GLP-1 Providers That Accept Wellness Stipend: Best Options for Easy Reimbursement
By Weight Loss Provider Guide Research Team · Last verified
Weight Loss Provider Guide is an independent comparison resource for GLP-1 telehealth providers. We may earn a commission when you click a provider link. Our rankings are based on verified provider policies, not commission rates. Methodology.
Most GLP-1 providers don't "accept" a wellness stipend the way they accept a Visa card. That's the mechanic search results keep burying — and it's the reason so many people try to use their wellness stipend on a GLP-1 and get denied or give up.
For the majority of employer stipend programs, reimbursement happens after you pay — you buy with a personal card, download an itemized receipt, and submit it to your stipend platform (Compt, Forma, Espresa, HealthEquity LSA, Fringe, Benepass, PeopleKeep, and similar) for reimbursement through payroll or direct deposit.
So the right question isn't which providers "accept" your stipend. It's which providers issue a receipt clean enough that your claim actually goes through — and whether your employer's specific rules allow compounded or FDA-approved medication.
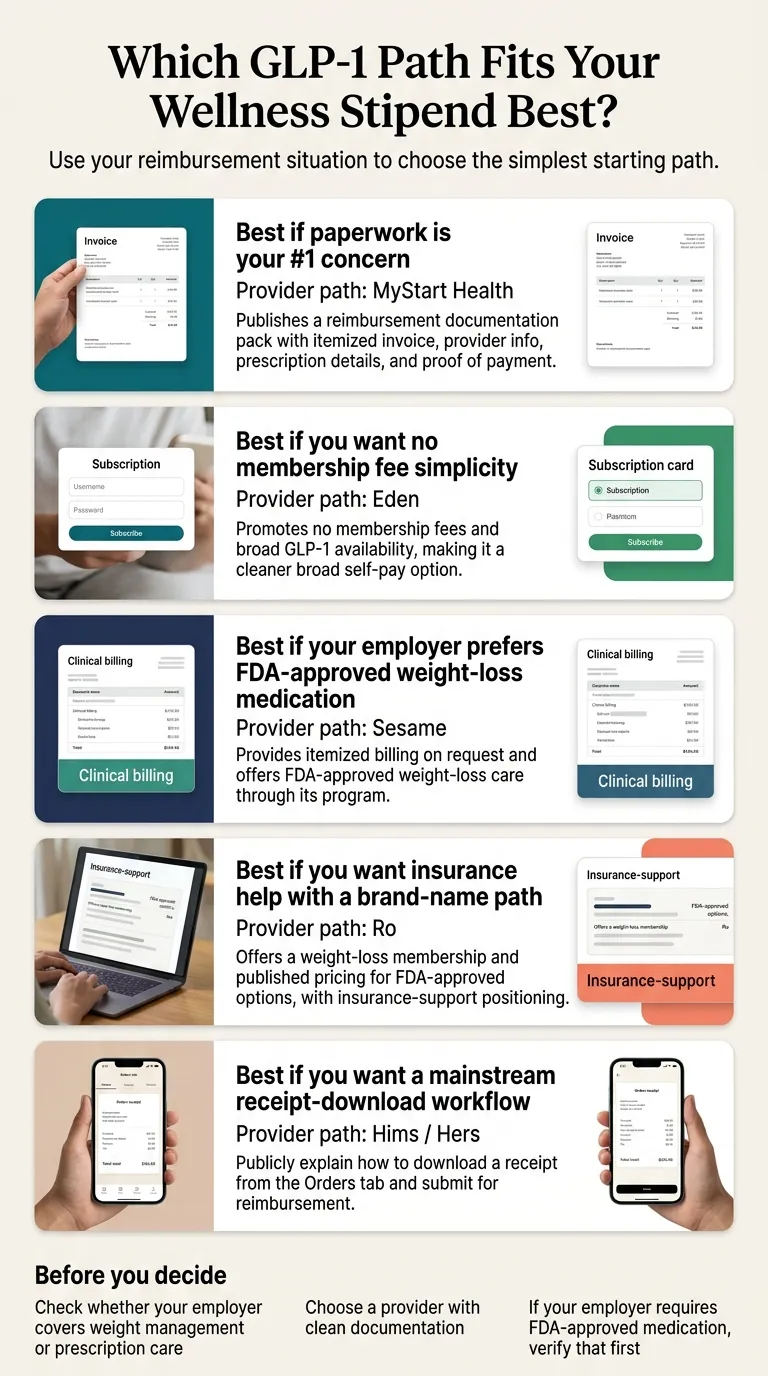
Based on verified provider policies as of April 2026, the cleanest paths are:
- MyStart Health — flat $299/month with a publicly documented 4-doc reimbursement pack
- Eden — no membership fee, compounded semaglutide from $249/month, HSA/FSA eligible, 50 states
- Sesame Care — cleanest FDA-approved path from $59/month annual plan + FDA-approved Wegovy, Zepbound, Foundayo
- Ro — FDA-approved with insurance help — start for $39, then as low as $74/month annual
- Hims / Hers — publicly documented receipt-download from Orders tab ($39 first month, $149/month + medication)
Can You Actually Use a Wellness Stipend for GLP-1 Care?
