
GLP-1 Missed Period: What To Do First If You’re Late on Ozempic, Wegovy, Mounjaro, or Zepbound
By the WPG Editorial Team · Editorial Standards · Affiliate Disclosure · 14 min read
Last updated: · Last verified: · Next audit:
Informational only, not medical advice. If your period is late and there’s any chance of pregnancy, take a home test today. If you have severe pelvic pain, heavy bleeding, fainting, or shoulder pain, seek urgent medical care now.
Affiliate disclosure: We’re an independent comparison resource. We don’t sell medication. We may earn a commission if you sign up through links to providers we mention. That doesn’t change our editorial framing.
A GLP-1 missed period almost never means the medication directly stopped your cycle. We reviewed the current FDA labels for Ozempic, Wegovy, Rybelsus, Mounjaro, Zepbound, and Foundayo — and missed period (or amenorrhea, the medical term) isn’t listed as a named adverse reaction on any of them. What you actually need to know is this: pregnancy comes first, and one specific drug class on this list — tirzepatide, plus the new oral medication orforglipron — carries a real birth control absorption warning that most articles either skip or get wrong.
We’re an independent comparison resource for GLP-1 telehealth providers. We don’t sell medication. We’re not your doctor. What we did was read every current FDA label for the medications on this page, the most-cited 2024–2026 medical literature, the Faculty of Sexual & Reproductive Healthcare clinical guidance on GLP-1s and oral contraception, and the Natural Cycles analysis of 1,754 GLP-1 users — then put the answers in one place so you don’t have to open ten tabs at midnight.
Read this first if you take Mounjaro, Zepbound, or Foundayo and use birth control pills. Per the FDA labels, these medications can reduce how well your pill is absorbed for 4 weeks after starting and 4 weeks after each dose increase (Mounjaro/Zepbound), or 30 days (Foundayo). If your period is late and you’ve been in one of those windows, take a pregnancy test today.
Quick triage: what to do right now
| If this is you | Do this first |
|---|---|
| Pregnancy is possible and you’re more than a week late | Take a home pregnancy test now. Use first-morning urine. Repeat in 3–4 days if negative and your period still hasn’t come. |
| You take Mounjaro, Zepbound, or Foundayo and use the pill | Test today. Then ask your prescriber about switching to a non-pill method (IUD, implant, ring, patch, or injection) or adding condoms. |
| You take Ozempic, Wegovy, or Rybelsus and there’s any chance of pregnancy | Test today. Semaglutide doesn’t carry the same pill warning, but pregnancy still needs ruling out. |
| You vomited or had diarrhea within hours of taking your pill | Treat it as a missed pill. Add a barrier method or follow your pill packet’s missed-pill rules. Test if you’re late. |
| You have severe pelvic pain, heavy bleeding, fainting, or shoulder pain | Seek urgent medical care. Do not wait for an online answer. |
| You’ve missed three or more periods in a row | Contact your prescriber or OB-GYN this week, even if your tests are negative. |
| You’re not pregnant, no urgent symptoms, but worried | Track your next cycle. Most cycle changes settle as your weight, dose, and intake stabilize. |
Not sure what to do next?
Get a personalized triage checklist — pregnancy test timing, prescriber message, contraception question, or urgent-care flag — based on your medication, cycle day, dose timing, and symptoms.
Open the GLP-1 missed-period triage tool →What we actually found in the FDA labels
We pulled the current prescribing information for every medication on this page directly from FDA-approved labels (via DailyMed and FDA.gov). Here’s the row-by-row scan, so you can see exactly what each drug says and what it doesn’t:
| Medication | Active ingredient | Status | Missed period listed? | Oral contraceptive warning? | Backup contraception window | Pregnancy instruction |
|---|---|---|---|---|---|---|
| Ozempic | Semaglutide | FDA-approved (T2D) | No | No | None labeled | Stop at least 2 months before a planned pregnancy |
| Wegovy | Semaglutide | FDA-approved (weight) | No | No | None labeled | Discontinue when pregnancy is recognized |
| Rybelsus | Semaglutide (oral) | FDA-approved (T2D) | No | No | None labeled | Stop at least 2 months before a planned pregnancy |
| Mounjaro | Tirzepatide | FDA-approved (T2D) | No | Yes | 4 weeks after starting + 4 weeks after each dose increase | Use only if benefit justifies fetal risk |
| Zepbound | Tirzepatide | FDA-approved (weight) | No | Yes | 4 weeks after starting + 4 weeks after each dose increase | Discontinue when pregnancy is recognized |
| Foundayo | Orforglipron | FDA-approved April 1, 2026 (weight) | No | Yes | 30 days after starting + 30 days after each dose increase | Discontinue when pregnancy is recognized |
Sources: FDA prescribing information accessed via DailyMed and FDA.gov. Last verified .
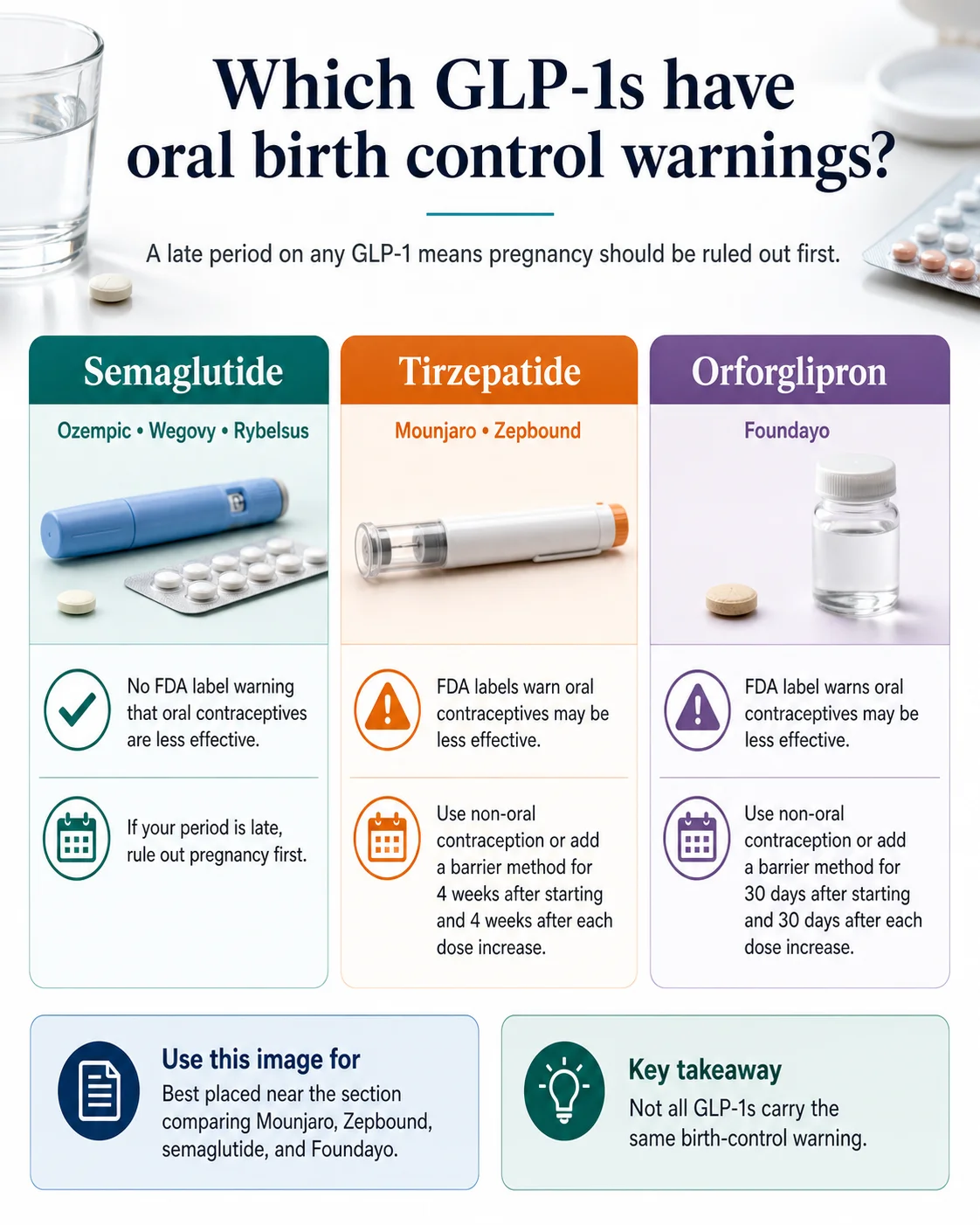
Two things matter most in this table. First, none of these labels list missed periods as a known adverse reaction — that’s why claiming GLP-1s “stop your period” doesn’t match what’s on the label. Second, the contraceptive warning isn’t universal. It applies to tirzepatide (Mounjaro and Zepbound) and orforglipron (Foundayo). It does not apply to semaglutide (Ozempic, Wegovy, Rybelsus). That distinction changes what you should actually do tonight.
