidelines), CVS Caremark. | Keep a weight log from day one. Your doctor should document your starting weight clearly in your chart. |
Authorization length varies by plan and indication:
CVS Caremark grants 8 months for weight management and 6 months for OSA. UHC grants 6 months initially, then 12 months for reauthorization. BCBSM may grant up to 1 year. Set a calendar reminder to start the renewal process at least 30 days before your current authorization expires — there's typically no grandfathering if it lapses.Why Is My Zepbound Prior Authorization Taking So Long?
If you're past the normal window and still waiting, the cause is almost always traceable. Here are the six most common failure points — and how to fix each one.
| What's probably wrong | How to confirm | How to fix it |
|---|---|---|
| 1. Missing BMI or current weight | Call insurer: "Was the PA returned for additional information?" | Ask your doctor's office to resubmit with a dated weight measurement in the chart notes. |
| 2. No documented lifestyle modification history | Insurer denial letter will reference "prior weight management attempts" | Provide any evidence: diet program enrollment, gym membership, dietitian visits, app data. Highmark's form explicitly accepts wearable device summaries and program receipts. |
| 3. Step therapy not completed | Insurer says "try [other medication] first" | If you've already tried another medication, document it with dates and outcomes. On CVS Caremark plans specifically, this often means trying Wegovy first. |
| 4. Wrong indication or diagnosis code | Check the PA form — is it submitted under E66.01 (obesity) or G47.33 (OSA)? | If you have both obesity and OSA, the OSA indication may have a clearer approval path. Discuss with your doctor which indication to submit under. |
| 5. Request was never received or was misrouted | Call insurer: "Do you have a PA on file for Zepbound under my name and member ID?" | If they say no — that's your answer. Request immediate resubmission, preferably via ePA (CoverMyMeds), not fax. |
| 6. Your plan doesn't cover Zepbound (this is a coverage exclusion, not a PA delay) | Insurer says "not a covered benefit" or "formulary exclusion" | A PA can't override a plan exclusion. You'd need a formulary exception request (different process), the OSA pathway, or cash-pay alternatives. |
The single most fixable delay:
Making sure the submission is complete on the first try. Every round-trip back to your doctor's office for missing information can add a week or more to the process — because it has to re-enter their queue and then re-enter the insurer's review queue.What Should You Do on Day 3, Day 7, and Day 14?
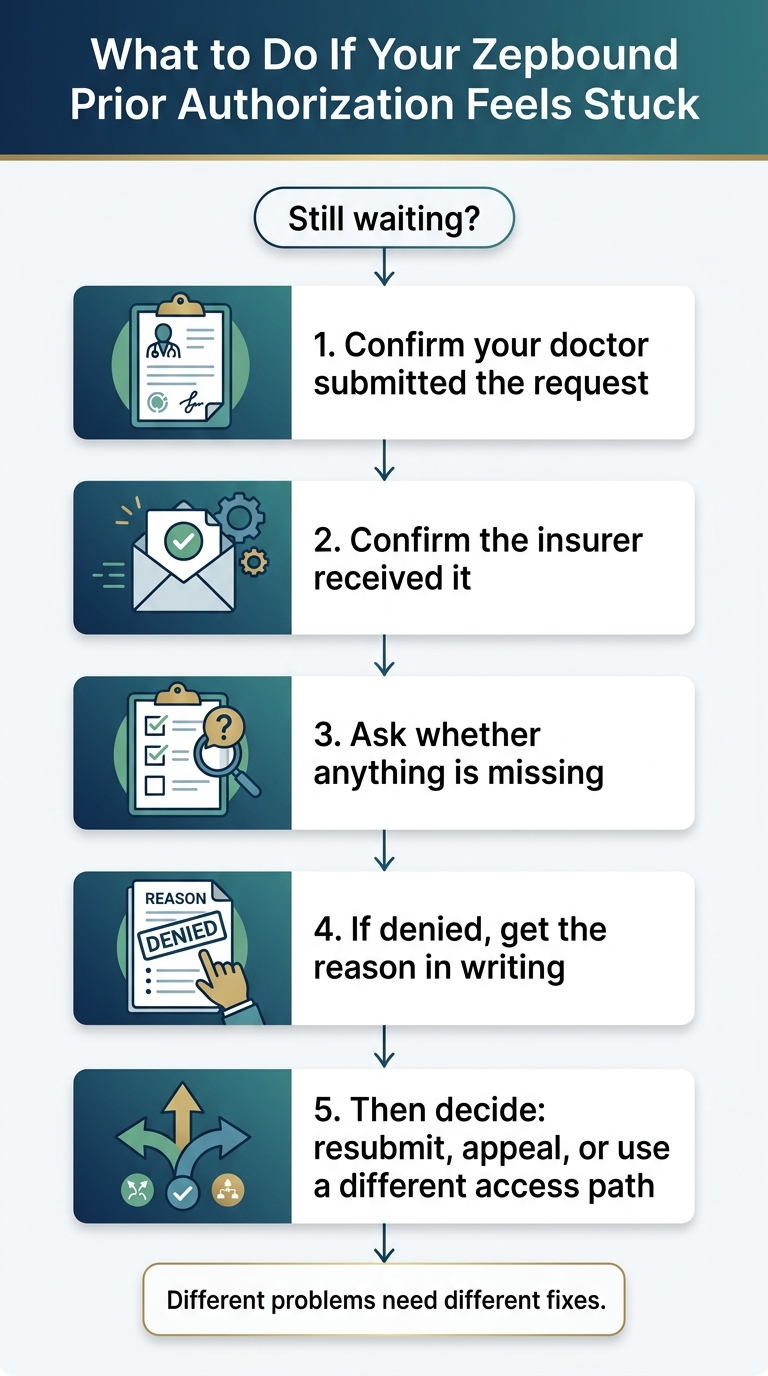
The right action depends on where you are in the process. Here's our editorial recommendation based on the verified timing windows above.
- Call your doctor's office: "Can you confirm when the prior authorization for Zepbound was submitted, and whether it was sent electronically or by fax?"