A wellness stipend is an employer-funded allowance that reimburses eligible expenses. Your employer sets three things:
- 1How much. Wellness stipends commonly range from about $50 to $300 per month, or $500 to $1,500 annually, based on Forma's published guidance. Some employers offer more for GLP-1 or weight-management specifically — Compt has published examples of weight-management stipends around $150 per month.
- 2What's eligible. Some employers open the category wide to anything wellness-related. Others specifically include or exclude prescription medications, compounded products, or weight-loss treatment.
- 3What documentation is required. Most platforms ask for an itemized receipt; some ask for a Letter of Medical Necessity; a few accept a simpler payment confirmation.
The 60-second check before you spend a dollar
Wellness Stipend vs. HSA vs. FSA vs. LSA vs. HRA
A quick decoder — people often use these terms loosely when they mean something different.
| Benefit Type | Tax Treatment | Who Sets Rules | GLP-1 Eligibility |
|---|---|---|---|
| Wellness stipend | Post-tax (reimbursement reported on W-2 as wages) | Your employer | Typically allowed if employer opts in |
| Lifestyle Spending Account (LSA) | Post-tax | Your employer, within platform rules | Typically allowed if employer opts in |
| HSA (Health Savings Account) | Pre-tax | IRS (with plan rules) | Eligible with prescription |
| FSA (Flexible Spending Account) | Pre-tax | IRS (with plan rules) | Eligible with prescription; some plans request Letter of Medical Necessity |
| HRA (Health Reimbursement Arrangement) | Pre-tax for employer; non-taxable reimbursement | Employer, within ERISA rules | Depends on plan — some run a dedicated Weight Management HRA |
How Wellness Stipend Reimbursement Actually Works for a GLP-1
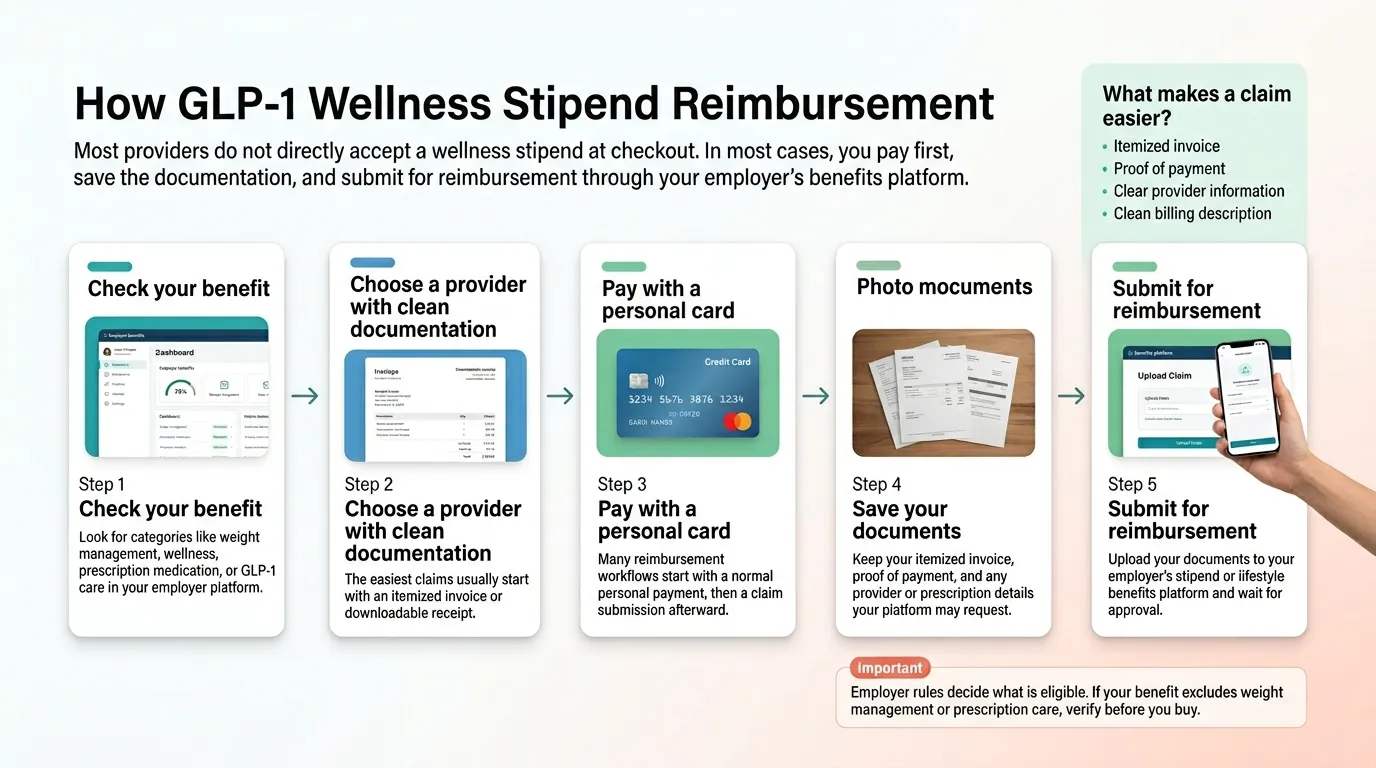
Step 1: Confirm weight management is eligible inside your stipend platform
Log in. Search for "weight management," "GLP-1," "semaglutide," or "prescription medications." If any of these appear, you're approved by default. If not, use the email template below — don't skip this step.
Step 2: Pick a provider based on how your platform pays out
Receipt-upload reimbursement (Compt, Forma, Espresa, HealthEquity LSA) — any provider with a clean itemized receipt works. Benefits card / direct spend (Benepass, some PeopleKeep) — providers accept these like any debit card, but keep the receipt. Marketplace (Fringe) — eligibility depends on whether your employer added GLP-1 vendors.
Step 3: Pay with the right payment method