Can a GLP-1 actually cause a missed period?
Short answer: Not directly. GLP-1 medications don’t act on the hormones that run your cycle (estrogen, progesterone, LH, FSH). They mimic a gut hormone that controls appetite, blood sugar, and how fast your stomach empties. None of those touch ovulation directly. When women experience period changes on a GLP-1, the cause is almost always indirect — fast weight loss, shifts in insulin sensitivity, low food intake, or, with two specific drug classes, reduced absorption of birth control pills.
That’s the answer most affiliate sites won’t give you straight. They hint at it. They say “may affect your cycle.” They list “missed periods” alongside nausea like the two are equivalent side effects. They’re not. Missed periods aren’t on any FDA label for the medications above. Nausea is. The difference matters because it changes what you should do tonight.
Here’s what the evidence shows. A 2024 Natural Cycles analysis surveyed 1,754 GLP-1 users about their cycles. 27% noticed changes. Among the most common reported changes, 45% of all respondents and 64% of respondents with PCOS reported their periods became more predictable. That doesn’t sound like a medication that’s “stopping” cycles. It sounds like one whose downstream effects on weight and insulin can shift cycles in either direction depending on where you started.
So if it’s not the drug itself, what is it?
The three real reasons your period changed
1. Rapid weight loss. Body fat (adipose tissue, the medical term) is hormonally active — it produces estrogen. When you lose weight quickly, estrogen production drops and your brain reads “low energy availability” as a stress signal. The hypothalamus (the part of your brain that controls reproductive hormones) can pause ovulation in response. Doctors call this hypothalamic amenorrhea — literally “no period from the hypothalamus.” It’s well-documented in athletes, in people with eating disorders, and in anyone losing weight fast.
2. Insulin and metabolic shifts. GLP-1s improve insulin sensitivity. For most women, this is neutral or positive. For women with PCOS — polycystic ovary syndrome, a hormonal condition where insulin resistance and elevated androgens often interfere with ovulation — improved insulin sensitivity often normalizes cycles. The Natural Cycles 64% figure for PCOS isn’t an accident. A small 2023 study by Carmina and colleagues followed 27 women with obesity and PCOS who hadn’t responded to lifestyle programs and reported normalized cycles in roughly 80% of semaglutide responders.
3. Birth control absorption — for tirzepatide and orforglipron specifically. This is the one most pages miss, and it’s the most actionable. Tirzepatide (Mounjaro, Zepbound) and orforglipron (Foundayo) slow your stomach emptying enough that birth control pills may not absorb as well. Both labels include an explicit warning. Semaglutide (Ozempic, Wegovy, Rybelsus) does not carry the same warning — and a 2024 systematic review by Skelley and colleagues, summarized in National Geographic, concluded semaglutide doesn’t reduce oral contraceptive absorption in a clinically meaningful way.
So when your period is late, the question isn’t really “did my GLP-1 stop my cycle.” The questions are: Could I be pregnant? Am I on a drug with the pill warning? Have I lost weight fast? Did I throw up or have diarrhea after my pill? Is something else going on?
That’s the order. Let’s go through it.
What to do today if your period is late on a GLP-1
Short answer: Take a home pregnancy test. Use first-morning urine for the most reliable result. If it’s negative and your period still doesn’t come within 3–4 days, repeat the test — or ask your prescriber for a quantitative blood test. If you’re on Mounjaro, Zepbound, or Foundayo and use the pill, test sooner rather than later — those medications can reduce how well your pill is absorbed during specific windows.
Here’s the thing about pregnancy tests that almost no GLP-1 article explains clearly: timing is the whole game. The FDA says home pregnancy tests are most reliable starting after a missed period, and even more reliable 1–2 weeks after. The Office on Women’s Health adds that some tests aren’t sensitive enough to catch a pregnancy on day one — so a negative test on the day your period was supposed to start doesn’t fully rule out pregnancy.
That’s why the right move when you’re late is usually:
Step 1: Test now if you’re at least a day late. Use the first urine of the morning. It has the highest concentration of hCG (the pregnancy hormone the test is detecting). Follow the instructions exactly. Test sensitivity varies by brand — read the package for the lowest hCG level it can detect.
Step 2: Test again in 3–4 days if your period still hasn’t come. Especially if you tested very early. Some pregnancies don’t produce enough hCG to register on a home test until you’re 1–2 weeks past your missed period.
Step 3: Ask about a blood test if you’re more than a week late and home tests keep coming up negative. Quantitative blood tests can detect pregnancy earlier and more reliably. Most prescribers and OB-GYN offices can order one.
If your test is positive, contact your prescriber or OB-GYN today — not next week — before taking another dose of your medication. Different GLP-1 labels handle pregnancy differently: Wegovy, Zepbound, and Foundayo instruct stopping when pregnancy is recognized; Ozempic and Rybelsus emphasize stopping at least 2 months before a planned pregnancy; Mounjaro says use during pregnancy only if the benefit justifies the fetal risk. Your prescriber will know which instruction applies and can guide you on next steps, including whether to enroll in the manufacturer’s pregnancy exposure registry.
If your test is negative and you’re still late, keep reading. There are several reasons this happens, and most are not emergencies.
When a missed period on a GLP-1 is actually urgent
Short answer: Most missed periods aren’t emergencies. But certain symptom combinations are. Severe pelvic or abdominal pain, heavy bleeding, shoulder pain (especially with a positive pregnancy test), fainting, fever, or foul-smelling discharge all warrant urgent care today, not a wait-and-see approach. A missed period plus any of these symptoms could indicate ectopic pregnancy, pelvic infection, or another condition that needs evaluation now.