- If they say it hasn't been submitted yet, ask what's holding it up and what you can provide to speed it along.
- If they confirm submission, note the exact date. That's when your insurer's clock starts.
- Call your insurer's pharmacy benefits number (often on the back of your card but separate from general member services): "I'm calling to check on a prior authorization for Zepbound, tirzepatide. Can you confirm you received it and tell me the status?"
- If pending: ask if any additional documentation has been requested.
- If approved: ask for the authorization number and call your pharmacy to confirm they can see it.
- If not received: contact your doctor's office immediately for resubmission.
- Call both your doctor's office and your insurer on the same day.
- With your insurer: "This PA was submitted on [date]. Can you tell me specifically what's needed to move it forward? Is there a missing document? Has additional information been requested?"
- With your doctor: "My insurer says [specific missing item]. Can this be resubmitted within 48 hours?"
- Ask your insurer if an expedited review is appropriate. Important: expedited PA review is reserved for situations where waiting could seriously jeopardize your health — not available simply because the wait is frustrating. Your doctor would need to justify the medical urgency.
- Get the denial reason in writing.
- Determine which category: missing documentation (fixable with resubmission), criteria not met (appeal), or plan exclusion (different process).
- See the denial section below for specific next steps.
You've been patient long enough. Get your personalized next-step plan — our free matching tool walks through the best path forward in about 60 seconds.
Get your next-step planWhat If Your Zepbound Prior Authorization Is Denied?
✅ Denied because documentation was incomplete
This is the most common and most fixable scenario. Your doctor's office resubmits with the missing items, and the review starts fresh. This isn't technically an appeal — it's a new submission.
Fix: Get the specific list of what was missing. Provide it. Resubmit.
⚠️ Denied because you don't meet the plan's criteria
This could mean your BMI is below the plan's threshold (some plans require ≥35, stricter than the FDA's ≥30), you haven't completed required step therapy, or you haven't documented enough prior lifestyle modification effort.
Fix: You can appeal. Eli Lilly's own access resources confirm that your provider can submit a new PA with a letter of medical necessity, or file a formal appeal. (zepbound.lilly.com/access-coverage) The typical appeals process has three levels:
- First-level internal appeal — your provider calls or writes to the insurer with additional documentation and a letter of medical necessity.
- Second-level internal review — reviewed by a medical director not involved in the original decision.