For receipt-upload models: use a personal credit or debit card. Do not use an HSA/FSA card unless you're also planning an HSA/FSA submission (to avoid double-dipping). For benefits-card models: use the card, but save the itemized receipt anyway.
Step 4: Download your itemized receipt
Your receipt must show: provider name, medication or program name (not "monthly subscription"), date of purchase, dollar amount, and payment confirmation. MyStart → documented reimbursement pack. Eden → account portal. Sesame → email [email protected]. Ro → account history. Hims/Hers → Orders tab.
Step 5: Upload to your stipend platform
File under "Weight Management" if available, otherwise "Health & Wellness" or "Wellness." Attach the receipt and any supporting documents. Add a brief note: "Physician-supervised GLP-1 treatment for weight management. Itemized invoice and payment confirmation attached."
Reimbursement is taxable wages
Best GLP-1 Providers That Accept Wellness Stipend in 2026
How we scored stipend fit:
- • 40% — Documentation and reimbursement support (itemized invoice quality, receipt downloadability, LMN workflow, published guidance)
- • 20% — Price simplicity (flat pricing, same price across doses, clean single-line billing)
- • 15% — Cancellation friction (cutoff windows, refund eligibility)
- • 15% — State availability (50-state vs. limited footprint)
- • 10% — Regulatory and trust signals (LegitScript, pharmacy disclosures, FDA actions, transparency)
The Comparison Table
| Provider | Best For | Starting Price | Reimbursement Path | States | Score |
|---|---|---|---|---|---|
| ★ MyStart Health | Documentation-heavy stipend users | $299/mo flat | Published docs pack: itemized invoice + provider credentials + Rx details + proof of payment | 50 states | 9.4 / 10 |
| Eden | No-membership broad default | Compounded semaglutide from $249/mo; tirzepatide from $349/mo | HSA/FSA eligible across plans; downloadable receipt | 50 states | 8.9 / 10 |
| Sesame Care | FDA-approved-only stipends | Success by Sesame from $59/mo (annual) + medication | Itemized bill on request via [email protected] | 50 states | 8.6 / 10 |
| Ro | FDA-approved with insurance help | $39 first month, $149/mo standard (or $74/mo annual) | Pay-first/reimburse-later; detailed receipts in account history | 50 states + D.C. | 8.1 / 10 |
| Hims / Hers | Mainstream branded receipt workflow | $39 first month, $149/mo membership + medication | Downloadable from Orders tab; documented at hims.com/weight-loss/fsa-hsa | Wide coverage | 7.7 / 10 |
| Willow | All-in-one HSA/FSA checkout in served states | $299/mo | HSA/FSA at checkout; itemized receipt available | State-specific (check their FAQ) | 7.6 / 10 |
Verified April 17, 2026 against provider and platform published sources.