We’re putting this section second because it’s the part of triage that actually saves lives, and we don’t want it buried.
Symptoms that mean go to urgent care or the ER today
- Severe one-sided pelvic or abdominal pain — especially with a positive pregnancy test or a possibility of pregnancy. This can signal an ectopic pregnancy, when a fertilized egg implants outside the uterus, usually in a fallopian tube. Mayo Clinic flags severe pelvic pain with vaginal bleeding as a potential emergency symptom.
- Shoulder pain — sounds odd, but in someone who could be pregnant, shoulder pain can indicate internal bleeding from a ruptured ectopic. Don’t ignore it.
- Fainting, severe lightheadedness, or feeling like you’re going to pass out — possible signs of internal bleeding or significant blood loss.
- Heavy bleeding — soaking through a pad or tampon every hour for several hours in a row, or passing large clots.
- Fever above 101°F with pelvic pain or unusual discharge — possible pelvic infection.
- Severe pain that’s not relieved by over-the-counter pain medication.
Symptoms that mean call your prescriber or OB-GYN within a few days
- You’ve missed three or more periods in a row.
- You’re spotting between periods for more than a few days.
- Your bleeding pattern has changed dramatically from your normal baseline.
- You think you might be pregnant but tests are negative.
- You have a history of hormonal disorders (PCOS, thyroid issues, premature ovarian insufficiency) and your cycle just changed significantly.
- You’ve lost a lot of weight quickly and your period stopped.
Symptoms that mean you can probably track and wait
- One late or skipped period, no other symptoms, you’re not sexually active or pregnancy is impossible.
- A cycle that came a week early or late but is otherwise normal in flow.
- A lighter or shorter period than usual after starting a GLP-1, with no other concerning signs.
If you’re ever uncertain, call. That’s not us hedging — it’s the actual right answer in YMYL medicine.
Mounjaro and Zepbound: the birth control warning that matters most
Short answer: Yes, tirzepatide (the active ingredient in both Mounjaro and Zepbound) can make birth control pills less effective. The FDA prescribing information for both drugs says to either switch to a non-oral contraceptive method or add a barrier method (condoms, diaphragm) for 4 weeks after you start the medication and 4 weeks after every dose increase. This is the single most important medication-specific fact on this entire page.
Here’s why. Tirzepatide slows gastric emptying — the rate at which food (and pills) move from your stomach into your small intestine where they get absorbed. The effect is most pronounced when you first start the drug and when you increase your dose. During those windows, your birth control pill may not be absorbed well enough to reliably prevent pregnancy.
Eli Lilly’s own FDA-approved labels for Mounjaro and Zepbound say this directly. The MotherToBaby fact sheet from OTIS (the Organization of Teratology Information Specialists) reinforces it: tirzepatide may change how oral birth control pills are absorbed, which might increase the chance of pregnancy even if the pill is taken correctly and consistently.
What the pharmacokinetic data actually shows
In Lilly’s own clinical study, tirzepatide reduced overall exposure (AUC) to ethinyl estradiol by about 20% and reduced the peak concentration more substantially. The Faculty of Sexual & Reproductive Healthcare — the UK’s specialist body on contraception — reviewed this evidence and concluded that the effect on oral contraceptive absorption is clinically relevant for tirzepatide, while semaglutide’s effect on absorption was not clinically relevant in their review. That’s why the two drugs get different treatment in the labels.
This is also why the “Ozempic babies” stories you’ve seen — surprise pregnancies in women on weight-loss medication — are more often tirzepatide babies in cases where birth control was the only protection. The mechanism is real and documented.
What to actually do if you’re on Mounjaro or Zepbound and use the pill
The FDA label gives you three options:
- Switch to a non-oral contraceptive method. IUD, implant, injection (Depo-Provera), patch, or vaginal ring. None of these depend on stomach absorption.
- Add a barrier method (condoms or diaphragm) for the 4-week windows after starting and after each dose increase.
- Talk to your prescriber about both. This is the right call for most people, because the timing of dose increases isn’t always predictable.
Copy-paste this message to your prescriber
If you’re not sure how to start the conversation, paste this directly into your provider’s secure messaging portal:
Hi — I’m taking [Mounjaro / Zepbound] at [dose]. I’m on [pill name or “combined oral contraceptive”]. My period is now [X] days late. I started or increased my dose on [date]. I’d like to know whether I should: (1) take a pregnancy test now, (2) add a barrier method, (3) switch to a non-oral birth control method, or (4) all of the above. What do you recommend?
This message takes 90 seconds to fill out and gives your prescriber every piece of information they’d otherwise spend an appointment trying to extract.
Send the right message now
Open our prescriber-message builder to fill in your dose date, cycle day, birth-control method, and test result, then send a clean, complete message in under two minutes.
Open the prescriber-message builder →Ozempic, Wegovy, and Rybelsus: what semaglutide does (and doesn’t) do to your cycle
Short answer: Semaglutide — the active ingredient in Ozempic, Wegovy, and Rybelsus — does not have an FDA contraceptive interaction warning on its labels. A 2024 systematic review by Skelley and colleagues, plus the FSRH clinical guidance, concluded semaglutide doesn’t reduce oral contraceptive concentrations in the bloodstream in a clinically meaningful way. If your period is late on Ozempic or Wegovy, the cause is more likely weight loss, insulin shifts, or pregnancy than the medication interfering with your pill. Semaglutide labels for Ozempic and Rybelsus do recommend stopping the medication at least 2 months before a planned pregnancy; Wegovy’s label instructs discontinuation when pregnancy is recognized.
This is one of the biggest information gaps on the internet right now. Most articles lump every GLP-1 together and tell you to add backup contraception “just in case.” That’s overcautious advice that doesn’t match the FDA labels. Semaglutide and tirzepatide aren’t the same drug, and the FDA didn’t write the same warnings for them.
What the semaglutide labels actually say
The FDA prescribing information for Wegovy, Ozempic, and Rybelsus all include pregnancy-related instructions, and Ozempic and Rybelsus specifically recommend stopping at least 2 months before a planned pregnancy because semaglutide has a long half-life (it stays in your system for weeks after the last dose). But none of these labels include an oral contraceptive interaction warning, because the pharmacokinetic studies didn’t support one.
Skelley et al. searched the medical literature for studies measuring how much oral birth control got into people’s bloodstream while they were on GLP-1s. Their finding for semaglutide: no meaningful reduction in oral contraceptive levels, no clinically relevant delay in absorption. National Geographic’s November 2025 piece on the “Ozempic baby boom” cited the same review.
So why are women on Ozempic still getting pregnant unexpectedly?
Two reasons:
1. Weight loss can restore fertility. Many women with PCOS, obesity-related insulin resistance, or metabolic syndrome aren’t ovulating regularly to begin with. GLP-1s improve the metabolic conditions that suppress ovulation. When ovulation comes back, fertility comes back. This isn’t a side effect — it’s the medication treating a contributing cause of infertility. For women trying to conceive, it’s good news. For women on a GLP-1 who don’t want to be pregnant, it means contraception matters more than ever.