- Independent external review — an outside organization reviews the case. For Medicare Part D, appeal timelines are 7 days standard and 72 hours expedited. (CMS.gov)
🚫 Denied because your plan excludes weight-loss medications
This is fundamentally different. A PA denial means “you didn't prove this was necessary.” A plan exclusion means “we don't cover this category of drug regardless.” No amount of documentation fixes a plan exclusion through the standard PA process.
Options:
- Request a formulary exception — this is a separate process from PA. Your doctor argues that Zepbound is medically necessary and no covered alternative is appropriate.
- Pursue the OSA indication — if you have obesity AND obstructive sleep apnea, Zepbound is the only FDA-approved medication for OSA. Some plans that exclude weight-loss drugs do cover the OSA indication. A sleep study showing AHI ≥15 events/hour is typically required. → See our Zepbound sleep apnea PA guide
- Switch to a self-pay path — see the section below for cash-pay pricing with no PA required.
CVS Caremark note: CVS Caremark removed Zepbound from its standard formulary effective July 2025. If your PBM is CVS Caremark, you'll generally need to document trial and failure (or intolerance) of Wegovy before a Zepbound formulary exception will be considered. (CVS Caremark GLP-1 formulary page)
Can You Get Zepbound Without Waiting on Insurance?
Yes. And understanding this option doesn't mean giving up on insurance — it means you don't have to choose between waiting on bureaucracy and starting treatment.
Cash-pay Zepbound: no PA, no insurer, ships to your door
Eli Lilly offers Zepbound through self-pay channels (LillyDirect and authorized partners like Ro) with no prior authorization required. Current pricing:
| Dose | Monthly cost (self-pay via LillyDirect/Ro) | Notes |
|---|---|---|
| 2.5 mg (starting dose) | $299/month | |
| 5 mg (maintenance dose) | $399/month | |
| 7.5 mg | $449/month | LillyDirect Self-Pay Journey offer; must refill within 45 days of previous delivery |
| 10 mg | $449/month | Same 45-day refill requirement |
| 12.5 mg | $449/month | Same 45-day refill requirement |
| 15 mg | $449/month | Same 45-day refill requirement |
Regular price without the 45-day refill offer is higher for 7.5 mg+ doses ($499–$699 depending on dose). Source: zepbound.lilly.com/savings, verified April 11, 2026.
If you want help navigating brand-name Zepbound through insurance — or want someone else to handle the paperwork
Ro carries FDA-approved Zepbound with both a cash-pay path and an insurance concierge
Getting started: $39 for the first month (Ro Body membership).
Ongoing membership: As low as $74/month with annual plan paid upfront, or $149/month month-to-month. Medication cost is separate.
Insurance path: Ro's care team submits the prior authorization on your behalf, handles paperwork, and follows up with your insurer. Their stated timeline for the full insurance process is about 2–3 weeks, which includes intake, documentation preparation, submission, and insurer review.
Cash-pay path: Zepbound KwikPen ships directly to you at the same LillyDirect pricing above. No PA required. Typically arrives within a week.
And here's what a lot of people don't realize: you can do both at the same time. Start on cash-pay now so you don't lose momentum, while Ro's team fights for your insurance coverage in the background. If the PA comes through, you switch to your copay and your cost drops.
What about the Zepbound Savings Card?
If your commercial insurance covers Zepbound
Savings card can bring your copay down to as low as $25/month (up to $100 savings per 28-day fill, $1,300 annual cap). You still need PA approval first — the card reduces your copay, it doesn't bypass PA.
If your commercial insurance doesn't cover Zepbound
Savings card can reduce the cost of single-dose pens to as low as $499/month (up to $620 savings per fill, $8,060 annual cap).
What about Medicare?
Medicare Part D currently does not cover Zepbound for weight loss. However:
- Some Part D plans cover Zepbound for obstructive sleep apnea.
- The Medicare GLP-1 Bridge (CMS demonstration program) runs July 1, 2026 through December 31, 2026. It will offer eligible Medicare Part D enrollees access to Zepbound KwikPen specifically (not the single-dose pen or single-dose vial) for weight management at $50/month. Prior authorization will be managed through a single centralized CMS processor. (Source: CMS.gov Medicare GLP-1 Bridge FAQ)
- The BALANCE Model for broader Medicare Part D coverage launches January 2027. (CMS.gov)
What If You're Using Zepbound for Sleep Apnea?