MyStart built infrastructure specifically around reimbursement. Their dedicated HSA/reimbursement page (mystarthealth.com/hsa) walks through what their documentation pack includes — itemized invoice, provider credentials, prescription details, and proof of payment — the four artifacts most stipend platforms request. For a stipend user, that's the entire game.
What we verified:
- Published reimbursement documentation pack at mystarthealth.com/hsa
- Flat $299/month pricing with price-lock across dose levels
- Licensed clinicians available in all 50 states
- Cancel-anytime; refunds issued before medication fulfillment
- No separate membership fee
The real trade-off
Eden is the strongest broad default for stipend users who want simplicity without membership fees. All plans are HSA/FSA eligible. Pricing stays consistent as dose increases. Serves all 50 states.
- Compounded semaglutide from $249/month
- Compounded tirzepatide from $349/month
- FDA-approved Wegovy, Ozempic, and Zepbound available at brand-name cash-pay pricing
- HSA/FSA eligibility language published for all plans
- 50-state GLP-1 program availability
Trade-off: Eden doesn't publish a reimbursement documentation pack as explicitly as MyStart. For standard stipend claims, the downloadable receipt is enough. For employer programs requiring extra documentation, MyStart's pack is cleaner.
If your employer's stipend rules say the word "FDA-approved," Sesame is the clean answer. Sesame publishes its itemized-billing workflow directly on support pages — email [email protected] for an itemized bill suitable for HSA, FSA, or stipend submission.
- Success by Sesame subscription from $59/month (annual plan)
- FDA-approved Wegovy pill (oral) from $149/month
- FDA-approved Wegovy injection, Zepbound (tirzepatide), Foundayo (orforglipron)
- HSA/FSA itemized bill process via [email protected]
Trade-off: Subscription and medication are separate line items on your stipend submission. Most platforms handle both — verify before you buy.
Ro fits when your stipend rules require FDA-approved medication and you also want help navigating insurance. Ro's Body program includes an insurance concierge for prior authorization — matters if your employer requires attempting insurance before the stipend kicks in.
- $39 intro offer for first month, $149/month standard, or $74/month annual plan paid upfront
- FDA-approved Zepbound® and Foundayo™ in the lineup; Wegovy® pill available
- Services available in all 50 states + D.C.
- Pay-first/reimburse-later with detailed receipt available in account history
Trade-off: Membership billed separately from medication — two line items on your stipend submission.
Hims and Hers publicly document the receipt-for-reimbursement workflow on their own websites. Their instructions walk you through downloading your receipt from the Orders tab and submitting it through your benefits platform.
- $39 first month, $149/month membership, medication billed separately
- Published reimbursement workflow at hims.com/weight-loss/fsa-hsa and forhers.com/weight-loss/fsa-hsa
- Orders tab receipt download process
Worth a mention if you're in a Willow-served state and want a single all-inclusive monthly charge with HSA/FSA usable at checkout. Programs start at $299/month. Cancellations require at least two business days' notice before next processing date.
Trade-off: Willow is compounded-only. If your stipend language requires FDA-approved, skip Willow and go to Sesame or Ro.