2. Pregnancy is still possible while taking any medication. No medication is contraception. If you don’t want to be pregnant, contraception is the answer — semaglutide just doesn’t interfere with the pill the way tirzepatide does.
What this means if your period is late on Ozempic or Wegovy
- Take a pregnancy test if there’s any chance of pregnancy.
- If it’s negative and your period is still late, consider weight loss, insulin shifts, stress, or other causes (covered below).
- You don’t need to add backup contraception based on FDA labeling alone, but talk to your prescriber if you have questions.
- If you’re trying to conceive, plan to stop semaglutide at least 2 months before you start trying.
For more on semaglutide as a class, see our best online Ozempic provider and best online Wegovy provider guides.
Foundayo (orforglipron): the newest GLP-1 and the longest contraception window
Short answer: Foundayo is an oral once-daily small-molecule GLP-1 tablet, FDA-approved on April 1, 2026, and marketed as the GLP-1 pill for weight loss that can be taken any time of day without food or water restrictions. Per the FDA prescribing information, Foundayo can reduce oral contraceptive effectiveness, and the label recommends switching to a non-oral method or adding a barrier method for 30 days after starting and 30 days after each dose increase. Most articles haven’t been updated to include Foundayo yet — but if you’re on it and use the pill, the warning applies to you.
Foundayo is brand-new. We’re including it because the FDA approved it less than five weeks before this article’s publish date, and almost no other site has updated their content to reflect it. If you’re searching “GLP-1 missed period” and you’re on Foundayo, here’s the straight answer.
What Foundayo’s label says
Foundayo (orforglipron, made by Eli Lilly) delays gastric emptying. The Lilly Medical FAQ on Foundayo notes that the effect of Foundayo on oral contraceptive absorption hasn’t been evaluated in a dedicated clinical trial — but because delayed gastric emptying may affect oral medications, the label recommends switching to a non-oral contraceptive method or adding a barrier method for 30 days after starting and 30 days after each dose escalation. The label states the medication may make birth control pills work less well at preventing pregnancy during those windows.
What to do if you’re on Foundayo and your period is late
Same playbook as tirzepatide:
- Take a pregnancy test today.
- Note when you started the medication and when your last dose increase was.
- If you’re within 30 days of starting or increasing, treat your pregnancy risk as elevated relative to a non-pill backup.
- Message your prescriber about contraception options. If you’re using the pill alone, you’ll likely be advised to add a barrier method or switch to a non-oral method.
If you become pregnant on Foundayo, the label instructs discontinuation when pregnancy is recognized. Eli Lilly maintains a Foundayo Pregnancy Registry (1-800-545-5979) to track outcomes for women who become pregnant while on the medication. For more on Foundayo as a medication option, see our best Foundayo providers and cheapest Foundayo online guides.
What if I vomited or had diarrhea after taking my birth-control pill?
Short answer: Treat it as a missed pill. Vomiting within about two hours of taking a combined oral contraceptive — or severe diarrhea — can prevent the pill from being absorbed properly. Per FSRH guidance, if you vomit or have severe diarrhea after taking your pill, follow the missed-pill rules in your packet leaflet (typically: take the next pill on schedule, and add a barrier method or abstain for 7 days if it happens repeatedly). For GLP-1 users, this matters more than it would otherwise — because nausea and GI side effects are common, especially during titration.
This is a question almost no GLP-1 page bothers to answer, and it’s directly relevant to a missed period. Here’s the practical version:
When this matters
- Within ~2 hours of taking your pill. That’s the absorption window. Vomiting before the pill is absorbed is functionally a missed pill.
- Severe diarrhea. Several loose stools in a row can also reduce absorption, especially with the lower-dose combined pills.
- Repeated GI symptoms across several days. Even if any single episode wouldn’t qualify as “missed pill,” a pattern can compound risk.
What to do
- Take your next pill as scheduled.
- Add a barrier method (condoms) for at least the next 7 days, or longer if your pill packet specifies more.
- Read your specific pill leaflet’s missed-pill rules. Different pills have different rules; combined pills and progestogen-only pills are not the same.
- Test if you’re late. If your period is now late and you’ve had GI episodes, the missed-pill risk plus the GLP-1 absorption issue (if you’re on tirzepatide or Foundayo) compound.
- Message your prescriber if it’s recurring. Repeated nausea or vomiting on a GLP-1 is a sign your dose may need adjustment, not a sign to suffer through it.
If GI side effects are knocking you out for hours every dose, your titration plan probably needs reconsideration. Our GLP-1 nausea: what to eat guide can help in the short term, but persistent vomiting is a conversation worth having before another missed period happens.
Compounded semaglutide and tirzepatide: what to know if your period is late
Short answer: Compounded GLP-1 products are not FDA-approved finished products. They may vary in formulation, concentration, packaging, instructions, and quality review. If your period is late on a compounded medication, follow the same pregnancy-first triage, then contact the specific prescriber and pharmacy that issued your prescription for product-specific pregnancy and contraception guidance. Don’t assume the patient labeling for Ozempic, Wegovy, Mounjaro, Zepbound, or Foundayo applies to a compounded product.
Here’s the regulatory reality, explained plainly. The FDA approves finished drug products — that’s what Ozempic, Wegovy, Mounjaro, Zepbound, and Foundayo are. Compounded medications are made by pharmacies that prepare a customized version, often when the FDA-approved version is in shortage or when a patient needs a specific formulation. The FDA states that unapproved GLP-1 drugs have not undergone FDA review for safety, effectiveness, or quality. The agency has also issued warnings about dosing errors with compounded injectable semaglutide and unapproved GLP-1 products sold directly to consumers.
What that means for your missed period:
- The pharmacology of the active ingredient guides expectations, but compounded products don’t carry the same FDA-reviewed patient labeling.
- If your compounded prescription is described as tirzepatide and you use oral hormonal contraception, ask your prescriber whether to follow the FDA-approved tirzepatide label’s 4-week non-oral or barrier contraception window.
- If your compounded prescription is described as semaglutide, ask your prescriber and pharmacy for product-specific instructions — don’t assume it has the same review or labeling as Ozempic, Wegovy, or Rybelsus.
- If you bought your medication from a “research use only” supplier or anywhere outside a licensed prescriber-pharmacy relationship, contact a licensed healthcare provider promptly and don’t rely on that seller for medical guidance.
What to verify if you’re on a compounded GLP-1
| Verify this | Why it matters |
|---|---|
| Your prescriber’s name and license | You need someone medically responsible for your care |
| Your pharmacy’s name and license | 503A and 503B compounding pharmacies are state and federally regulated; “research-only” suppliers are not |
| The medication form (injection, oral, sublingual) | Different forms have different absorption profiles |
| The exact dose in milligrams or units | Dosing errors are a documented risk with compounded injectables |
| Pregnancy and contraception guidance from your prescriber | Compounded products may not include the same patient leaflets as branded medications |
One regulatory development worth knowing
On April 30, 2026, the FDA proposed excluding semaglutide, tirzepatide, and liraglutide from the 503B bulks list — the list that allows certain outsourcing facilities to compound these drugs from bulk active ingredients. The public comment period runs through June 29, 2026. Whether and how this proposal is finalized could materially change compounded GLP-1 availability later in 2026. If you’re on a compounded product, ask your prescriber and pharmacy how they’re tracking this and what your access plan looks like if rules change.