That's a different approval path — and in many cases, a stronger one. The FDA approved Zepbound for moderate-to-severe obstructive sleep apnea in adults with obesity in December 2024, making it the first and currently only FDA-approved medication for OSA. (FDA press announcement)
Key documentation for OSA-pathway PA:
- Sleep study results with AHI ≥15 events/hour
- BMI ≥30
- Documentation of prior CPAP/PAP therapy and compliance (or documented intolerance)
- In some cases, sleep specialist involvement (UHC criteria specifically require this)
Because Zepbound has no formulary alternative for OSA — unlike weight loss, where insurers can steer you toward Wegovy — the formulary exception argument is significantly stronger on this pathway.
This page focuses on the weight-loss PA timeline. For the full OSA criteria breakdown by insurer — including UHC, CVS Caremark, Highmark, and BCBSM specifics — read our Zepbound sleep apnea PA guide →
How the Prior Authorization Landscape Is Changing in 2026
Several shifts are happening right now that affect how long your Zepbound PA takes — and whether you'll need one at all.
Insurer tightening
Some insurers are raising BMI thresholds from ≥30 to ≥35 and extending step therapy requirements. Several plans have confirmed there will be no grandfathering of existing PAs at plan renewal — even if you have an active authorization, it may need to be reapproved under new terms when your plan year resets. Start the renewal process early.
CVS Caremark Wegovy-first policy
If your PBM is CVS Caremark, Zepbound is off their standard formulary as of July 2025. Any Zepbound claim requires a formulary exception with documented Wegovy trial and failure or intolerance.
Medicare expansion (July 2026)
The Medicare GLP-1 Bridge brings Zepbound KwikPen to eligible Medicare Part D enrollees at $50/month from July 1 through December 31, 2026, with PA managed centrally by CMS.
New alternatives entering the market
Foundayo (orforglipron), an oral non-peptide GLP-1 for obesity developed by Eli Lilly, received FDA approval April 1, 2026. The Wegovy tablet (oral semaglutide for weight management) was approved December 2025. As oral options gain traction, insurers may shift formulary positioning over time — which could change the Zepbound PA landscape.
Want Ro's team to handle your Zepbound PA paperwork while you start on cash-pay now?
Ro's insurance concierge handles the calls, forms, and follow-ups. Start for $39. Cash-pay Zepbound ships within a week.
What We Actually Verified for This Page
We built this page from official sources — not from rewording what other sites said. Here's exactly what we checked.
Timing sources verified (April 11, 2026)
| Source | What it told us |
|---|---|
| CMS Part D coverage determination rules | 72-hour standard, 24-hour expedited decision windows for drug coverage determinations |
| Blue Shield of California drug PA page | Drug PA "typically" takes 24–72 hours |
| Cigna pharmacy exception documentation | 72-hour standard, 24-hour expedited |
| BCBSIL prior authorization page | 5 calendar days non-urgent, 48 hours urgent |
| CMS-0057-F final rule | Excludes drug PAs from new federal timing/API requirements |
Zepbound-specific criteria documents verified (April 11, 2026)
| Source | Key details |
|---|---|
| Eli Lilly Zepbound PA Resource Guide | Typical PA questions, required documentation, ICD-10 codes |
| Eli Lilly patient access page | PA process overview, denial/appeal guidance |
| Highmark Zepbound PA form | Detailed documentation requirements including wearable data, OSA fields |
| CVS Caremark Zepbound criteria | 6-month lifestyle program, BMI thresholds, 8-month initial approval |
| UnitedHealthcare weight-loss PA criteria | BMI thresholds, lifestyle modification, 6-month initial authorization |
| BCBSM PA and step therapy guidelines | Up to 1-year approval, 5% weight loss for continuation |
What still varies by employer plan:
Employer-sponsored plans can set their own Zepbound criteria, BMI thresholds, step therapy requirements, and coverage exclusions. No guide can tell you whether your specific employer plan covers Zepbound — call the pharmacy benefits number on your insurance card and ask: “Is tirzepatide (brand name Zepbound) on my plan's formulary for weight management? Is prior authorization required? What are the specific criteria?”Related Guides
Frequently Asked Questions: Zepbound Prior Authorization
Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz. A few quick questions about your insurance situation, budget, and goals — and we'll match you with the path most likely to get you started without unnecessary delays.