Which Stipend Platforms Allow GLP-1 Reimbursement?
| Platform | GLP-1 Eligibility | Payout Model | Tax Treatment |
|---|---|---|---|
| Compt | Explicitly addressed — GLP-1s (Wegovy, Zepbound, Ozempic) eligible under taxable stipend when employer opts in | Receipt upload; does not recommend stored-value cards | Post-tax |
| Forma | Explicitly addressed via dedicated Weight Management HRA product; also supported through standard LSA/wellness stipend config | Platform-configured (HRA or stipend/LSA) | HRA: pre-tax; wellness stipend/LSA: post-tax |
| Espresa | Explicitly addressed — Specialty Care Account designed for GLP-1, HRT, and specialty mental health | Platform-defined; confidential claims processing | Post-tax |
| HealthEquity LSA | Eligibility defined by employer setup; LSA is separate from HSA | Receipt upload; typically within three business days, one to three pay periods | Post-tax |
| Benepass | Employer-defined | Visa Benecard for direct spend OR bank-account reimbursement, depending on configuration | Post-tax |
| Fringe | Employer-defined — marketplace model | Direct marketplace spend, not traditional receipt reimbursement | Post-tax |
| PeopleKeep | Employer-defined | Benefits card OR reimbursement, depending on plan | Post-tax |
Does Compt cover GLP-1?+
Yes, when the employer allows it. Compt's own guide states: GLP-1 medications including Wegovy, Zepbound, and Ozempic can be covered under a taxable stipend when classified as part of a broader health and wellness benefit. Compt operates on a receipt-upload model.
Does Forma cover GLP-1?+
Yes — and Forma has a dedicated product for it. Forma's Weight Management HRA is a pre-tax HRA designed specifically to cover weight-loss medications including GLP-1 treatments. Forma also supports GLP-1 through standard LSA or wellness stipend configurations when the employer includes weight management.
Does Espresa cover GLP-1?+
Yes — Espresa sells a Specialty Care Account designed specifically for GLP-1 reimbursement, covering GLP-1s, HRT, and certain mental health services with capped, predictable employer coverage.
Does Fringe cover GLP-1?+
It depends on your employer's marketplace configuration. Fringe operates a marketplace model where employers curate eligible vendors. If your Fringe doesn't include a GLP-1 telehealth vendor, check whether your employer allows out-of-marketplace submissions.
Does HealthEquity LSA cover GLP-1?+
Your HealthEquity LSA might, if your employer configured weight management into the eligible categories. HealthEquity also runs an HSA-integrated GLP-1 program through Agile Telehealth — that's a separate product from a HealthEquity LSA.
Does Benepass cover GLP-1?+
Depends on your Benepass configuration. Benepass supports a Visa benefits card for direct spend and direct-deposit reimbursement. If GLP-1 telehealth is eligible in your program, you can typically use either model.
Email template if your platform doesn't list weight management
Subject: Question about wellness stipend eligibility for GLP-1 care
Hi [Benefits Admin],
I'd like to confirm whether physician-supervised weight-management care with a GLP-1 prescription is an eligible expense under our wellness stipend or LSA. I'd be paying for a telehealth program and prescribed medication through a licensed provider and planning to submit itemized receipts for reimbursement.
If eligible, what documentation would you need, and which category should I file it under?
Thanks!
The answer is usually yes. Even when it isn't pre-listed, many employers will approve weight management as a case-by-case category when asked directly.
Compounded vs. FDA-Approved: What Matters for a Stipend Claim
When FDA-approved is the safer stipend play
- Stipend policy explicitly says "FDA-approved" or "pharmacy-grade"
- Benefits admin has previously rejected compounded medication claims
- Employer is risk-averse about reimbursing non-FDA-approved treatments
- You want to avoid the regulatory context around compounded providers
→ Go to Sesame Care or Ro
When compounded cash-pay still makes sense
- Stipend language written broadly ("weight management," "prescription medications")
- You want flat monthly pricing — compounded typically runs $249–$299/month
- Stipend amount is modest and brand-name math doesn't work
- You're comfortable with the clinical trade-off of a non-FDA-evaluated product
→ Go to MyStart Health or Eden
How to Submit a Wellness Stipend Claim Without a Denial
The four documents to save every time
- 1Itemized invoice: Showing provider name, medication or program name, date, and amount. A charge labeled "monthly subscription" typically won't pass.
- 2Proof of payment: Credit card confirmation or bank statement line matching the charge.
- 3Prescription details: Usually included on the invoice; request from provider support if not.
- 4Plan / checkout summary: The page that listed what you purchased and the total.