If your prescriber and pharmacy can’t or won’t answer the verification questions above, you’re in the wrong relationship. We talk about how to find a better-supported GLP-1 path further down.
Can rapid weight loss stop your period?
Short answer: Yes. Rapid or substantial weight loss, undereating, low body fat, excessive exercise, and stress can all pause your menstrual cycle through a process called hypothalamic amenorrhea — your brain interpreting an energy shortage as a stress emergency and temporarily halting ovulation. Cleveland Clinic notes that when the underlying energy or stress issue is treated consistently, it most often takes 3–6 months to begin menstruating again. If you have no period for 3 months, get evaluated.
This is the indirect mechanism most likely to be behind your missed period if pregnancy is ruled out and you’re on a GLP-1.
Here’s how it works in plain terms. Your hypothalamus (the small region of your brain that controls reproductive hormones) is constantly reading two signals: your weight and your energy intake. If either drops fast enough, it interprets the change as a stress event and pumps the brakes on the hormones that drive ovulation. No ovulation means no period — sometimes for one cycle, sometimes for several months.
Athletes get this. People on aggressive diets get this. And now, some people losing weight rapidly on GLP-1s get it too. It’s not the medication doing it directly; it’s the speed of the weight change combined with reduced food intake. Cleveland Clinic confirms that significant weight loss, restrictive eating, over-exercising, and stress can all disrupt your cycle.
How fast is too fast?
Clinical guidance generally points to 1–2 pounds per week as a sustainable weight-loss rate. GLP-1 trials average within this range over the long term — the STEP and SURMOUNT trials for Wegovy and Zepbound averaged about 15–20% body weight loss over 68–72 weeks. But early in treatment, when nausea suppresses appetite hard, some people lose much faster than that for a few weeks.
If you’ve lost weight rapidly — especially if you’ve crossed about 10% of your starting body weight in a short time — your cycle change is more likely about pace and intake than about anything intrinsic to the medication.
Practical things you can do
We’re not going to give you a diet plan. We will tell you what’s worth bringing up with your prescriber:
- Protein. Aim for about 0.7 grams per pound of your goal body weight. Reduced appetite on GLP-1s makes it easy to undereat protein, which compounds the metabolic stress.
- Calories that aren’t zero. “Eating less” isn’t the same as “eating nothing.” If you’re going whole days without meals because you’re not hungry, your body reads that as a famine signal regardless of why you’re not eating.
- Iron, vitamin D, and B12. All three matter for cycle regularity and all three are easy to under-consume when appetite is suppressed.
- Sleep and stress. Cortisol disrupts the same hypothalamic signals as weight loss does. Both stack.
- Talk to your prescriber about titration speed. If you’ve lost weight very fast, ask whether holding your current dose for an extra month before the next increase makes sense.
If your missed period is hypothalamic amenorrhea and you’re consistently treating the underlying issues, Cleveland Clinic’s window for periods returning is about 3–6 months. If yours doesn’t return in that timeframe — or if you’ve gone three months with no period — that’s a signal to escalate to your prescriber or OB-GYN.
Could you actually be pregnant? The “Ozempic babies” question
Short answer: Yes — pregnancy is possible on any GLP-1, and unexpected pregnancies on GLP-1s are widely reported. The mechanisms are clinically plausible: GLP-1s can improve metabolic health enough to restore ovulation (especially in PCOS or obesity-related anovulation), and tirzepatide and orforglipron specifically reduce how well oral birth control absorbs during their dosing windows. Human pregnancy-safety data for GLP-1s is still limited. If your period is late and there’s any chance of pregnancy, test today before assuming the medication is the cause.
The “Ozempic babies” thing started as social media language and became a clinical observation. Cleveland Clinic, University Hospitals, Endocrinology Advisor, and National Geographic have all covered it. It refers to women who became pregnant unexpectedly after starting a GLP-1 — often after years of difficulty conceiving.
There are two distinct mechanisms behind it, and they don’t overlap as much as people think:
Mechanism 1: Restored ovulation. Many women with PCOS, obesity-related insulin resistance, or metabolic syndrome aren’t ovulating regularly to begin with. GLP-1s improve the metabolic conditions that suppress ovulation. When ovulation comes back, fertility comes back. This isn’t a side effect — it’s the medication treating a contributing cause of infertility. For women trying to conceive, it’s good news. For women on a GLP-1 who don’t want to be pregnant, it means contraception matters more than ever.
Mechanism 2: Reduced pill absorption (tirzepatide and orforglipron only). This is the one we’ve covered above. It applies to Mounjaro, Zepbound, and Foundayo, and only during specific dosing windows.
What to do if your test is positive
Contact your prescriber or OB-GYN today before taking another dose. The exact instruction depends on your medication: Wegovy, Zepbound, and Foundayo labels instruct discontinuation when pregnancy is recognized; Ozempic and Rybelsus emphasize stopping at least 2 months before a planned pregnancy; Mounjaro’s label says use during pregnancy only if the benefit justifies the fetal risk. Your prescriber will know which instruction applies and can guide you on next steps, including whether to enroll in the manufacturer’s pregnancy exposure registry.
Pregnancy registries by manufacturer
| Medication | Manufacturer | Registry contact |
|---|---|---|
| Mounjaro / Zepbound / Foundayo | Eli Lilly | 1-800-LillyRx (Foundayo registry: 1-800-545-5979) |
| Ozempic / Wegovy / Rybelsus | Novo Nordisk | Ask your prescriber for current enrollment info |
Some reassurance, with appropriate caveats. A small prospective cohort study of 168 first-trimester GLP-1-exposed pregnancies found no increased risk of major birth defects or pregnancy loss compared with reference groups of pregnant women with diabetes and overweight or obesity. The authors emphasized the small sample size and the need for larger studies. This is not a green light to use GLP-1s during pregnancy — they’re not approved for use in pregnancy, and animal studies show developmental concerns. But if you’ve already been exposed during early pregnancy, the available human data so far is reassuring.
How long until it’s safe to try to conceive after stopping?
This depends on your medication:
| Medication | Active Ingredient | Pre-pregnancy guidance |
|---|---|---|
| Ozempic / Rybelsus | Semaglutide | Label recommends stopping at least 2 months before a planned pregnancy |
| Wegovy | Semaglutide | Discontinue when pregnancy is recognized; ask prescriber about pre-conception planning |
| Mounjaro / Zepbound | Tirzepatide | MotherToBaby reports it can take, on average, up to 30 days for most tirzepatide to be cleared. Ask your prescriber for pre-conception guidance |
| Foundayo | Orforglipron | Discontinue when pregnancy is recognized; pre-conception planning should be discussed with your prescriber |
Sources: Each medication’s current FDA prescribing information, plus MotherToBaby fact sheets from OTIS.