If your claim is denied
Fix: Request an accurate itemized receipt from your provider's support team showing medication, date, and amount as separate line items. Every provider in our comparison can produce one.
Fix: Request an accurate receipt that truthfully reflects the service and medication you purchased. Do not ask a provider to relabel a charge in a way that misrepresents what you bought.
Fix: Request from your prescribing clinician. Many providers issue within 24–48 hours on request; confirm availability with your specific provider.
Stack — don't double-dip
- • Insurance pays the prescription claim if GLP-1 is covered
- • HSA / FSA pays any remaining out-of-pocket copay or coinsurance
- • Wellness stipend pays adjacent costs your HSA/FSA doesn't cover
You cannot reimburse the same dollar from both HSA and your stipend. Audits catch it.
Providers We Don't Lead With for This Use Case
Yucca Health — Not Recommended for Stipend Users
Yucca Health's own FAQ states that they do not provide itemized receipts. For a page specifically about stipend reimbursement, that's disqualifying — itemized receipts are the single most common documentation requirement. If you were considering Yucca, MyStart Health is the better path because it produces exactly what Yucca doesn't.
MEDVi and SkinnyRx — Why They're Not the Top Picks Here
MEDVi and SkinnyRx were among approximately 30 telehealth providers receiving FDA warning letters in March 2026 regarding compounded GLP-1 marketing. Both remain operational. Neither company's documentation workflow for stipend reimbursement is as explicitly published as MyStart's or Hims/Hers'. For this use case, MyStart or Eden are cleaner starting points.
What We Actually Verified on This Page
Verified :
- ✓MyStart Health — $299/month flat pricing, published reimbursement documentation pack, 50-state clinician availability, cancel-anytime with refunds before shipment (verified at mystarthealth.com/hsa, April 2026)
- ✓Eden — HSA/FSA eligibility across plans, compounded semaglutide from $249/month, tirzepatide from $349/month, 50-state GLP-1 program availability, three-month prepaid commitment for compounded plans (verified at tryeden.com, April 2026)
- ✓Sesame Care — Success by Sesame subscription from $59/month annual plan, itemized bill via [email protected], FDA-approved Wegovy (injection and pill), Zepbound, and Foundayo (verified at sesamecare.com, April 2026)
- ✓Ro — $39 first month, $149/month standard, $74/month with annual plan paid upfront, FDA-approved Zepbound and Foundayo, 50 states + D.C. (verified at ro.co/weight-loss/pricing, April 2026)
- ✓Hims / Hers — $39 first month, $149/month membership, published reimbursement workflow at hims.com/weight-loss/fsa-hsa and forhers.com/weight-loss/fsa-hsa (verified April 2026)
- ✓Willow — $299/month program pricing, HSA/FSA at checkout, two-business-day cancellation cutoff (verified at startwillow.com, April 2026)
- ✓Compt — Published GLP-1 stipend guidance at compt.io (verified April 2026)
- ✓Forma — Weight Management HRA product at joinforma.com (verified April 2026)
- ✓Espresa — Specialty Care Account product for GLP-1 at espresa.com (verified April 2026)
- ✓HealthEquity LSA — LSA reimbursement model and processing time at HealthEquity support documentation (verified April 2026)
- ✓Benepass, Fringe, PeopleKeep — Payout model descriptions verified from each platform's public positioning (verified April 2026)
- ✓IRS Section 132(e) de minimis fringe — Confirmed via IRS and Compt's published guidance (verified April 2026)
- ✓FDA warning letters to compounded GLP-1 telehealth providers — Confirmed via FDA releases, September 2025 and March 2026 (verified April 2026)
- ✓Yucca Health itemized receipt policy — Confirmed at tryyucca.com/frequently-asked-questions (verified April 2026)
Items not individually verified: employer-specific plan exclusions, state-by-state Willow footprint, individual plan-admin substantiation requirements for LSAs.
Refresh cadence: Last verified · Next scheduled: May 17, 2026 (monthly pricing; quarterly policy language; immediate on material FDA changes).
Frequently Asked Questions
Still Not Sure Which GLP-1 Program Is Right for You?
Every employer's wellness stipend rules are different. Every GLP-1 provider fits a slightly different stipend type. The fastest way to match your benefit type, stipend amount, state, and medication preference.
Take the free 60-second GLP-1 matching quiz →Already know what you want?