GLP-1s and PCOS: when a missed period is actually a sign of progress
Short answer: If you have PCOS, evidence suggests cycles may become more regular for some responders on a GLP-1 — not less. The Natural Cycles 2024 analysis found 64% of GLP-1 users with PCOS reported more predictable periods. The small 2023 Carmina study of 27 obese women with PCOS who hadn’t responded to lifestyle programs reported that, among semaglutide responders, about 80% saw their cycles normalize. So if you have PCOS, your cycles got more regular on a GLP-1, then suddenly stopped — pregnancy is the first thing to rule out, because restored fertility is real and well-documented.
PCOS is a hormonal condition where insulin resistance and elevated androgens (male-pattern hormones) interfere with ovulation. Many women with PCOS go months without a period, then have an unpredictable one. GLP-1s can change that picture for some.
Here’s what tends to happen:
- You start a GLP-1.
- Your insulin sensitivity improves.
- Your ovaries respond by ovulating more regularly.
- Your periods become more predictable.
- You may now be more fertile than you’ve been in years — possibly without realizing it.
If you went from years of irregular cycles to several months of regular ones, then your last period didn’t come — that’s a major fertility change you should treat seriously. Take a pregnancy test today. If it’s negative, retest in 3–4 days. If you weren’t actively trying to prevent pregnancy because you assumed you were less fertile, talk to your prescriber about contraception that fits your medication.
The 2023 international PCOS guideline and a 2025 GLP-1 receptor agonist meta-analysis in Scientific Reports both recognize GLP-1s as an option for weight management in higher-weight adults with PCOS, while emphasizing effective contraception when pregnancy isn’t the goal — because of exactly the fertility-restoration dynamic we just described. For more on this medication path, see our best GLP-1 for PCOS guide.
What if my pregnancy test is negative but my period is still late?
Short answer: A negative test on day one of a missed period doesn’t fully rule out pregnancy. Some pregnancies don’t produce enough hCG to register on a home test until you’re 1–2 weeks past your missed period. Repeat the test with first-morning urine in 3–4 days, or ask your prescriber for a quantitative blood test. If you’re consistently testing negative and your period still doesn’t come within 3 months, contact your prescriber or OB-GYN even if pregnancy seems impossible — that’s the threshold for medical evaluation regardless of cause.
This is one of the most anxiety-driving searches in this whole topic, and it deserves a clear answer.
Reasons a pregnancy test can be negative when you actually are pregnant
- Tested too early. This is the most common reason. The day of your missed period is the earliest most home tests can detect pregnancy reliably, and even then, sensitivity varies by brand.
- Diluted urine. First-morning urine has the highest hCG concentration. Drinking a lot of water before testing can dilute the result.
- Test instructions not followed exactly. Reading the result outside the time window, not waiting long enough, or contaminating the test can produce false negatives.
- Irregular ovulation. If you ovulated late in your cycle, you’re not as far along as your calendar suggests, and your hCG may not have built up yet.
- Test sensitivity. Some over-the-counter tests detect pregnancy at 25 mIU/mL of hCG; others require 50 mIU/mL. The lower the number, the earlier the test can detect.
Retest schedule
| Where you are | What to do |
|---|---|
| 1–2 days late, negative test | Repeat in 3–4 days with first-morning urine |
| 1 week late, negative test | Repeat with first-morning urine, or ask your prescriber for a blood test |
| 2 weeks late, negative test | Get a quantitative blood test — these can detect pregnancy at very low hCG levels |
| 4+ weeks late, multiple negatives | Contact your prescriber or OB-GYN. Even if pregnancy is unlikely, this needs evaluation |
| 3 months late, multiple negatives | Medical evaluation is needed regardless of pregnancy possibility |
What if the cause isn’t pregnancy?
After pregnancy is reliably ruled out, the most common reasons for a missed period on a GLP-1 are the indirect mechanisms we’ve already covered: rapid weight loss, low food intake, stress, PCOS adjustments, thyroid issues, perimenopause (the years before menopause), or other unrelated medical conditions.
Cleveland Clinic identifies pregnancy, breastfeeding, hormonal birth control, perimenopause, low body weight, weight gain, stress, PCOS, thyroid disorders, and primary ovarian insufficiency as common causes of missed periods. Notice what’s not on that list: GLP-1 medications. If your provider tells you “it’s just the medication” without ruling these out, that’s worth a second opinion.
How long can a missed period last on a GLP-1?
Short answer: A single late or missed period is almost always temporary. Two missed cycles in a row is worth bringing up with your prescriber. Three or more missed periods in a row — what doctors call secondary amenorrhea — should be evaluated regardless of whether you’re on a GLP-1 or not. Some cycle changes settle as your weight, dose, intake, and stress stabilize; if you go three months without a period, get evaluated.
Here’s the timeline most clinicians use:
One missed period: Common. Many women experience this at some point in their lives unrelated to medication. If pregnancy is ruled out, track and watch.
Two missed periods: Worth a conversation with your prescriber. Especially if your cycles were previously regular and the change started after you began or increased a GLP-1. Bring your medication name, dose, start date, weight loss, and other tracked details to the conversation.
Three or more missed periods: Medical evaluation. Cleveland Clinic, Mayo Clinic, the Office on Women’s Health, and the National Institute of Child Health and Human Development (NICHD) all identify three months without a period as the threshold for evaluation. Workup typically includes pregnancy testing, thyroid function (TSH), prolactin, FSH, LH, and androgen levels depending on the clinical picture.
The good news for most women on GLP-1s: when cycle changes are tied to the indirect mechanisms we’ve covered (rapid weight loss, low intake, stress, dose changes), they often settle as those underlying factors stabilize. Your prescriber is the right partner for figuring out which cause applies to you.
What to track before you message your prescriber
Short answer: Bring specific data, not vague concerns. Track your last period date, your usual cycle length, current cycle day, pregnancy test dates and results, GLP-1 medication name and dose, start date, last dose increase date, weight change, eating patterns, and any concerning symptoms. This is what your prescriber needs to give you a real answer instead of a generic “let’s wait and see.”
The tracking checklist
Print this, screenshot it, or type it into a note. Bring it to your provider conversation:
- Date of your last menstrual period (first day of bleeding)
- Your usual cycle length (e.g., 28 days, 30 days, irregular)
- Current cycle day (how many days since your last period started)
- Days late
- Pregnancy test date(s) and result(s)
- Your GLP-1 medication name (Ozempic, Wegovy, Mounjaro, Zepbound, Foundayo, compounded semaglutide, compounded tirzepatide, etc.)
- Current dose
- Date you started the medication
- Date of your most recent dose increase
- Any missed doses in the past month
- Any vomiting or severe diarrhea after taking your birth-control pill
- Weight change in the past 30 days (in pounds)
- Total weight loss since starting the medication
- Appetite and food intake changes (eating much less? specific times you’ve been unable to eat?)
- Any nausea or vomiting that may have caused you to lose a pill or dose
- Exercise changes
- Stress, travel, or illness in the past month
- Birth control method, if any
- Any history of PCOS, thyroid problems, or irregular cycles before this
- Any new symptoms (severe pain, unusual bleeding, mood changes, hot flashes, hair changes)
The copy-paste prescriber message
Use this template if you’re not sure what to write:
Hi — I’m taking [medication] at [dose]. My last period started on [date], my usual cycle is [X] days, and I’m now [X] days late. I took a pregnancy test on [date] and the result was [positive/negative/unclear]. I [use / don’t use] [birth control method], and I started or increased my dose on [date]. In the past 30 days I’ve lost [X] pounds and have been [eating less than usual / occasional nausea / specific symptoms]. I’d like to know whether I should: (1) take or repeat a pregnancy test, (2) get bloodwork, (3) adjust my contraception, (4) pause or adjust my medication, or (5) something else. What do you recommend?
This message takes 90 seconds to fill out and gives your prescriber every piece of information they’d otherwise spend an appointment trying to extract.
If your current prescriber doesn’t respond to messages like this in a reasonable window, that’s a meaningful gap. Especially while you’re trying to figure out something potentially important about your reproductive health.
Should I stop my GLP-1 if my period is late?
Short answer: Don’t stop, restart, skip, or adjust your GLP-1 dose based on a late period alone without talking to your prescriber. If your pregnancy test is positive, contact your prescriber or OB-GYN today before taking another dose. If the test is negative and you have no concerning symptoms, continue as prescribed and bring the missed period up at your next check-in. The right decision depends on your medication, your test result, your symptoms, and your medical history — not on a website.
Here’s where we’re going to do something most affiliate sites won’t do: tell you what we can’t tell you.
We can’t tell you whether your specific next dose is safe. That decision depends on your medication, your pregnancy status, your symptoms, your medical history, and your prescriber’s clinical judgment. A website that pretends to make that call for you is selling something more than information.
What we can do is give you the cleanest order of operations and the exact information your prescriber will need:
- Take a pregnancy test if there’s any chance of pregnancy.
- Note your medication name, dose, and recent dose changes.
- Track the symptoms and timing details listed above.
- Use the copy-paste message above to message your prescriber.
- If you can’t reach your prescriber within 24 hours and pregnancy is positive, contact an OB-GYN, urgent care, or your primary care doctor.
That’s the right answer. Anyone who tells you “you can definitely keep taking it” or “you should definitely stop” without seeing you, your test result, and your medical history is guessing.
If your prescriber isn’t reachable when you have questions like this, that’s a real problem — and it’s worth solving before your next refill.
When to consider switching GLP-1 providers
Short answer: If your current GLP-1 provider isn’t responsive when you have urgent questions about pregnancy, contraception, or symptoms, that’s a meaningful gap. The right provider should respond to medical messages quickly, give clear contraception guidance with tirzepatide or orforglipron, and adjust your treatment plan if you’re losing weight too fast or experiencing concerning symptoms. Several telehealth providers publish 24/7 messaging or fast-response support, but you should verify response times, pregnancy protocols, contraception guidance, and pause or cancellation policies before switching.
We’re not going to push you into a comparison table here. This is a health-anxiety page, not a shopping page. But if you’ve gotten this far and one of the things keeping you up tonight is that your current provider isn’t supporting you well, here’s a brief honest take.
Affiliate disclosure: We may earn a commission if you sign up through our matching quiz or links to the providers below. Compensation does not affect medical eligibility, prescribing, or our editorial framing. Verify current pricing and policies on each provider’s site before enrolling.
What good provider support looks like for this specific situation
- Fast secure messaging response times. When you need to ask “do I need to switch contraception?” you shouldn’t wait a week.
- Clinicians comfortable answering contraception questions confidently. Not every GLP-1 telehealth provider has a clinician who handles this well.
- Clear pregnancy and contraception protocols built into onboarding. A provider who never asked you about contraception or pregnancy plans is not the right provider for someone on tirzepatide or orforglipron.
- A pause or adjustment process that doesn’t lock you in. If you become pregnant or need to step away, the provider should make that easy.
Three providers we’ve reviewed that meet the basics
We’re naming these as factual examples, not paid placements. Each one is a different fit:
- MEDVi — broad menu (compounded GLP-1 injections starting from $179 month one and tablets from $249, plus newer branded paths), 24/7 support included, no insurance required. Strong default for most women on a compounded GLP-1 who want a deep medication menu and around-the-clock support access. Verify current pricing and program terms at sign-up.
- Eden — flat-rate pricing structure where Eden’s official semaglutide page states the program fee stays consistent when your provider adjusts your dose ($149 first month, $249/month ongoing), with both compounded and brand-name medication paths available. Strong if you want predictable monthly cost and broad medication access.
- Ro — strongest FDA-approved option, particularly for women who want brand-name medication or insurance coverage. Ro’s published cash-pay GLP-1 list includes Foundayo, Wegovy pill, Wegovy pen, Zepbound pen, and Zepbound KwikPen, matches LillyDirect / NovoCare / TrumpRx pricing on medication, and includes a dedicated insurance concierge plus a free GLP-1 Insurance Coverage Checker. Ro Body Program membership is $39 for the first month, then $149/month — or as low as $74/month with annual prepay. Medication cost is separate from membership and varies by product and dose.
If you’re in the middle of a panic about a late period, please don’t switch providers tonight. Handle the safety steps first — pregnancy test, prescriber message, urgent care if symptoms warrant it. Switching providers is a longer-term decision worth making calmly when you have time.
Find a GLP-1 path that fits your situation
Take our free 60-second matching quiz. We’ll match you to a GLP-1 telehealth provider whose support model, pricing, medication options, and contraception-comfortable clinicians fit what you actually need.
Take the matching quiz →A note on what most other pages get wrong
Here’s our one honest negative, said plainly: we don’t have access to a clinical trial that tested every GLP-1 medication’s effect on every birth control method in every type of woman. Nobody does. That research mostly hasn’t been done at the scale women deserve, and the FDA labels reflect that — they err on the side of caution where the data is incomplete.
What that means for you: there’s a small but real chance that future studies will reveal something we don’t know yet about how these medications interact with reproductive hormones. We’ve shown you what the current evidence supports — semaglutide doesn’t appear to delay birth control absorption in a clinically meaningful way; tirzepatide and orforglipron do, with FDA-labeled windows; weight loss can pause cycles; restored fertility is real. We’ve cited primary sources for each claim. We’ll update this page when better data comes out.
That uncertainty is also why your prescriber matters more than this page does. The best information always comes from someone who can actually examine you and review your full history.
GLP-1 missed period FAQ
Can a GLP-1 directly cause a missed period?
Not directly. GLP-1 medications don't act on reproductive hormones, and missed period or amenorrhea isn't listed as a named adverse reaction on the FDA labels we reviewed for Ozempic, Wegovy, Rybelsus, Mounjaro, Zepbound, or Foundayo. Cycle changes that women report on GLP-1s are almost always indirect — driven by weight loss, insulin sensitivity shifts, or, with tirzepatide and orforglipron, reduced absorption of oral birth control.
Can you get pregnant on Ozempic, Wegovy, Mounjaro, Zepbound, or Foundayo?
Yes. GLP-1s are not contraceptives. They can also indirectly increase the chance of pregnancy by improving insulin sensitivity and restoring ovulation, particularly in women with PCOS. Tirzepatide (Mounjaro, Zepbound) and orforglipron (Foundayo) can reduce oral birth control absorption per FDA labeling. If you don't want to be pregnant, talk to your prescriber about non-oral or barrier contraception during the labeled windows.
How long does it take for periods to return to normal on a GLP-1?
It varies. When the cause is indirect (weight loss, low intake, stress), cycles often settle as those underlying factors stabilize. Cleveland Clinic's window for hypothalamic amenorrhea is 3–6 months once the underlying issue is treated consistently. If you go three months without a period, get evaluated regardless of cause.
Does Ozempic affect birth control?
Ozempic and Wegovy (both semaglutide) don't have an FDA contraceptive interaction warning. The 2024 systematic review by Skelley and colleagues, plus FSRH guidance, concluded semaglutide doesn't reduce oral contraceptive absorption in a clinically meaningful way. Mounjaro and Zepbound (tirzepatide) and Foundayo (orforglipron) do — they have specific FDA warnings about oral contraceptive effectiveness.
What if I vomited or had diarrhea after taking my birth control pill?
Treat it as a missed pill. Vomiting within about two hours of taking a combined oral contraceptive — or severe diarrhea — can prevent absorption. Follow your pill packet's missed-pill rules, add a barrier method for at least 7 days, and message your prescriber if it's happening repeatedly on a GLP-1.
Should I stop my GLP-1 if my period is late?
Don't stop without talking to your prescriber. If you've taken a pregnancy test and it's positive, contact your prescriber today before taking another dose. If the test is negative and there's no other concerning symptom, continue as prescribed and bring up the missed period at your next check-in.
How long after stopping a GLP-1 can I try to get pregnant?
Per FDA labeling, semaglutide (Ozempic, Rybelsus) recommends stopping at least 2 months before a planned pregnancy. Tirzepatide (Mounjaro, Zepbound): MotherToBaby reports it can take, on average, up to 30 days for most tirzepatide to be cleared — your prescriber can give pre-conception timing for your specific situation. Foundayo guidance is to discontinue when pregnancy is recognized; pre-conception planning should be discussed with your prescriber.
I have PCOS. Why is my period suddenly missing on a GLP-1?
For some women with PCOS on a GLP-1, cycles become more regular, not less — and that's worth knowing. If your previously irregular cycles got regular and then your last period didn't come, take a pregnancy test (restored fertility is real on GLP-1s) and contact your prescriber if the test is negative.
Can missing GLP-1 doses affect my period?
Missing doses can disrupt your medication routine, but it doesn't prove that's why your period is late. Use the same sequence: pregnancy test first, check your symptoms, track your dose dates, and message your prescriber if pregnancy is possible or your period stays missing.
Is heavy bleeding a side effect of GLP-1s?
Heavy bleeding isn’t listed as a named adverse reaction on the FDA labels we reviewed. Some women report heavier periods anecdotally; others report lighter ones. Heavy bleeding alongside severe pain or bleeding longer than 7 days warrants medical evaluation.
Can a GLP-1 cause a false negative pregnancy test?
Most medications, including GLP-1s, don't affect home pregnancy test results. False negatives are usually caused by testing too early, diluted urine, or test-use issues. Repeat the test or ask about a blood test if pregnancy is still possible.
Is this perimenopause or the GLP-1?
It could be either, or neither. Age, cycle history, symptoms, medication changes, pregnancy possibility, thyroid function, and weight loss speed all matter. If you're in your 40s and noticing both cycle changes and other perimenopause symptoms (hot flashes, sleep changes, mood shifts), bring it up with your prescriber or OB-GYN.
Should I report menstrual changes to my GLP-1 prescriber?
Yes. Tell your prescriber if your period is late, missing, unusually heavy, painful, or repeatedly irregular — especially after a dose change or if pregnancy is possible.
Will my period stop forever if I stay on a GLP-1?
No evidence we reviewed for this page supports permanent period cessation from GLP-1s. Persistent absence of periods for three or more consecutive months should be evaluated.
Are "Ozempic babies" real?
Unexpected pregnancies on GLP-1s are widely reported, and the mechanisms are clinically plausible — restored ovulation after metabolic changes, plus the tirzepatide and orforglipron oral-contraceptive warnings. Human pregnancy-safety data for GLP-1s remain limited.
What we actually verified for this page
Sources reviewed: FDA prescribing information for Ozempic, Wegovy, Rybelsus, Mounjaro, Zepbound, and Foundayo via DailyMed and FDA.gov; the Skelley et al. 2024 systematic review summarized in National Geographic and Endocrinology Advisor; the FSRH (Faculty of Sexual & Reproductive Healthcare) guidance on oral contraceptive use with GLP-1 agonists; the Natural Cycles 2024 menstrual changes survey (n=1,754); Carmina et al. 2023 (semaglutide and PCOS, n=27); the Lin et al. 2025 GLP-1 receptor agonist meta-analysis in Scientific Reports; Cleveland Clinic, Mayo Clinic, Office on Women’s Health, and NICHD on amenorrhea and pregnancy testing; MotherToBaby fact sheets from OTIS; FDA safety communications on unapproved GLP-1 drugs and compounded GLP-1 dosing errors; the FDA’s April 30, 2026 proposed rule on the 503B bulks list.
What we did: Pulled the contraceptive guidance for each medication directly from current FDA labels rather than from competing affiliate sites. Cross-referenced provider claims against published pricing pages. Built the drug-by-drug comparison table from the actual prescribing information.
What we didn’t do: Interview patients, run a clinical trial, or invent a medical reviewer credential. This page is informational and is not medical advice. If you’re worried about a missed period, take a pregnancy test if there’s any chance of pregnancy, and contact your prescriber or OB-GYN for personal guidance.
Last verified: . We re-check FDA label language, pregnancy-test guidance, and provider information at least quarterly.
Bottom line
A GLP-1 missed period almost never means the medication directly stopped your cycle. Pregnancy is the first thing to rule out, and with two specific drugs — tirzepatide (Mounjaro, Zepbound) and orforglipron (Foundayo) — pregnancy is more relevant than usual because the FDA labels warn about reduced oral birth control absorption during specific windows. Semaglutide (Ozempic, Wegovy, Rybelsus) doesn’t carry the same warning. Rapid weight loss can pause your cycle through hypothalamic amenorrhea. PCOS often improves on a GLP-1, which can also restore fertility unexpectedly. Most cycle changes settle as your weight, dose, intake, and stress stabilize. Three or more missed periods warrants medical evaluation regardless of cause.
If you’re scared right now: test, message your prescriber with the template above, and if your symptoms are urgent, go to urgent care today. You’re not alone in this — 27% of women on GLP-1s notice cycle changes, and most resolve without anything bad happening. The page you’re reading exists because we believed you deserved a clearer answer than the one you were getting.
Still not sure which GLP-1 program is right for you, or which contraceptive setup fits your situation?
Take our free 60-second matching quiz
We’ll match you to a GLP-1 telehealth provider whose support model, pricing, and medication options fit what you actually need. Just a personalized plan you can use to make a confident decision.
Take the matching quiz →Weight Loss Provider Guide is an independent comparison resource for GLP-1 telehealth providers. We may earn a commission if you sign up through our matching quiz, at no extra cost to you. Compounded medications discussed on this page are not FDA-approved as finished products. This page is for informational purposes only and is not medical advice. Always consult a licensed healthcare provider for guidance specific to your situation.
Last verified: · By the WPG Editorial Team